- D C Dutta's textbook of gynecology
- Assisted Reproductive Technology (ART) - (https://www.nichd.nih.gov/health/topics/infertility/conditioninfo/pages/art.aspx)
- Assisted Reproductive Technologies - (http://www.sart.org/sart_assisted_reproductive_technologies/)
- What is Assisted Reproductive Technology? - (https://www.cdc.gov/art/whatis.html)
What is Assisted Reproductive Technology (ART)?
Assisted Reproductive Technology (ART) is a complex and biotechnologically advanced technique which can help a couple to conceive, when all the other conventional medical and surgical corrective procedures have failed. The various techniques of assisted reproductive technologies can be used for both males as well as females.
The technique is so advanced, that it can work at the microscopic level (cellular level) with your gametes (sperm and ovum), and has helped millions of shattered couples to become proud parents. The technique bypasses the role of sexual intercourse and the eggs and sperms are handled in the laboratory environment.

What are the Types of Assisted Reproductive Technology?
Assisted reproductive technology is a cluster of various techniques used for the treatment of infertility and comes under the field of reproductive endocrinology. The various techniques used are as follows:
- IVF-ET: In vitro fertilization and embryo transfer (IVF-ET): The ovum and sperm are taken from the parents and fused together in a petridish in laboratory. The resultant product of fusion or fertilization, called the zygote is your baby in the form of a single cell. It is then allowed to grow into the embryo, which is then transferred inside the uterus and the pregnancy is established.
- GIFT: The ovum and the sperm are injected into the fallopian tube and the fusion is attained inside the body of female
- ZIFT: In this technique, the ovum and sperm are made to fertilize in the petridish, and the resultant zygote is transferred to the fallopian tube of the female.
- IUI: In intrauterine insemination, the female is artificially inseminated by using the sperm from either husband or a healthy donor. The sperm is inserted deep inside the female’s uterus to establish the pregnancy.
- ICSI: In this technique, one single sperm is inserted directly into the cytoplasm of the ovum, through an injecting pipette under a high quality microscope.
How do you Prepare for an ART Procedure?
Since assisted reproductive technology is a costly affair, one must be thoroughly prepared to go for the procedure. Here are certain facts that must be kept in mind both by the couple and by the physician before attempting ART.
- Ovarian reserve testing is done to measure egg quality, quantity and reproductive potential. Levels of follicle stimulating hormone (FSH), estradiol and AMH (antimüllerian hormone) are taken on the second or third day of your periods. Also performed are the clomiphene citrate challenge test (CCCT) and counting the number of small follicles in the ovary (antral follicle count).
- Uterine cavity abnormalities like fibroids, polyps, or a septum are checked using a thin, flexible, lighted telescope (hysteroscope) along with a sonogram to view the images.
- Fallopian tube disorders like fluid-filled and blocked fallopian tubes must be clipped or removed before IVF.
- Semen must be tested before ART. Consult a specialist on male infertility, if there are correctable problems or underlying health concerns.
- Lifestyle issues: Smoking should be quit as it may lower a woman’s chance of success by as much as 50%. Obesity must be adequately dealt with and a more optimal weight prior to undergoing IVF must be achieved. Alcohol, recreational drugs and excessive caffeine consumption should be avoided.

What is In Vitro Fertilization and Embryo Transfer (IVF-ET)?
In vitro fertilization (IVF) is the most common and effective ART procedure where eggs and sperm are taken from the couple and are put together in a dish. The gametes are allowed to fuse together and grown up to the embryo stage. The embryo is then implanted into the lady's uterus, where it might embed and result in an effective pregnancy.
