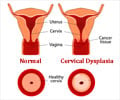
Scientific breakthrough regarding where and how cervical cancer takes origin in the body has settled a decades-long mystery and may well lead to even better prevention in the future, posit experts.

But apparently as early as the 1920s, doctors in Boston, Massachusetts discovered a related phenomenon that arose from a common practice of cauterizing the cervix, or burning off any abnormal cells, after childbirth.
Back then, they noted that women who underwent the procedure almost never developed cervical cancer, but they were not sure why.
Now, doctors believe it was because they were burning off a population of host cells which cannot regenerate.
And the finding has made some consider whether the technique should be revived to help in parts of the developing world where cervical cancer remains a widespread killer of women.
Nearly 530,000 women are diagnosed with cervical cancer annually worldwide and 275,000 die from the disease, according to the World Health Organization.
But back then, the unusual absence of cancer among a certain group of American women drew the attention of doctors.
In the article, Younge recalled learning of the technique from a colleague, Paul Gustafson, who "began routine postpartum cauterization of the cervix over 30 years ago," and who told him shortly before dying that he had performed the procedure on more than 6,000 women.
Younge said only one of those patients in the Boston area had ever developed a cervical lesion, and urged all physicians to routinely cauterize the cervix after childbirth in case abnormalities were observed.
Younge and his colleague Albert Kevorkian performed the procedure for years until they retired from the Free Hospital, which has now become known as Brigham and Women's Hospital, said Ralph Richart, who worked with them in 1960 when he was a fellow at Harvard University. Both men are now deceased.
"Everybody puzzled over this," Richart, 78, a professor emeritus at Columbia University, told AFP. "We speculated that you were treating by virtue of doing the cautery."
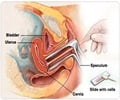
The technique involved peering at the cervix with a microscope-like instrument and delivering an electrical current through a medical wand to burn off the cells.
Patients were awake for the procedure and were not typically given narcotics to numb the pain.
"Women would describe it like bad menstrual cramps," he said.
Years later, Richart told Christopher Crum, who was working under him as a fellow at Columbia University, about the Boston doctors' findings and the hints they left toward a potential preventive technique against cervical cancer.
Now Crum, who worked with colleagues from Harvard Medical School and the Agency for Science Technology and Research (A-STAR) in Singapore on the latest study, finally has some evidence for the phenomenon.
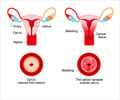
The cells where cancer takes root are usually located near the opening of the cervix, in a transition area between the vagina and uterus known as the squamo-columnar junction.
These cells appear to be remnants of the cell division and growth that occurs in the transition from embryo to fetus, called embryogenesis.
A similar population of cells has previously been found in the esophagus, in a transition area between the stomach and the throat.
The team described its findings in the Proceedings of the National Academy of Sciences.
Crum, now director of the division of women's and perinatal pathology at Brigham and Women's Hospital, sent his mentor a preprint of the article.
"I said, 'Whoa! You have solved a 60-year-old mystery!'" recalled Richart. "I am an old guy and there are not many people left who remember those observations."
Researchers hope further study will reveal if such cells are linked to other HPV cancers, such as those that affect the anus and the throat.
The findings could also benefit places like south Asia and sub-Saharan Africa, where women may not have the opportunity for regular screenings or vaccines to prevent cervical cancer, but may be able to undergo a brief cryo-probe procedure that would freeze off the cells, Crum said.
Richart agreed that the technique may be due for an update and a revival.
"It may be possible to fashion clinical interventions which will take care of that in countries which can't afford screening," Richart said.
"The more we know, the more likely we are to be able to utilize it for the benefit of women."
Source-AFP
 MEDINDIA
MEDINDIA

 Email
Email