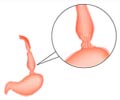
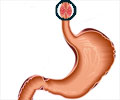
Barrett’s esophagus, a condition that affects the esophagus or food pipe, has been linked to cancer. Barrett’s esophagus occurs as a consequence of damage to the inner lining of the esophagus by acid regurgitating upward from the stomach. The cells of the esophagus change their appearance and resemble the intestinal lining.
Barrett’s esophagus is a premalignant condition, that is, it predisposes a person to esophageal cancer. The patient may initially show some cellular changes called low-grade dysplasia. Low-grade dysplasia may further progress to high-grade dysplasia and then to a type of cancer called adenocarcinoma. It is for this reason that people with Barrett’s esophagus are recommended periodic surveillance with repeated endoscopies and biopsies at regular intervals.However, recent statistics indicate that most cases of adenocarcinoma in the general population do not have a previous diagnosis of Barrett’s esophagus. Also, regular surveillance of cases of Barrett’s esophagus has not shown any benefit in terms of survival.
A large study was carried out to estimate the risk of developing adenocarcinoma and high-grade dysplasia in patients with Barrett’s esophagus in Denmark. Data for the study was obtained from the Danish Pathology Registry and the Danish Cancer Registry. In addition, the researchers also aimed to compare the incidence of adenocarcinoma in patients with Barrett’s esophagus with that of the general population. They also tried to find out whether the presence of low-grade dysplasia at the time of diagnosis of Barrett’s esophagus could influence the development of adenocarcinoma or high-grade dysplasia.
According to the data, 11,028 patients in Denmark were diagnosed as suffering from Barrett’s esophagus based on endoscopic biopsy between the years 1992 to 2009. These included 7366 men and 3662 women. During the follow-up period of a median of 5.2 years, 197 new cases of adenocarcinoma were diagnosed. Of these, 131 cases were diagnosed in the first year of follow up following diagnosis and 66 or 33.5% cases were diagnosed after the first year.
During this same period, 2602 new cases of adenocarcinoma were diagnosed in the general population. Thus, only 7.6% of all cases of adenocarcinoma occurred in patients with pre-existing Barrett’s esophagus.
The study thus showed that though patients with Barrett’s esophagus are at a risk of developing high-grade dysplasia and adenocarcinoma, the risk is relatively lower that what was previously reported. In fact, it states that the incidence was 4 to 5 times lower than what was previously reported.
Low-grade dysplasia also increased the changes of patients suffering from high-grade dysplasia in the later years.
The study thus concludes that the risk for developing esophageal adenocarcinoma is small in the absence of dysplasia. Thus, subjecting these patients to routine surveillance may not be necessary. This approach could reduce the cost of treatment as well as inconvenience to the patient. In fact, the American Gastroenterology Association has recently recommended considering removal of dysplastic cells through endoscopic eradication rather than surveillance especially in cases of high-grade dysplasia.
Reference:
1. Hvid-Jensen F, Pedersen L, Drewes AM, Sørensen HT, and Funch-Jensen P. Incidence of Adenocarcinoma among Patients with Barrett's Esophagus. N Engl J Med 2011; 365:1375-1383
Source-Medindia