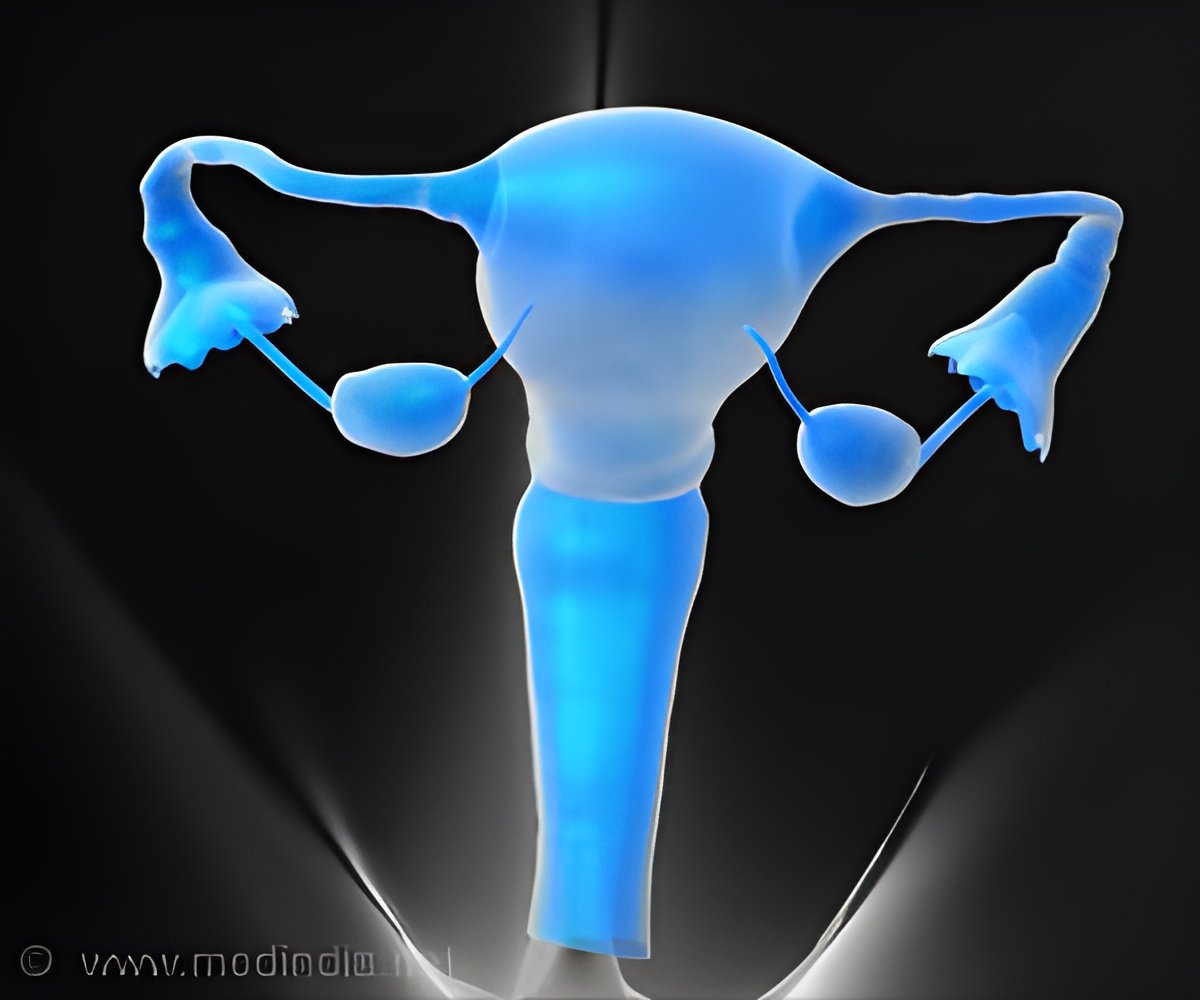
‘Surgical removal of the ovaries and fallopian tubes or bilateral salpingo-oophorectomy (BSO), may have health risks for younger pre-menopausal women, but is safer in older post-menopausal women.’
Read More..Tweet it Now
In Ontario, around 12,000 women undergo hysterectomy for non-cancerous gynecologic conditions each year. It is the most common major surgery performed on non-pregnant women worldwide, according to the Organization for Economic Co-operation and Development.Read More..
Previous study suggested that bilateral salpingo-oophorectomy (BSO) may be linked to an increased risk of death in younger women. However, limited data are available on BSO in older women, creating uncertainty for surgeons about what to recommend for women over 50.
“Our core goal was to try to understand the health risks associated with bilateral salpingo-oophorectomy for women of different ages, and provide information that patients and surgeons need to make the right treatment decisions,” said Dr. Maria Cusimano, lead author of the study.
Researchers at Unity Health Toronto and ICES evaluated 200,549 women who underwent hysterectomy either with or without concurrent BSO, from 1996 to 2015, and split the women into four age groups.
The analysis found an increased risk of death in women who had undergone BSO in the under 45 and the 45–49 age groups, but not in the 50–54 or over 55 groups. The median follow-up to assess survival was 12 years post-procedure.
Advertisement
To find out the relationship between BSO and mortality as women age, researchers used a different, more advanced modelling technique and still found that the overall relationship gradually shifted from harmful to not harmful around the years when most women begin the transition to menopause.
Advertisement
"There are definite cancerous and non-cancerous conditions where we actually do need to remove the ovaries, even if a woman is premenopausal. Our study shows that surgeons need to be cautious about removing the ovaries without a clear reason in premenopausal women. However, this strategy may be a safe and effective way to prevent ovarian cancer in older postmenopausal women.”
The risk of death in women who undergo BSO prior to menopause is higher because BSO in these patients prematurely stops all ovarian hormone production, which may predispose them to serious health problems later in life. The production of estrogen affects multiple organs and a sudden loss of the hormone may contribute to the development or progression of disease.
When the ovaries are removed during hysterectomy in pre-menopausal patients, the sudden loss of hormone production effectively puts patients in “sudden menopause” and patients will immediately begin to experience menopausal symptoms.
Side effects include fatigue, hot flashes, insomnia, and increased risk of osteoporosis and heart disease, according to the Canadian Women’s Health Network.
Researchers say that the findings will allow surgeons to help patients make more informed choices about their health, but that more research is needed on the impact of BSO to quality of life and sexual function to more fully guide decision-making in this area.
Source-Medindia