Criteria to select ideal patients for IVF-ET
- The couple must be less than 35 years of age
- Serum FSH level in females must be less than <10 IU/L
- Husband must have a normal seminogram
- The couple must test negative for HIV and hepatitis
- The uterine cavity should be found normal as evaluated by hysteroscopy
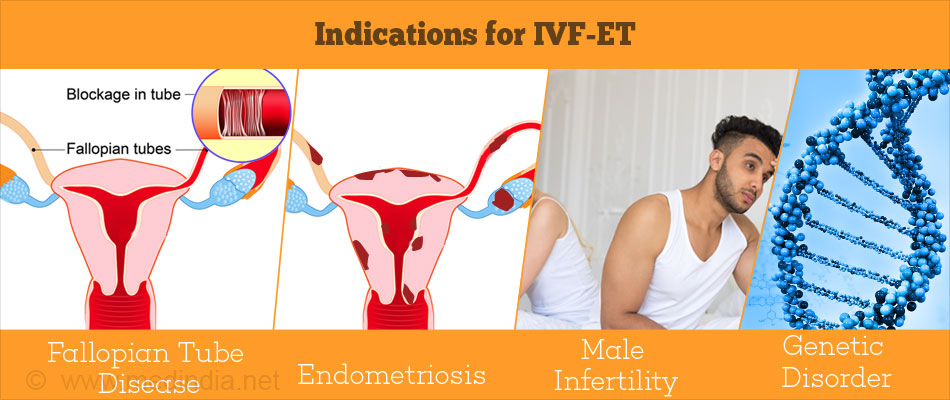
Indications for IVF-ET
- Fallopian tube disease ( such as blocked, damaged or absent fallopian tubes)
- Unexplained infertility
- Endometriosis
- Male factor infertility - abnormal sperm counts, motility, size or shape
- Failure to induce normal ovulation in female by fertility drugs
- Ovulation is infrequent or there is loss of ovarian function below the age of 40
- Women with normal ovaries but no functional uterus also called as Mullerian agenesis
- Women with a genetic disorder that is at risk to be passed on to the baby
- Benign uterine fibroids that might interfere with implantation of fertized egg
- Preservation of eggs prior to cancer radiation or chemotherapy treatment
Stimulation of Egg Maturation
In this procedure, otherwise called ovarian stimulation or ovulation induction, synthetic hormones are given by infusion for 8 to 14 days to fortify the ovaries to make many developed eggs at one time. The advancement of the eggs is closely monitored utilizing trans-vaginal ultrasound and blood tests.
Egg retrieval
Once the eggs are mature, the doctor takes out the eggs 34 to 36 hours after the injection. Egg retrieval is done under aseptic and anesthetic conditions through vaginal route, by the process of vaginal needle aspiration under ultrasound guidance. Painkillers are given. Post-retrieval, the ovum is maintained in a culture media in a petridish outside of the body for 4-6 hours.
Sperm retrieval
- A semen sample can be obtained from your partner at the clinic. There are medical procedures to assist ejaculation in men for those who cannot ejaculate normally by masturbation, may be due to spinal cord injuries. Testicular sperm extraction (TESE) is a medical procedureused to extract sperm from reproductive tissues for men who can ejaculate, but do not have sperm in their semen.
Fertilization (IN VITRO)
The sperm utilized for insemination is prepared by density gradient centrifugation technique.
1. Insemination: Around 50,000 to 100,000 capacitated sperm are placed in the petri dish containing the ovum within 4-6 hours of retrieval. The petri dish is left overnight in an incubator. The eggs may exhibit signs of fertilization, when inspected 16-18 hours after insemination. Sperm density and motility are the two most essential criteria for fruitful IVF.
2. Intra Cytoplasmic Sperm Injection (ICSI):
One single spermatozoon is made to penetrate directly into the cytoplasm of an ovum by micro puncture of the external membrane of ovum..This procedure is done under a high quality microscope.
Intracytoplasmic sperm injection is indicated in cases of extremely low sperm count (5 million sperm/mL), abnormal morphology of sperm, low sperm motility and presence of sperm antibodies, which kill the sperms in spite of perfectly normal sperm count.
Fertilization rate is about 60-70 percent. Pregnancy rate is 20-40 percent per embryo transfer.
Embryo transfer
The prepared ova at the 6-8 blastomeric stage are set into the uterine cavity near the fundus around 3 days after preparation through a fine adaptable delicate catheter transcervically. Not more than three embryos should be transferred per cycle to limit the risk of multiple pregnancies.
The number of embryos to be transferred depends predominantly on maternal age and the embryo quality.
Determination of pregnancy by estimation of B-hCG or human chorionic gonadotropin hormone confirms conception.
What is Sperm Donation and Ovum Donation?
Sperm donation Couples can use donated sperms, when a man does not produce sperm or produces extremely less numbers of sperm, or if he suffers from a genetic disease. Donated sperm can be used either with intrauterine insemination or with in vitro fertilization.

Ovum donation It is used when the female is unable to produce healthy eggs that can be fertilized. The egg donor undergoes ovary stimulation and egg retrieval steps of IVF. The husband’s sperm can then fertilize the donated egg and the embryo is implanted into the woman's uterus. It is helpful for women who have primary ovary insufficiency, who have undergone surgical removal of the ovaries, or were born without ovaries, are carriers of any genetic disease, or are unable to conceive because of poor egg quality.
What is Gamete Intra Fallopian Transfer (GIFT)?
