- Clinical application of drug delivery systems in cancer chemotherapy: review of the efficacy and side effects of approved drugs - (http://www.ncbi.nlm.nih.gov/pubmed/23649331)
- Targeted drug delivery - (http://en.wikipedia.org/wiki/targeted_drug_delivery)
- Targeted Drug Delivery Systems Mediated by a Novel Peptide in Breast Cancer Therapy and Imaging - (http://www.plosone.org/article/info%3adoi%2f10.1371%2fjournal.pone.0066128)
- Targeted Cancer Therapies - (http://www.cancer.gov/cancertopics/factsheet/therapy/targeted)
What is Drug Delivery Systems?
Targeted drug delivery system delivers medication to the patient in a pre-specified way to a particular organ, tissue or cells within the body. Targeted drug delivery in oncology provides a localized and prolonged drug delivery to the affected organ or tissues. Various types of drug delivery systems are used based on the drug, route of administration, ease of consumption, combination of the drugs and the delivery systems, and other factors.
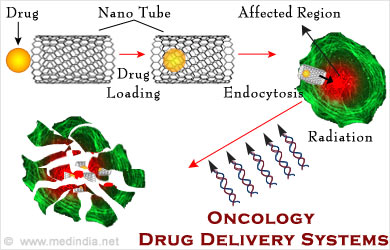
What is Oncology?
Oncology, the branch of science that deals with cancers, involves diagnosis, treatment, follow-up after treatment, palliative care of patients with terminal cancers and also screening for cancer among high-risk groups. A medical professional or expert in cancer is called an oncologist.
The diagnostic methods include biopsy, endoscopy, Single Photon Emission Computed Tomography, Positron Emission Tomography, CT and MRI scan, ultrasound and many others. Palliative care includes the various symptom management techniques, pain relief, activities, support and counseling given to the patient along with the family members who face problems coping with the life-threatening illness.
The treatment of cancer depends upto the stage to which the cancer has progressed. Surgery, chemotherapy and radiation therapy are the usual methods of treatment. Chemotherapy involves using the cancer drugs for treatment; these are administered through various routes.
Types of Drug Delivery Systems
The classification of the available drug delivery systems are based on various factors.
- Routes of drug delivery system: A drug can be delivered through various routes such as oral inhalation, sublingual, rectal or vaginal. Injections can be done through various routes like subcutaneous or intravenous route.
- The manner of drug release: Some drugs may be released over sustained periods of time throughout the body, while some drugs may have target sites where they are released. Pulsatile drug delivery system is the controlled release over intervals of time.
- Drug delivery vehicles: The physio-chemical properties of the drug, its solubility in water and various other factors determine the binding of the drug with the carrier. Vehicles of drug delivery system like liposomes, micelles and dendrimers, artificial DNA nanostructures and biodegradable particles also differ based on the drug to be delivered.
Drug Delivery System in Oncology
Targeting the delivery of drugs to tumors is a great advance in the field of oncology treatment. Various types, routes and vehicles of drug delivery to the site of the lesion are being researched. Current technologies are used to deliver drugs that are released for extended periods of time that can range from a few days to a few years.
- Certain oral and transdermal drug delivery systems can deliver drugs for 24 hours. They increase the efficacy of the drugs at the site of lesion and also minimize the side-effects.
- Implantable drug delivery systems are known to deliver drugs for longer periods of time like a few months to years.
- Passive targeting of drugs is based on drug accumulation in the areas around the tumors that have weak blood walls. Active targeting refers to specific interactions between drug or drug carriers and the target cells. They reach the target tissue via the blood circulation and absorbed into the circulation of the tumor.
Tumor Treatment with Drug Delivery Systems – Factors To Consider
Some factors that should be considered in treating tumors with drug delivery systems:
- EPR Effect: Enhanced permeation and retention effect refers to a leaky vascular structure and inefficient lymphatic drainage present at the tumor site. The weak structure of the blood vessels enhances the absorption of the drug or the carrier, thus improving the effect of treatment.
- Extravasation and Intratumoral distribution: After a drug carrier reaches its target cell, it needs to extravasate through the openings in the blood vessels and get into the tumor tissue. The flow is driven by the pressure gradient called interstitial fluid pressure. Once the drug carrier passes into the tumor, it has to distribute itself. The intratumoral distribution ability of the drug carrier has to be considered for the selection of the drug carrier.

- Tumor heterogeneity: The tumor itself is a mass or collection of several types of cells including cancer stem-like cells and other types of bulk cells, which can survive from standard cytotoxic treatments.
- Over-expression: Drug receptors (parts of the cells on which drugs act) are often overexpressed on the cancer cells. Thus, this is certainly a factor to be considered for target-specific delivery of drugs.
