Johns Hopkins researchers have found that dense mats of interacting bacteria, called biofilms, were present in the majority of cancers and polyps, particularly those on the right side of the colon.
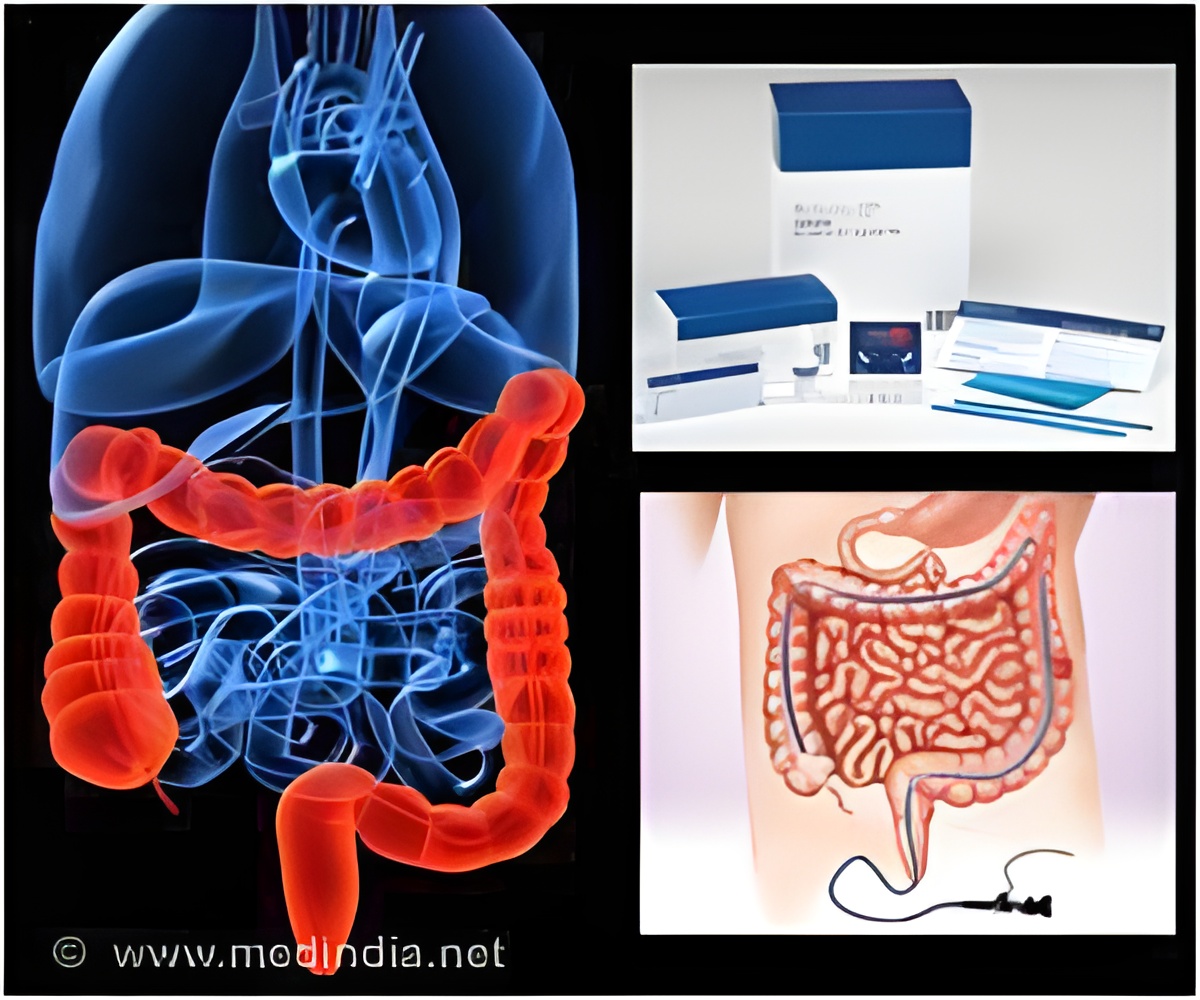
Like tooth plaque and slime on pond stones, bacterial biofilms may coat the mucus layer of cells lining the colon, causing inflammation and some noncancerous bowel diseases. The bacteria "invade the layer of mucus that protects epithelial cells in these areas and upend the whole biology of the system," says Cynthia L. Sears, M.D., professor of medicine and oncology at the Johns Hopkins University School of Medicine and Bloomberg School of Public Health.
In an examination of healthy and cancerous tissue biopsied from 118 people undergoing surgery or colonoscopy at The Johns Hopkins Hospital or at the University of Malaya Medical Centre in Malaysia, Sears and her colleagues found that biofilms were present on 89 percent of tumors - 13 of 15 cancers and four of four polyps - removed from the right or ascending colon.
By contrast, biofilms, for reasons not known, were found only 12 percent of the time on tumors on the left side of the colon - two of 15 cancers and no polyps.
Overall, the researchers say, their data suggest the risk of developing colorectal cancer might be fivefold higher in patients with biofilms on the right side of the colon, compared to patients without the bacterial mats. Results of their work were published online Dec. 8 in the Proceedings of the National Academy of Sciences.
"What was so striking was that these biofilm-positive samples cluster so dramatically in the right colon," says Sears. "In fact, it's virtually a universal feature of tumors that appear in that section of the colon, although we don't understand why."
Colonoscopies currently are the gold standard in detecting colorectal cancer, but only approximately 60 percent of people in the U.S. get them. At the same time, colonoscopies are less frequently performed outside the U.S., especially in low-resource countries, where colorectal cancers are on the rise, Sears says. "We have an obligation to find better ways to diagnose this, because colonoscopies will not be done routinely in other parts of the world, and we need better tools to help prevent disease."
The researchers also identified the types of bacteria found in the colon tissues through genetic sequencing. They found that the same species of bacteria were present in tumors from people with and without biofilms. This suggests that the biofilm itself, rather than a particular kind of bacteria, may be the cancer-causing trigger, adds Sears, a member of the Johns Hopkins Kimmel Cancer Center.
Sears' earlier research looked at the role of bacteria and diarrheal disease, "but over time we recognized that our bacteria triggered changes in cells that were consistent with the ability to induce tumors," she says. "And we wondered whether colonization with these organisms might be a long-term trigger for colon cancer."
The researchers plan to examine biofilms in subjects over at least five years, Sears says, "to see if we can understand the dynamics of their formation, persistence and relationship to early cancer development."
Source-Eurekalert
 MEDINDIA
MEDINDIA

 Email
Email




