MRI is assuming increasing importance in helping doctors decide if the patient is fit to undergo surgery or not.
MRI is assuming increasing importance in helping doctors decide if the patient is fit to undergo surgery or not.
The patient described in this paper, Amanda Mayer, age four, of Staten Island, N.Y., had previously undergone all three stages of the Fontan procedure at The Children's Hospital of Philadelphia, but developed severe complications. Her oxygen saturation was very low – only 72 percent, compared to normal levels of at least 95 percent – which indicated the possibility of abnormal connections between the veins and arteries in one of her lungs. Normally, the liver releases hormonal factors that prevent these abnormal connections, so the presence of the malformations indicated a low supply of hepatic blood to the lung.To improve the distribution of these hormonal factors to both lungs, the surgeons needed to re-operate and reconfigure the patient's cardiovascular anatomy. Georgia Tech's surgical planning framework helped Thomas L. Spray, M.D., chief of the Division of Cardiothoracic Surgery at Children's Hospital, to determine the optimal surgical option.
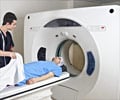
"MRI acquires images of the child's heart without using radiation," said Spray. "Then we use the computerized technology to model different connections to simulate optimum blood flow characteristics, before we perform the surgery."
The image-based surgical planning consisted of five major steps: acquiring magnetic resonance images of the child's heart at different times in the cardiac cycle, modeling the preoperative heart anatomy and blood flow, performing virtual surgeries, using computational fluid dynamics to model the proposed postoperative flow, and measuring the distribution of liver-derived hormonal factors and other clinically relevant parameters as feedback to the surgeon.
Fogel collected three different types of magnetic resonance images, and Yoganathan, along with graduate students Kartik Sundareswaran and Diane de Zélicourt, generated a three-dimensional model of the child's cardiovascular anatomy. From the model they reconstructed the three-dimensional pre-operative flow fields to understand the underlying causes of the malformations.
For this particular patient, the team saw a highly uneven flow distribution – the left lung was receiving about 70 percent of the blood pumped out by the heart, but only five percent of the hepatic blood. Both observations suggested left lung malformations, but closer examination of the flow structures in that particular patient revealed that the competition between different vessels at the center of the original Fontan connection effectively forced all hepatic factors into the right lung even though a vast majority of total cardiac output went to the left lung.
RAS/L
 MEDINDIA
MEDINDIA


 Email
Email










