Preeclampsia, a dangerous form of hypertension during pregnancy can be fatal for both mother and child. The root cause of preeclampsia remains a mystery although it is known to originate in the placenta. An international research team led by the Max Delbrück Center for Molecular Medicine (MDC) has shown that epigenetically regulated genes play an important role in preeclampsia and it is not solely caused by genetic factors. The Berlin research team also developed an in vitro model of the disorder which demonstrates the dysregulation of an important transcription factor. The findings are published in the scientific journal
Circulation.
The research team compared placental tissue samples and the genetic makeup of patients with preeclampsia with those of healthy women. The entirety of their genetic material was analyzed for genes that are differentially expressed in the preeclamptic versus healthy placentas and checked for disrupted genomic imprinting, which refers to certain genes that are "switched off" on either the paternal or maternal chromosome. This led them to identify the so-called DLX5 gene as a significant transcription factor involved in regulating the activity of other genes in preeclampsia. This gene is usually turned off - or epigenetically "imprinted" - on the paternal chromosome, controlling the proper dosage of gene expression. Due to loss of the regulation by imprinting, DLX5 was strongly upregulated in case of 70 percent of the samples studied from preeclampsia patients, meaning the gene was switched on in these cases. This study is the first to demonstrate that a change in epigenetic gene regulation by imprinting can contribute to preeclampsia. The scientists also found three separate types of preeclampsia, supporting the view that preeclampsia is a complex disease.
‘DLX5 gene identified as a significant transcription factor involved in regulating the activity of other genes in preeclampsia.’




The study involved close collaboration between basic research and clinical institutes. Participants included research groups led by the molecular biologist Dr. Zsuzsanna Izsvák of the MDC and Dr. Ralf Dechend of the Helios clinic in Berlin-Buch and the Experimental and Clinical Research Center (ECRC), a joint institution of MDC and Charité - Universitätsmedizin Berlin. The interdisciplinary team also included researchers from the Berlin Institute of Health (BIH) and the evolution biologist Laurence Hurst from University of Bath, UK.
Development of the in vitro cell model for preeclampsia
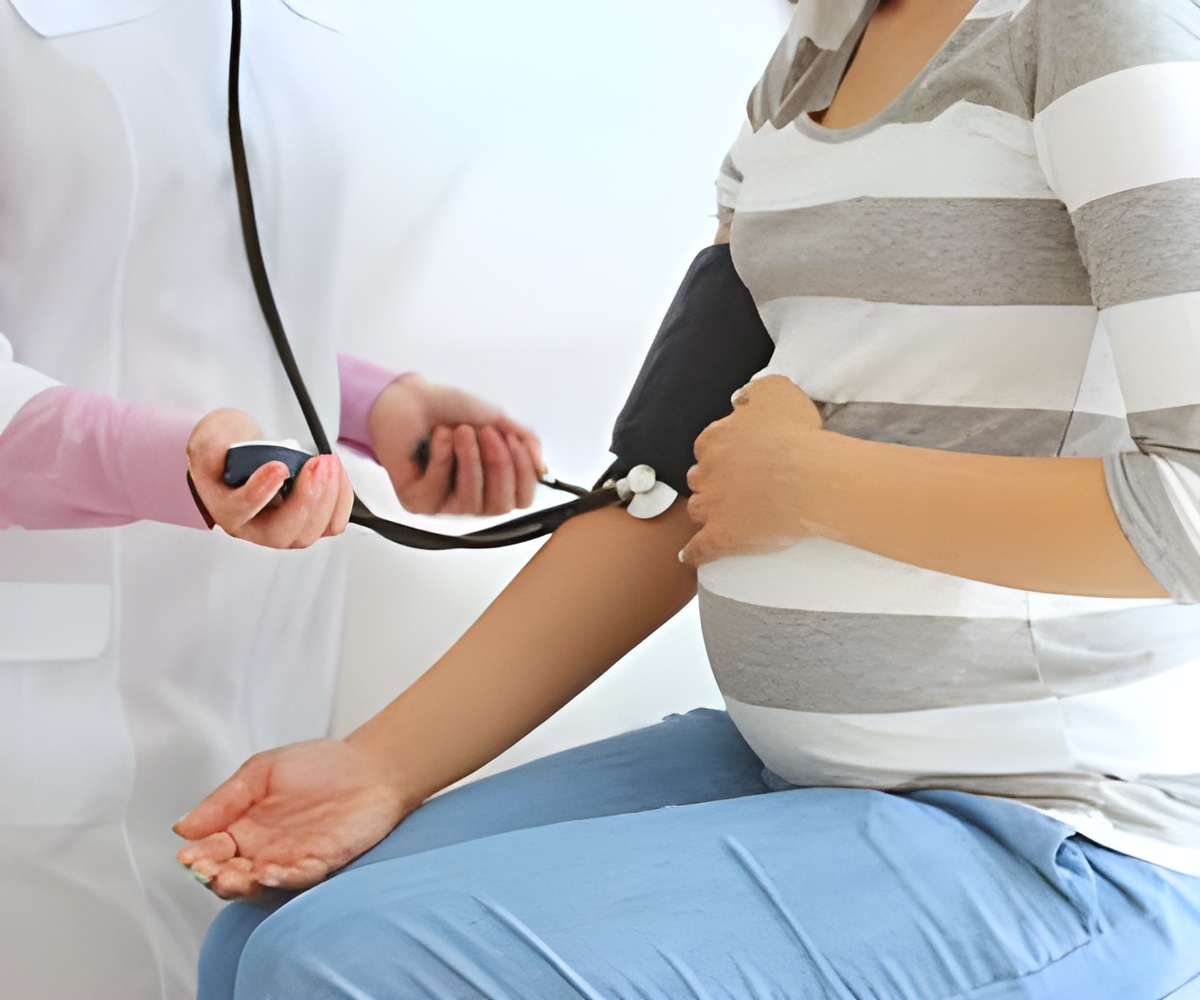
Preeclampsia affects around four percent of all pregnancies. Its main symptoms are high blood pressure and protein in the urine. If these symptoms reach dangerous levels, delivery must be induced prematurely. In Germany, preeclampsia causes as many as 20,000 premature births every year. The condition occurs only in humans, and no robust animal models have been proven suitable. The development of an in vitro model is therefore of vital importance.
Here, the Berlin-based research group achieved a real breakthrough. In their in vitro model, they increased the activity of the DLX5 gene in the trophoblastic cells - the outer layer of the embryonic cell that later builds the placenta. The cells showed an increased stress response, which is also observed in patients. This cellular system will now allow for further investigation into the different types of preeclampsia and for new medications and active agents to be found.
Why does this condition only affect humans?Advertisement
Izsvák and Dechend are already planning the next steps: "We want to find out why this condition occurs only in humans," says Izsvák. "We also hope to find biomarkers for the three types of preeclampsia we have identified," adds Ralf Dechend. "These will help diagnosing or predicting the disease before the actual illness develops."
Advertisement
Source-Eurekalert