In this system, both the sperm and the unfertilized ovum are moved into the fallopian tubes. Fusion of gametes is then accomplished in vivo that is inside the body. The essential element for GIFT is to have normal and healthy uterine tubes.
The general pregnancy success rate is as high as 27-30 percent but it is a more invasive and costly procedure as compared to in vitro fertilization. The outcome is poor in male associated infertility.
What is Zygote Intra Fallopian Transfer (ZIFT)?
In this technique after in vitro fertilization, instead of transferring the embryo, the zygote is placed in the fallopian tube, a day after the in vitro fertilization. This technique is the perfect substitute of GIFT when the defect lies in the husband or in cases of a failed GIFT. It is contraindicated in cases where the tubal factors for infertility are present.
What is Intra Uterine Insemination(IUI)?
Intrauterine insemination involves the insemination of a man's sperm into a woman's uterus using a long, narrow tube. It is more suitable in men who have low sperm counts, sperms with low motility, erectile dysfunction and men with history of retrograde ejaculation (a condition where semen is ejaculated backwards into the male’s urinary bladder instead of out of the penis into woman’s vagina).
IUI is used in combination with medications to enhance ovulation and this combination increases the chance of conception greatly.
What is Cryopreservation of Embryo/Ovum/Ovarian tissue/ Sperm?
Cryopreservation of embryos- Extra embryos that remain after the embryo transfer in case of in vitro fertilization can be cryopreserved (frozen) for future use by conventional (slow) freezing and “vitrification” or fast freezing. This technique makes future ART cycles simple, cheap, with minimal invasion, and the embryos can be stored for prolonged periods.
Cryopreservation of eggs- Nowadays, cryopreservation of eggs or ovum prior to fertilization is commonly done in young women who are about to take certain therapies or procedures that might adversely affect their future fertility, such as chemotherapy for cancer.
In addition, it must be noted that, there are no documented cases of infectious disease transmission, or the risks of birth defects, chromosomal abnormalities by using cryopreservation technique compared with using fresh sperm, eggs, or embryos.
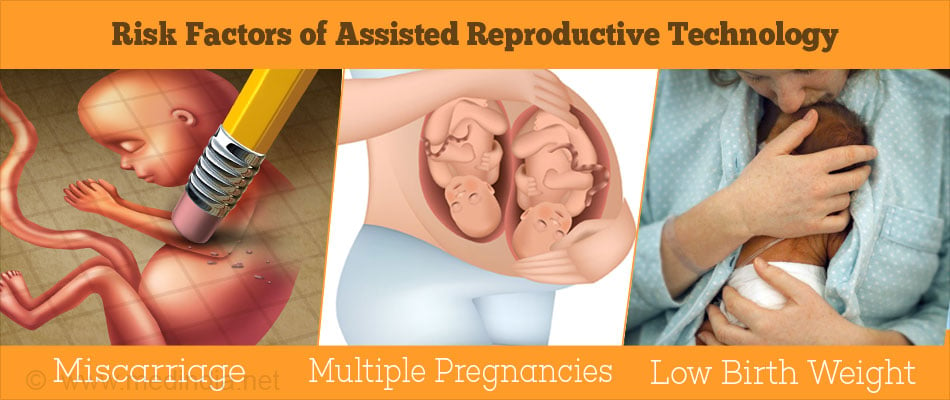
What are the Risk Factors of Assisted Reproductive Technology?
There is increased risk of the following:
- Miscarriage (18%): Miscarriage may occur in approximately 15% of women younger than age 35, in 25% at age 40, and in 35% at age 42 after the use of assisted reproductive techniques.
- Multiple pregnancies (31%): There is high risk of preterm deliveries in cases of multiple pregnancies.
- Ectopic pregnancy (0.9%): It manifests as first-trimester bleeding. Bleeding or pain (before 13 weeks), indicates a need for medical evaluation to determine the cause.
- Low birth weight of baby and prematurity.
- Perinatal mortality and morbidity.
- Ovarian hyper stimulation syndrome when fluid accumulates in the abdominal cavity and in the chest. The female will feel bloated and nauseated. She might also experience vomiting and lack of appetite.
- A minimal risk of bleeding, infection, and damage to the urinary bladder, bowel, or a blood vessel during removal of eggs through aspirating needle.
- Increased psychological stress and anxiety for the couple due to the fear of failure of treatment or with a pregnancy loss. There is a major financial and emotional component involved on behalf of parents.
Health Tips
If depression and feelings of low self-esteem occur, especially after a failed ART attempt, couples are encouraged to go for psychological counseling for extra support and stress management.