- Legg-Calvé-Perthes Disease – Mayo Clinic - (https://www.mayoclinic.org/diseases-conditions/legg-calve-perthes-disease/symptoms-causes/syc-20374343)
- Loder RT, Skopelja EN. The epidemiology and demographics of Legg-Calvé-Perthes disease. ISRN Orthop. 2011; 2011: 504393. DOI: 10.5402/2011/504393 . PMID: 24977062.
- Legg- Calve-Parthes disease – Genetic and Rare Diseases Information Center (GARD). National Center for Advancing Translational Sciences, National Institutes of Health (NIH), USA - - (https://rarediseases.info.nih.gov/diseases/6874/legg-calve- perthes-disease)
- Legg Calvé Perthes Disease – National Organization for Rare Disorders (NORD) - (https://rarediseases.org/rare-diseases/legg-calve-perthes-disease/)
- Legg-Calvé-Perthes Disease – Seattle Children’s - (http://www.seattlechildrens.org/medical-conditions/bone-joint-muscle-conditions/hip- conditions-treatment/hip-disorders/legg-calve-perthes-disease/)
What is Legg-Calvé-Perthes Disease?
Legg-Calvé-Perthes Disease (LCPD), also known as Perthes Disease or Legg-Perthes Disease is a childhood bone disorder in which the blood supply to the head of the femur (thigh bone) is temporarily interrupted. Due to lack of blood flow, the head of the femur (the "ball" of the “ball-and-socket” joint of the hip) dies by a process called osteonecrosis or avascular necrosis (AVN). As the disease progresses, the head of the femur gradually begins to break apart. Over time, the blood supply to the femoral head is restored and the head eventually grows back. The entire process of bone death, degeneration and regeneration can take up to several years.
Nomenclature
Legg-Calvé-Perthes Disease is named after three physicians, namely, Arthur Legg, Jacques Calvé, and Georg Perthes, who in 1910 independently recognized the symptoms and provided a comprehensive description of the disease.
Epidemiology
The incidence of LCPD ranges between 0.4/100,000 to 29.0/100,000 children below 15 years of age. There is variability in the incidence or probability of occurrence and is more prevalent in white populations and in lower socioeconomic groups. LCPD usually occurs in the age group of 4-8 years (average 6.5 years). However, in Indian children, the average age is 9.5 years. The disease is 5 times more common in boys than girls, although greater bone damage occurs in girls. In 10-15% of cases, both hips are affected.
What are the Four Stages of Legg-Calvé-Perthes Disease?
The four stages of LCPD are briefly described below:
- Avascular Necrosis (AVN) or Initial Stage: In this stage the blood supply to the femoral head is disrupted and the bone dies by AVN. The area becomes intensely inflamed and the child experiences pain and may start limping. This stage can last for several months.
- Fragmentation or Resorptive Stage: In this stage, which can extend for 1-2 years, the body removes the dead bone tissue. As a result, the femoral head becomes weakened and begins to break up.
- Reossification Stage: In this stage, the bone starts to regenerate and builds up the head of the femur. This stage is the longest and lasts for several years.
- Remodeling or Healed Stage: In this stage the ossification is almost complete and the femoral head attains its final shape through a process called bone remodeling. The degree of roundness achieved depends on several factors, including the degree of fragmentation that initially took place, as well as the age of the child when the disease process started. The younger the age, the better the ability to regenerate the bone.
What are the Causes of Legg-Calvé-Perthes Disease?
The exact cause of LCPD is unknown. However, it has been associated with epiphyseal dysplasia, trauma, toxic synovitis, steroid use, or slipped femur head. Moreover, some studies have suggested that inheritance or genetic factors could play a role. In fact, some cases of LCPD with autosomal dominant inheritance have been reported, with mutations in the COL2A1 gene.
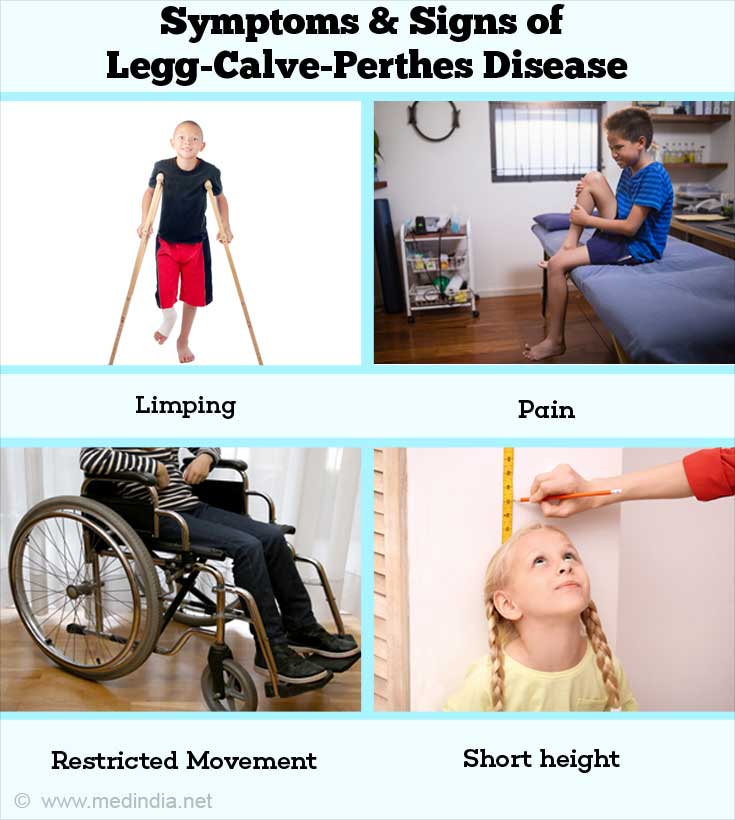
What are the Symptoms & Signs of Legg-Calvé-Perthes Disease?
