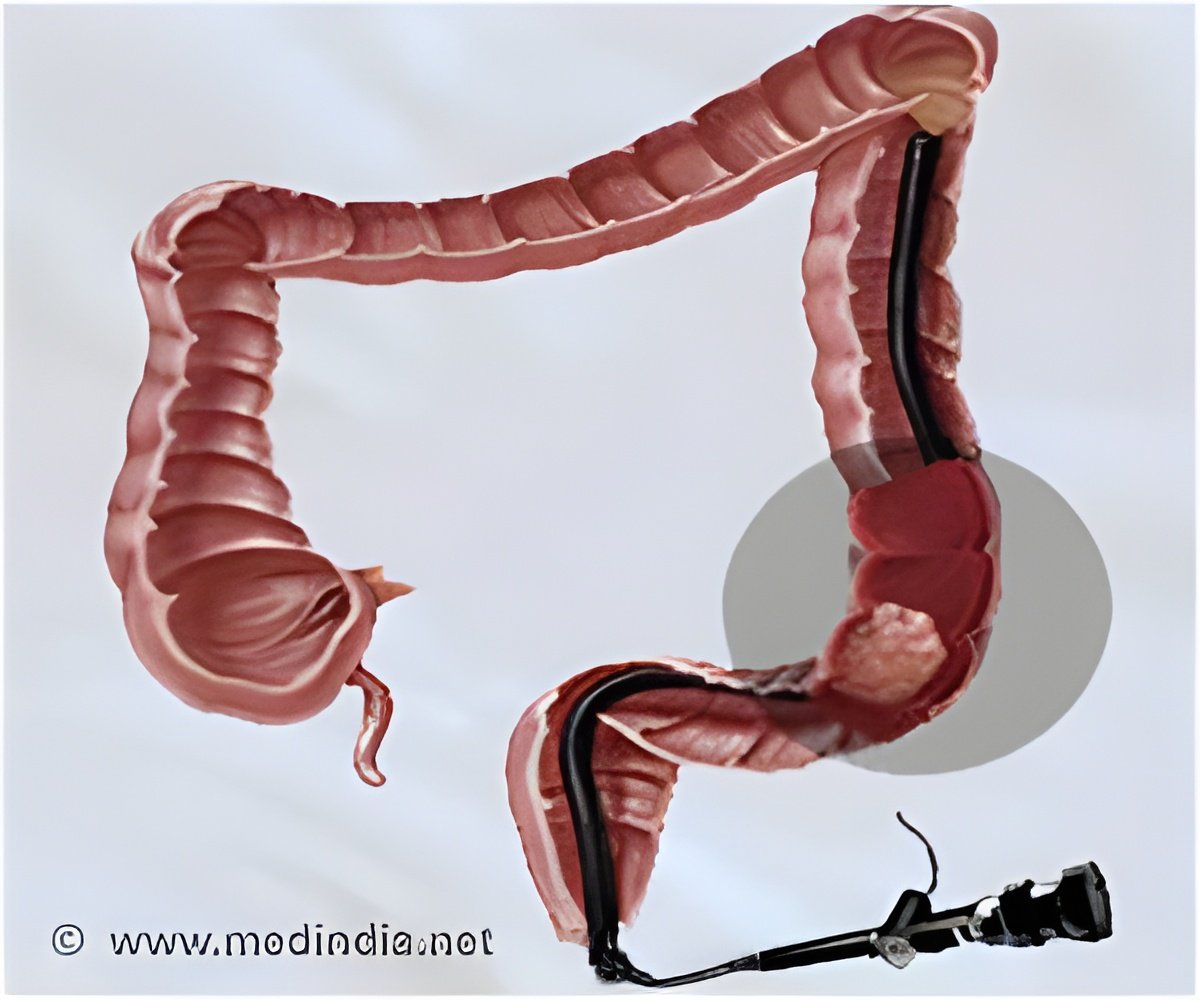
New research indicates that regular primary care visits lower colorectal cancer incidence, death, and all-cause mortality.
Note: For an embargoed PDF, please contact Megan Hanks or Angela Collom. The lead author can be reached through Jennifer Forbes at [email protected] or 732-235-6356.
2. Patient outcomes are not affected by early discharge from busy ICUs
Doctors in strained ICUs are more likely to make high-value care decisions
Physicians in resource-strained intensive care units (ICUs) are likely to discharge patients more efficiently without negatively affecting outcomes. Health care costs in the U.S. are likely to increase strain on ICU resources. Strain on ICU capacity may influence care providers to discharge patients as soon as possible to open beds, and communication may suffer during patient handoffs. Researchers reviewed heath records for 200,730 adults discharged from 155 ICUs in the U.S. to determine how ICU capacity strain on day of patient discharge affects ICU length-of-stay and post-ICU discharge outcomes. ICU capacity was measured by ICU census, number of new admissions, and average number of patients. The researchers found that when ICUs were busy, patients stayed for a shorter time and were somewhat more likely to be readmitted to the ICU. However, there were no increases in patient mortality rates, no greater overall length of hospital stay, and no greater rate of hospital readmission within 30 days of hospital discharge. The authors suggest that physicians are more likely to practice high-value care, efficiently discharging those patients who do not actually require ICU treatment.
Note: For an embargoed PDF, please contact Megan Hanks or Angela Collom. Lead author Dr. Jason Wagner can be contacted through [email protected] or 215-349-5653.
3. Medicare Advantage plans underreport high-risk prescribing practices
Under the Patient Protection and Affordable Care Act, the Centers for Medicare & Medicaid Services (CMS) are required to publicly report quality and performance measures so that providers and patients are fully informed about cost and quality of care. However, the accuracy of these reports is not known. Medicare Advantage plans report clinical performance using Healthcare Effectiveness Data Information Set (HEDIS) quality indicators. Researchers reviewed 172 Medicare Advantage Plans to compare reported HEDIS rates of high-risk prescribing (prescribing drugs that should be avoided in elderly patients) to rates calculated using Medicare Part D claims. They found that, on average, plans underreported high-risk prescribing by 5.8 percentage points. When ranking plans according to their calculated versus reported performance, plans with the most accurate reporting had the greatest penalty and those with the least accurate reporting had the greatest gain. The researchers also found that the rate of high-risk prescribing was the same for Medicare Advantage and Medicare fee-for-service beneficiaries. However, policymakers evaluating plan-reported rates would erroneously conclude that Medicare Advantage program has relative rates of high-risk prescribing that are approximately 20 percent lower than fee-for-service. This analysis suggests that reported performance measures should be regularly audited to ensure accuracy.
Source-Eurekalert
 MEDINDIA
MEDINDIA
 Email
Email










