Researchers from the University of Colorado say that death rates from pulmonary fibrosis have increased significantly in recent years, with no signs of slowing down.
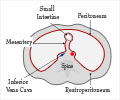
During 1992 and 2003, the age-adjusted mortality rate from PF (an often fatal disease which involves scarring of the lung ) rose by nearly 28.4 percent in men, and 41.3 percent in women. Over the same time period, an increasing percentage of patients with PF died of the disease itself rather than of coexisting conditions.“Rates rise with increasing age, are highest among older people, and are consistently higher in men than in women,” wrote the researchers. “However, mortality rates in women with PF are climbing more rapidly than in men.”
The study, led by Amy Olsen, M.D., M.S.P.H., of the University of Colorado Health Sciences Center, appears in the August 1, 2007, issue to the American Journal of Respiratory and Critical Care Medicine, published by the American Thoracic Society.
Dr. Olson and five colleagues analyzed the cause of death listed on death certificates for more than 28 million decedents using data compiled by the National Center for Health Statistics. Of that larger group, more than 175,000 deaths were linked to PF.
In developing a model to predict future mortality rates, the researchers applied a multivariable analysis to current data, finding a predicted significant increase in men over the age of 65 and for women in all age categories.
“Our study is the first large-scale study to examine age-, sex-, race-, and ethnicity-stratified mortality rates in decedents with PF,” said Dr. Olson.
Advertisement
Although previous studies have suggested that whites are more likely to be diagnosed with PF, differences in race or ethnicity “may also play a role in susceptibility,” the researchers note, and merit further examination.
Advertisement
“Although we were unable to determine the underlying cause of the geographic variation using this dataset, these differences warrant further exploration,” Dr. Olson said.
Similarly, the researchers were unable to determine whether the increased percentage of patients with PF dying from the disease itself represents an improvement in treatments for commonly co-existing conditions such as cardiovascular disease, reflects diagnostic changes, or the result of a new classification system implemented in 1997 that excludes patients with more hopeful prognoses.
“Although once considered an orphan disease, our results suggest that PF should no longer be considered a rarity,” Dr. Olson concluded, noting that current death rates for the disease are higher than multiple myeloma and bladder cancer “These findings indicate an important and growing problem and provide an argument for more resources focused on the pathobiology of and therapy for this disease.”
Source-Eurekalert
LIN/B