‘A fundamental understanding of how molecular mechanisms either boost or damp our immune response against Candida albicans will pave the way for a drugs against deadly fungal infections.’
Tweet it Now
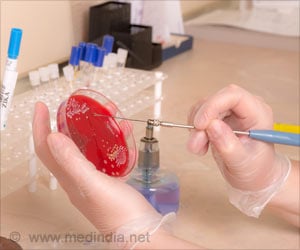
Knowing the enemyWhen fungal cells enter the body, they stand out from our own cells because they are ‘flagged' with unique patterns of molecular markers. These ‘pathogen-associated molecular patterns', or PAMPs for short, are recognised by receptor proteins on cells of the immune system. These receptors then activate signalling molecules triggering a cascade of different immune functions, such as inflammation, aimed at recruiting immune cells to the infected area. Those recruited immune cells will then, for example via the production of highly toxic reactive oxygen species, eliminate fungal pathogens.
"Unleashing" an immune response
Candida albicans is recognized by certain PAMP receptors, called Dectins, and triggers activation of the signalling molecule SYK. The first authors of the study, Gerald Wirnsberger (IMBA) and Florian Zwolanek (MFPL), now discovered that the protein CBL-B acts as a ‘brake' in this pathway: when CBL-B is present, Dectin and SYK activity are dampened and immune responses are eventually ‘switched off', but when CBL-B is absent, Dectin/SYK get over-activated and a protective anti-fungal immune responses occur.
Using this knowledge, the two research groups around Josef Penninger (IMBA) and Karl Kuchler (MFPL) - designed an inhibitory peptide to block CBL-B activity and thereby unleash defence mechanisms against invading fungal pathogens. After successfully testing this peptide with lab-grown cells, the peptide was used to treat Candida albicans infected mice. While untreated mice succumbed to the lethal infection, peptide treatment provided complete protection from fungal disease.
Gerald Wirnsberger explains: "This work constitutes a novel paradigm in antifungal therapy - a pharmacological modulation of the host immune response mediated by CBLB. A fundamental understanding of how molecular mechanisms either boost or damp our immune response against Candida albicans will pave the way for a drugs against deadly fungal infections".
Source-Newswise