The mystery behind why some children are more susceptible to malaria infection and anaemia has been deciphered by a new study led by an Indian origin scientist.
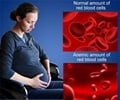
Lead researcher Indu Malhotra from Case Western Reserve University School of Medicine suggests that children who are exposed to Plasmodium falciparum (P. falciparum) malaria before birth become tolerant to the malaria parasites, or their soluble products.This tolerance, which persists into childhood, reduces the ability of the immune system to attack and destroy parasites and increases the susceptibility of these children to develop a malaria infection.
It also increases their risk for anaemia.
"This is the first time it has been shown why some children are more susceptible to malaria and anaemia than other children," said Malhotra.
"This study is timely given President Obama's Global Health Initiative to assist developing countries to control malaria, one of the 'big three' diseases," she added.
The researchers investigated how prenatal malaria exposure affects anti-malaria immunity in young children and their susceptibility to subsequent malaria infections.
Advertisement
The babies were classified into three groups: "sensitized" - those babies whose cord blood cells produce activating cytokines in response to the malaria antigens; "exposed, not-sensitized" - babies whose bodies did not produce activating cytokines but made an inhibitory cytokine; and "not-exposed"- babies born to mothers with no P. falciparum malaria infection at delivery.
Advertisement
They also had lower hemoglobulin levels, a sign of anaemia, than the other babies. The T cells of "exposed, not-sensitized" children were less likely to make activating cytokines in response to malaria antigens.
The study appears in the open access journal PLoS Medicine.
Source-ANI
RAS