‘Infective endocarditis (IE) patients who struggle with substance use disorder (SUD) are at a higher risk of dying within 6 months to 5 years after valve surgery. Therefore, it is necessary to treat SUD at the earliest to help patients improve their outcomes.’
Read More..Tweet it Now
Dr. Wurcel and colleagues queried The Society of Thoracic Surgeons Adult Cardiac Surgery Database for data related to patients who underwent heart surgery between January 2002 and December 2016 after an IE diagnosis.Read More..
The researchers also reviewed notes and toxicology screens included in the institutional medical records, identifying those with illicit drug use. Of the 228 patients who had surgery for IE during that time frame, 80 patients (35%) had SUD-IE and also were significantly younger than the non-SUD-IE patients (38 years old vs. 60 years old).
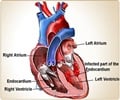
IE is a life-threatening bacterial infection in the endocardium, which is the inner lining of the heart chambers and valves. While this condition is often associated with heart defects or abnormal valves, it also is a notorious complication after using unsanitary needles and syringes to inject drugs, as bacteria from the skin’s surface and injection equipment release directly into the bloodstream. Despite medical advances, SUD-IE remains difficult to treat and has a high recurrence rate.
“Substance use disorder adds another layer to the complexity of managing postoperative valvular heart disease,” Dr. Wurcel said.
According to the Centers for Disease Control and Prevention, people with SUD-IE are 10 times more likely than other patients with IE to require a second surgery or die months after leaving the hospital. This research concurred, showing that repeat valve replacement for IE was more likely to happen in people with SUD than in those without (14% vs. 3%).
Advertisement
Dr. Wurcel explained that in this “midterm” period, patients with SUD-IE often find themselves with unstable housing conditions, limited access to transportation, and other challenges that prevent them from utilizing addiction-related services.
Advertisement
Because patients with SUD-IE tend to leave the hospital before completing the recommended weeks-long series of antibiotics treatment or fail to follow self-care instructions provided upon discharge, Dr. Wurcel recommended that traditional cardiac units offer addiction treatment so that patients can remain in recovery once they leave the hospital.
“We should focus more resources—both clinical and research—into understanding what people need to stay healthy,” said Dr. Wurcel. “We need to shift the paradigm of how we think about addiction. It is an illness with environmental and genetic triggers.”
Without a comprehensive approach to treating addiction, Dr. Wurcel said that outcomes for patients with SUD-IE likely will not improve. As a result, Tufts University created a multidisciplinary team approach to address IE and the contributing substance abuse. Surgeons, infectious disease clinicians, addiction specialists, case workers, and nurses work closely together and meet every 2 months to discuss patients with SUD-IE who are currently in the hospital or recently have been discharged.
“The opioid epidemic is a multiheaded monster that can be fatal in many ways,” said Thomas E.
MacGillivray, MD, of Houston Methodist in Texas, who was not directly involved with this research. “Substance abuse has long been known to be causative of endocarditis requiring high-risk valve repair or replacement surgery. This study highlights the continued increased risk of death in substance abuse patients even after the valve disease is addressed. More emphasis should be placed on managing the primary disease of substance abuse during the initial hospitalization in order for the secondary problem of endocarditis to have a lasting impact on survival.”
Dr. Wurcel agreed that reinfection may be prevented if patients are offered medication for substance use disorder (e.g., buprenorphine or methadone) and the importance of early and continued addiction management is emphasized.
“The health care team plays a crucial role in reversing the tide of substance abuse and addiction,” Dr. Wurcel said. “We are the people to whom patients turn in their times of need. Many with substance use disorder avoid medical interactions because of negative experiences. We need to focus on the patients every step of the way and change that.”
Source-Newswise