The major symptoms experienced by children suffering from LCPD include the following:
- Limping: This is one of the first symptoms, which may occur with or without pain.
- Pain: There may be pain in the hip, knee, thigh and/or groin.
- Muscle Degeneration: There may be loss of muscle mass (muscle atrophy), in the thigh muscles. This can be accompanied by muscle spasms in the affected leg.
- Restricted Mobility: There may be restricted movement in the hips, accompanied by inflammation of the membrane lining the hip joint (synovitis).
- Short Stature: As the affected children become older, the length of their legs may differ (leg length discrepancy), leading to a short stature.
How do you Diagnose Legg-Calvé-Perthes Disease?
LCPD can be diagnosed by the following strategies:
- Medical History: A detailed medical history of the child will be taken, especially to gather information whether there is a family history of the disease.
- Physical Exam: The doctor will carry out a thorough physical exam in order to assess the cause of the presenting symptoms, such as pain, limping and restricted mobility.
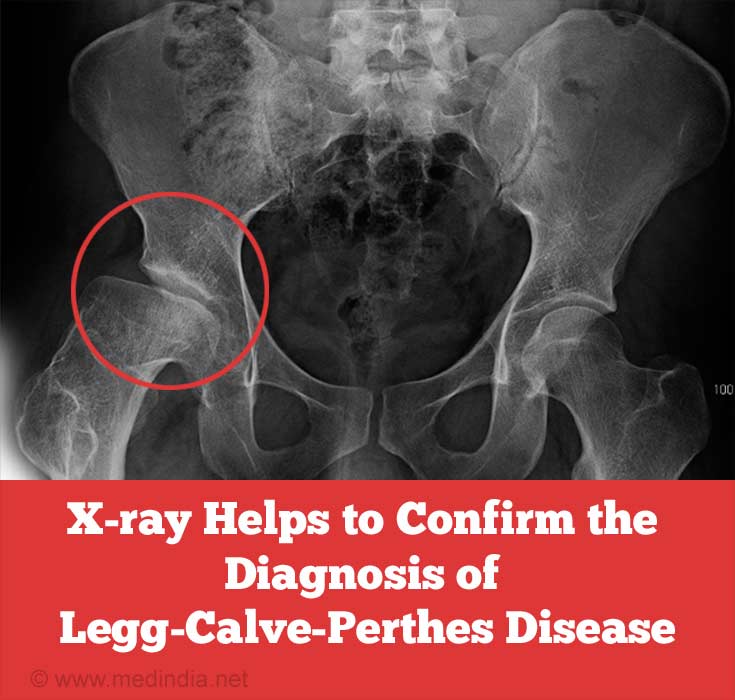
- X-Ray: Taking a standard X-ray of the upper end of the femur (capital femoral epiphysis) may reveal any abnormalities of the epiphysis. This will usually be sufficient to clinch the diagnosis.
- Specialized Investigations: If in doubt, the doctor will order some specialized investigations. These may include the following:
- Magnetic Resonance Imaging (MRI): In this imaging technique, a magnetic field and radio waves are used to create cross-sectional images of the upper end of the femur.
- Arthrography: In this technique, a contrast media is injected into the joint and imaged by radiography (X-rays) or in conjunction with fluoroscopy or MRI. The arthrogram provides a clear image of the soft tissues lining the joint, which helps to make an accurate diagnosis of the cause of the symptoms such as joint pain and/or inflammation.
- Scintigraphy: In this procedure a radioactive substance is injected into the joint and a scintillation counter is used to pick-up the radiations to visualize the internal structure of the joint.
How do you Treat Legg-Calvé-Perthes Disease?
Treatment involves the following strategies:
- Medical Treatment: These include (i) medicines for pain management and reducing inflammation, (ii) physical therapy for increasing mobility, or (iii) using assistive devices like braces for providing support. However, these are useful for children below the age of 6 years.
- Surgery: This is beneficial for children older than 6 years where the disease is more severe. The aim of surgery is to keep the head of the femur within the hip socket in order to maintain optimal mobility. The surgery is used to prevent the dislocation or collapse of the hip. The surgical procedure either tilts the ball so that it goes deeper into the socket, or rotates the socket so that it covers the ball better during walking. The surgeon may try both procedures simultaneously.

What is the Prognosis for Legg-Calvé-Perthes Disease?
The prognosis for patients with LCPD depends on the degree of bone degeneration and associated deformity. Overall, the prognosis for recovery after treatment is very good for most children. Generally, diagnosis at a younger age is associated with a better outcome. In children diagnosed below the age of 5 years the chance of development of degenerative arthritis later in life is reportedly low, while diagnosis above 10 years of age increases the chances appreciably. Moreover, the more deformed the femoral head is during reossification, the greater is the chance of developing osteoarthritis of the hip later in life, which may sometimes require a total hip replacement.






