Guido Silvestri, MD, division chief of Microbiology and Immunology at the Yerkes Research Center at Emory, and several of his research colleagues performed the first hematopoietic stem cell transplantation in three rhesus macaques infected with a simian human immunodeficiency virus (SHIV). Silvestri's colleagues on this study include Maud Mavigner, PhD, Yerkes and Emory Vaccine Center, Ann Chahroudi, MD, PhD, Emory University School of Medicine (EUSOM) Department of Pediatrics, and Leslie Kean, MD, PhD, and Benjamin Watkins, MD, EUSOM Department of Surgery.
The team of researchers harvested hematopoietic stem cells from three macaques prior to SHIV infection of all six animals in the study, treated the animals with anti-retroviral therapy (ART) to reduce viral load and mimic the situation in human HIV-infected patients who are treated with ART, and then exposed the three monkeys from which they had collected hematopoietic stem cells to a high dose of radiation. According to Silvestri, "This treatment eliminated most of the existing blood and immune cells, including up to 99% of the animals' CD4-T cells, which is the main target of HIV infection."
Following the irradiation, the researchers transplanted each monkey's own virus-free hematopoietic stem cells. The stem cells regenerated blood and immune cells in all three monkeys within six weeks, at which time the scientists stopped ART in all of the monkeys.
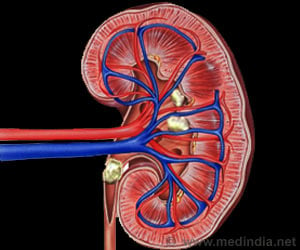
"As we expected, the virus rebounded rapidly in the control animals," says Silvestri. "Of the three transplanted animals, two also showed a rapid rebound, while the third animal had no rebound for two weeks. Unfortunately, we had to euthanize this monkey because of kidney failure, so we don't know how long this control would have lasted." Post-mortem analysis of the monkey that experienced no virus rebound after ART interruption showed low levels of viral DNA in a number of tissues.
Silvestri says, "These results support our hypothesis that a massive depletion of hematolymphoid cells by total body irradiation can cause a significant decrease in the viral reservoir in the body. At least in one monkey, we were very close to eliminating all reservoirs, so we think this approach is promising. We'll use what we've learned in this test-of-concept study to refine our research model toward our goal of curing HIV infection in all humans."
Advertisement
Source-Eurekalert