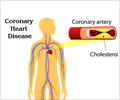
More people who have known coronary heart disease die from other causes — such as cancer, and lung and neurological diseases — than heart disease, compared with 20 years ago.

The researchers evaluated the trends in cause-specific, long-term mortality from 1991 to 2008 in patients at Mayo Clinic in Rochester who underwent percutaneous coronary intervention (PCI), a procedure used to open clogged heart arteries. They broke the study population into three eras: 1991 to 1996, 1997 to 2002, and 2003 to 2008. Cardiac deaths predominated in the first era and were about equal with non-cardiac deaths in the middle era. In the final era — the modern-era (2003 to 2008) — non-cardiac deaths dominated.
Approximately 20,000 PCI patients were studied. Of those, nearly 7,000 patients died within the study time frame. Among that group, only 37 percent of deaths in the modern-era (2003-2008) were cardiac-related.
"We found that patients with established heart disease undergoing angioplasty and stenting in the modern era have about a 1 in 3 chance of dying from their heart disease, and a 2 in 3 chance of dying from non-cardiac diseases in the long term," says Rajiv Gulati, M.D., Ph.D., senior author and Mayo Clinic interventional cardiologist.
The results surprised the authors, Dr. Gulati says. First, patients undergoing angioplasty in the modern era have gotten older, with more complex coronary disease and more risk factors compared with years ago. So, the authors were expecting their cardiac death rates to have increased. "In addition, in randomized clinical trials of PCI, deaths from cardiac disease still predominate," he says. The authors believe the sharp decline in long-term cardiac deaths in these patients may result from improved cardiac therapies. For example, more patients today with established heart disease take medications to lower cholesterol, prevent heart failure, and decrease blood pressure, and technologies used in catheterization laboratories — where PCI is performed — have improved, Dr. Gulati says.
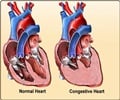
Of the cardiac-specific deaths, deaths from heart attack and sudden heart rhythm disturbances declined steeply, but there was no decline in deaths from heart failure.
Source-Eurekalert
 MEDINDIA
MEDINDIA



 Email
Email