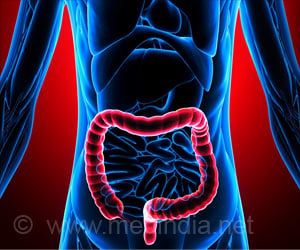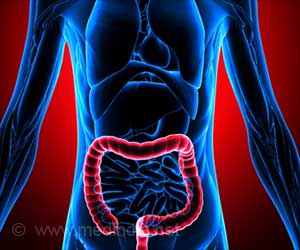
‘The medical approach for patients with IBD is symptomatic care and mucosal healing following a stepwise approach to medication, with escalation of the medical regimen until a response is achieved.’





On an average, humans ingest 1.5 litres of saliva containing bacteria every day, which could possibly have harmful effects on health. "We noticed that oral microbes are relatively enriched in gut microbiomes of patients with several diseases such as inflammatory bowel disease, HIV infection, and colon cancer compared with healthy individuals," said Masahira Hattori, Professor at the Waseda University in Tokyo.
For the study, published in the journal Science, the team administered salivary samples of healthy and inflammatory bowel disease-afflicted individuals to germ-free mice.
After six to eight weeks, the microbial content of the mice’s faeces were analysed, which showed that approximately 20 kinds of oral bacteria were present in these mice.
Klebsiella pneumoniae is usually a normal resident in the mouth of healthy individuals. However, the researchers advised against excessive and long-term use of antibiotics as Klebsiella pneumoniae could persist in the intestine.
Advertisement
"The study demonstrates for the first time that intensive periodontal intervention alone can reduce blood pressure levels, inhibit inflammation and improve endothelial function," said lead author Jun Tao, Chief of the department of Hypertension and Vascular Disease at the varsity.
Advertisement
Source-IANS