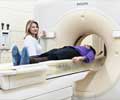
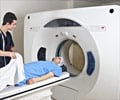
Coronary artery disease (CAD) is diagnosed through conventional coronary angiography, but this technique is invasive and potentially risky.
While several less invasive tests can be used to view the coronary arteries, computed tomography (CT) and magnetic resonance imaging (MRI) are preferred because of their superior image quality. An obvious indication for these noninvasive tests would be to reliably rule out CAD in patients with a low-to-moderate likelihood of the disease, thus avoiding an unnecessary invasive test. Researchers reviewed studies that compared CT (89 studies) or MRI (20 studies) to conventional coronary angiography in patients with suspected or known CAD. The studies were comprised of 7,516 and 989 patients, respectively. The researchers found that for ruling out CAD, CT is a more accurate noninvasive test than MRI.2. Extended-Duration Transdermal Nicotine Therapy Increases Smokers' Chances of Quitting Successfully
While the health benefits of smoking cessation are well-documented, quitting for good proves challenging for most long-term smokers. The transdermal nicotine patch is one of the most widely used treatments for tobacco dependence in the United States. Current guidelines recommend eight weeks of treatment with the patch. However, the evidence for this recommendation is limited. Researchers recruited 568 long-term smokers who wanted to quit smoking to determine if extended-duration transdermal nicotine therapy could help them quit more successfully. All participants were offered eight behavioral counseling sessions. In addition, the smokers were randomly assigned to receive nicotine patches for either eight weeks or 24 weeks. Smokers assigned to eight-week therapy received placebo patches from weeks 16 to 24. At 24 weeks, tobacco abstinence rates were significantly higher in the extended- versus the standard-therapy group. The researchers conclude that since many persons resume smoking once they stop nicotine treatment, longer-term patch use should be considered.
3. NSAIDS Ineffective for Treating Pericardial Effusion Following Heart Surgery
Pericardial effusion, or fluid around the heart, is the abnormal accumulation of fluid in the pericardial cavity. The condition is common after heart surgery, with an incidence of 50 to 80 percent a few days after surgery. A serious condition called cardiac tamponade occurs in about 1 to 2 percent of patients who have cardiac surgery, often after they have already been discharged from the hospital. In cardiac tamponade large amounts of fluid around the heart keep it from pumping effectively. In a previous study, the powerful predictor of cardiac tamponade was the size of the effusion, with larger effusions putting patients at risk. Typically, physicians prescribe nonsteroidal anti-inflammatory drugs (NSAIDs) for post-surgical pericardial effusion because the fluid is thought to be caused by inflammation. Researchers conducted a randomized, double-blind study of 196 patients with moderate to large amount of fluid more than 7 days after cardiac surgery to determine if the NSAID diclofenac was effective in reducing postoperative pericardial effusion volume. Researchers randomly assigned patients to receive either a placebo or diclofenac for 14 days. The effusions decreased by about the same amount in both groups, and about the same number of patients developed cardiac tamponade in both groups. The researchers recommend that doctors stop prescribing NSAIDs post-surgical pericardial effusion because they have no clear benefit.
Advertisement
RAS