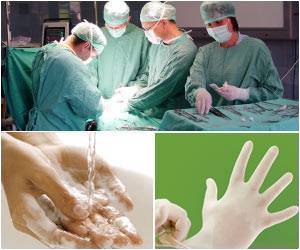
The hand-washing initiative promoted the 'five moments of hand-hygiene' to highlight critical times for health workers to wash their hands to control infection.

TOP INSIGHT
Australia’s hand hygiene initiative that aimed to curb hospital-acquired infections was found to be effective, but the program was expensive costing around $2.9 million every year.
He said the National Hand Hygiene Initiative aimed to curb hospital-acquired infections and improve safety in hospitals.
"We know that healthcare costs are spiraling upwards and that we will never have enough money to fund all the prevention and treatment we would like," Professor Graves said.
"Health economists look at the cost-effectiveness, or value for money, of health interventions, to identify where health dollars are being used efficiently.
"An example is that we know pregnant women should not smoke, but spending millions of dollars trying to convince a small number of women to stop could be a waste of money.
"Similarly, the national hand hygiene program has to stack up when compared to another health program we might like to fund."
"Health economists use the concept of 'life years gained' to assess the health benefits of competing programs," Professor Graves said.
"We look for programs that provide extra years of life at the lowest cost, and we should pick the bargains first if we want to get the biggest bang for our health buck.
"The extra $2.9 million bought us only 96 years of life for the whole country; this is about $29,700 per life year gained.
"The cost-effectiveness of the initiative varied across the states. Queensland, for example, got better value for money where it cost only $8,988 per life year gained, because infection rates were higher and, therefore, the initiative was more effective.
"But in Western Australia, where infection risks were already very low there were no cases prevented yet almost $600,000 was spent for nothing.
"A similar story emerged for Tasmania where no cases were prevented, and $250,000 was spent. In the ACT where 10 cases were prevented it cost $1,030 per life year gained, and this was a true bargain.
"We can see that The National Hand Hygiene Initiative worked, but it was quite an expensive way to generate health benefits."
Professor Graves said other research that had evaluated a variety of interventions for prevention, screening, diagnosis, and treatment had shown life years could be gained for $18,720, and a large number of programs cost under $10,000 per life year.
"These findings suggest the National Hand Hygiene Initiative is effective but expensive. Policy makers could take note of the variability between states and tailor hand hygiene campaigns to the local conditions."
QUT is one of five Australian universities that have come together to form the Australian Technology Network of Universities (ATN).
The study is published in the journal PLOS One.
Source-Eurekalert
 MEDINDIA
MEDINDIA


 Email
Email




