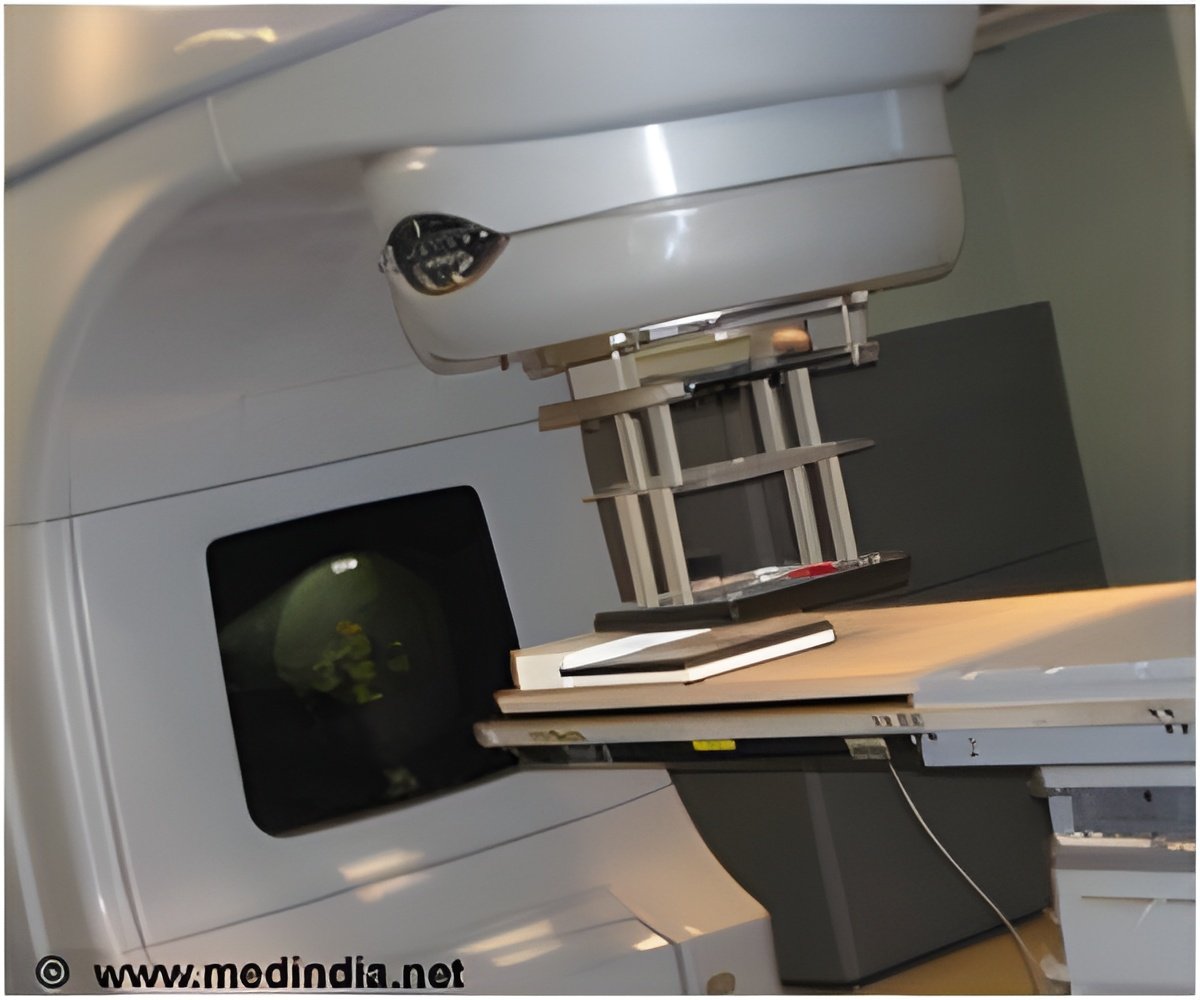
Radiation therapy is used to treat cancerous tumors in the brain and elsewhere in the body because of its ability to control cell growth.
TOP INSIGHT
Radiation works by damaging the DNA of cancerous tissue, a process that ultimately leads to cellular death. Rapidly dividing cancer cells are particularly vulnerable to radiation therapy
In order to spare the normal healthy tissue that the radiation beam passes through on its way to treat the tumor, physicians use shaped radiation beams that are aimed from several different angles and intersect at the tumor. This approach delivers the highest dose to the tumor while limiting radiation exposure to other cells.
The radiation is also typically delivered in a series of modest doses - a process called fractionation - over a period of several weeks or months, an approach that is believed to be more effective in sparing healthy cells from damage than applying the radiation in a single large dose.
While many of the cells found in the adult brain, most notably neurons, do not have the capacity to self-renew, the brain is also home to a population of cells that continue to divide and grow. Specifically a cell called the oligodendrocyte progenitor (OPC), which is responsible for producing myelin, the fatty tissue that insulates the connections between nerve cells and is critical for the conduction of signals between cells in the central nervous system. Because these cells continue to divide, even in the adult brain, OPCs are susceptible to the same mechanism that radiation employs to kill cancer cells.
The researchers conducted a series of experiments in mice. The animals received modest doses of radiation in their brains over a period of time. The researchers observed that the initial doses of radiation killed off some of the OPCs. However, when this occurred, the surviving OPCs became more active, essentially trying to make up for the loss of the other cells. This in turn made the remaining OPC cells even more vulnerable to subsequent doses of radiation, killing them off in larger numbers.
"This study indicates that single dose and fractionation radiation protocols elicited similar degrees of normal tissue damage, suggesting that conventional fractionation regimens do not spare the brain from sustained OPC depletion, reduced myelination, or alterations in signal conduction," said Jacqueline Williams, Ph.D., a professor of Environmental Medicine and Radiation Oncology at the URMC Wilmot Cancer Institute and co-author of the study. "These studies indicate that reducing the volume of the brain exposed to radiation is necessary to minimize white matter damage and the need to potentially revisit protocols for delivering radiation therapy in the brain."
 MEDINDIA
MEDINDIA



 Email
Email










