New research has indicated that a new virus that causes severe breathing distress and kidney failure elicits a distinctive airway cell response to allow it to multiply.
Their findings predict that certain currently available compounds might treat the infection. These could act, not by killing the virus directly, but by keeping lung cells from being forced to create a hospitable environment for the virus to reproduce.
The researchers caution that their lab and computer predictions would need to be tested to see if the drugs work clinically.
The results appear in the April 30 issue of mBio, the Journal of the American Society for Microbiology.
University of Washington virologist Laurence Josset is lead author of the paper, "Cell host-response to infection with novel human coronavirus-EMC predicts potential antivirals and important differences with SARS-coronavirus."
She conducted the research in the laboratory of senior author Michael G. Katze, UW professor of microbiology noted for pioneering systems biology approaches to host and pathogen interactions.
Advertisement
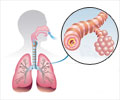
The new disease agent belongs to the betacoronavirus family, as does the severe acute respiratory syndrome virus, SARS. Both viruses attack the lungs. The new virus, however, is more closely related to bat coronaviruses than to SARS. The two viruses latch onto different receptors to infect cells.
Advertisement
Later, and throughout infection, the human coronavirus EMC incites a massive sabotage – much greater than that of the SARS virus – of many genetic controls of protein production in lung cells grown in the laboratory.
"We found that a set of 207 genes in the lung cells was dysregulated early and permanently throughout infection with human coronavirus EMC," Josset said. Various RNA levels were turned up or down.
The new virus appears to specifically hamper the work of several genes that enable the body to sense the presence of viruses. The scientists believe such gene re-tuning by the virus could significantly lower the ability of lung cells to mount an appropriate antiviral reaction.
While SARS and EMC activated a few similar lung cell responses for their own benefit, overall, not much overlap occurred. Each bad actor had its own modus operandi for interfering with lung cell gene activities.
Source-Eurekalert