Drug Delivery Vehicles
Several drug delivery vehicles that show promise in oncology are:
- Biopolymers in oral or parenteral drug delivery: Chemotherapy drugs are traditionally administered by intravenous injection, orally, interstitial placement or by intratumoral injection. Polymeric materials that are used as binders to the drugs control the release of the active agent by diffusion, cleavage, dissolution or matrix erosion. Biopolymers are more popular vehicles of drug delivery due to low toxicity, biodegradability, stability and renewable nature. Some of the examples of the carriers include cellulose, starch, pectin, alginates and gums.
- Hydrogels DDS: Hydrogels are polymers that are highly water swollen, soft and elastic gel. This soft and rubbery surface, structure and physio-chemical properties of hydrogels are similar to that of human tissue and are most suited to serve as carriers in drug delivery systems. The drug release kinetics is manipulated by modifying the shape, size and drug distribution of the hydrogels. In spite of certain limitations, like risk of syringe clogging, sustained release of the drugs bound to hydrogels provides a great potential for a safe and effective vehicle for drugs.
- Polyethylene glycol conjugation of protein and small molecule drugs: Poly (ethylene glycol) or PEG is a compound composed of repeating ethylene glycol units. It is non-toxic, non-immunogenic, hydrophilic and highly flexible. It is also known to enhance the solubility of hydrophobic drugs and achieve the ability of targeting the specific tumor by increasing permeability and retention effect.
- Emulsions: An emulsion is a mixture of two or more liquids that are normally unblendable. It can be oil and water, thus improving the odds of using drugs that are soluble in different kinds of liquids. Anticancer agents are typically water repelling and unstable in water. Nanoemulsions, or droplets of the size 50 to 1000 nanometers, can dissolve large quantities of hydrophobic anticancer agents. They also protect the anticancer drugs from breaking down due to water and enzymes. Thus the drugs are released over a sustained period of time, reducing the frequency and dosage of injections. Nanoemulsions are suitable for delivery of active ingredients through the skin. The small size of the droplets improves the uniformity of deposition over surfaces.
- Liposomal DDS: A liposome is an artificially prepared spherical vesicle composed of arrangements of two layers of lipid molecules. They consist of biocompatible and biodegradable material. They are suitable for both hydrophobic and hydrophilic anticancer agents. They can be administered through various routes and give localized action in particular tissues. Liposomes are suitable for target release and controlled release of drug delivery.
- Microparticle DDS: Microparticles refer to solid particles with a size in the range of 1 to 1000 micrometers. The cancer drug is dissolved, entrapped, encapsulated or attached to a microparticle matrix. The drug is confined to a cavity surrounded by a polymer membrane called microcapsule. Microspheres are matrix systems in which the drug is physically dispersed uniformly. Microparticles are easy to administer into the body through a variety of routes due to their size. The drug is effectively protected in the capsule and hence the release of drugs is effectively controlled for a longer duration of time.
Nanotechnology in Drug Delivery – Cancer treatment
Nanotechnology is the science of development of man-made materials in the 5-200 nanometer size range. Nanotechnology is the engineering of functional systems at the molecular scale and is characterized by unique physical, optical and electronic features that find their applications in the field of material science and medicine. Due to the unique physicochemical properties of nanoparticles, they show great potential for use in the targeted drug delivery systems.
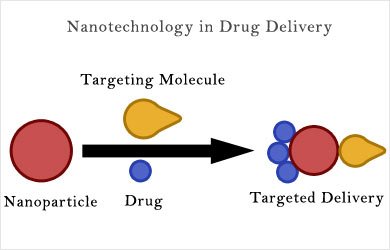
Nanoparticles have longer circulation half-life than other drug delivery vehicles. Circulation half-life refers to the amount of time the particles are reduced to half of their previous level by degradation, while in the human blood circulation. Nanoparticles also have enhanced permeability and retention effect, implying that they are better absorbed and dispersed within the tumor cells.
Nanoparticles are now available as drug carriers in the form of liposomes, capsules, tablets, gels and creams, aerosol sprays and aqueous solutions. They are also available as intravenous injections, without the risk of possible embolism. Nanoparticles offer hope for developing more energetic and more targeted methods of drug delivery, in which medications travel passively in the bloodstream and become active on reaching the target sites.
The compounds used as anticancer agents and cancer drugs are often highly toxic to many of the normal cell types. Targeting these compounds to the specific sites is crucial to minimize the effects on the healthy surrounding cells.
Materials used as Nanoparticle Carriers
Nanoparticles comprising gold, metal, iron oxides, polymers, silica, silver, composite and carbon types are used to make the anticancer agent stay longer in the tumor and increase the efficacy of the treatment. The choice of the nanoparticle depends on various factors.
- Polymeric nanoparticles are most widely used as it aids in the performance of poorly soluble drugs administered through any route.
- Noble metal nanoparticles have high surface-to-volume ratio, broad optical properties and are easy to synthesize.
- Metals like gold and silver can convert light or radiofrequencies into heat, and efficiently “burn” the cancer cells.
- Use of other nanoparticles as carriers is based on the properties of the compounds used as anticancer agents.








