New research indicates that women with a previous history of cardiovascular issues seem to have a higher cancer risk after five years of vitamin supplementation. The research is published in detail in the
Archives of Internal Medicine.
Although some studies have suggested that supplementation with B vitamins has some benefits for protecting against cancer, the few randomised clinical trials conducted internationally in recent years remain equivocal.The results of studies of the influence of supplementation with polyunsaturated fatty acids have been mixed.That is why Valentina Andreeva and Pilar Galan and their staff wanted to study the effects of B vitamins and omega-3 polyunsaturated fatty acids (PUFAs) on cancer by monitoring, for five years from 2003 to 2009, more than 2500 people aged between 45 and 80 who had survived a heart attack, stroke or angina in the last 12 months.The aim of the trial was to check the hypothesis that supplementation with en5-methyl-THF (and vitamins B6 and B12) and/or omega-3 was of value in preventing the recurrence of ischaemic pathologies in subjects who had suffered a heart attack or stroke.The results, published this week in the
Archives of Internal Medicine, are the outcome of a specific analysis performed as part of the intervention study SU.FOL.OM3, the results of which were published in 2010 in the
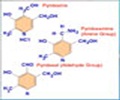
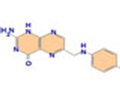
British Medical Journal SU.FOL.OM3 is a randomised double-blind placebo-controlled secondary prevention trial in which participants aged from 45 to 80 years with a previous history of cardiovascular pathologies were given daily supplements for five years of B vitamins (3 mg of vitamin B6, 560 μg of folates and 20 μg of vitamin B12) and/or omega-3 PUFAs (600 mg of eicosapentaenoic acid, EPA, and docosapentaenoic acid, DHA, in a ratio of 2:1), according to a factorial design.
It tested the effect of supplementation on cancer development over the five-year monitoring period in 145 men and 29 women.
All types of cancer were monitored"Despite the low numbers, the results are significant," the authors believe, because the "methodology used – a randomised double-blind trial – is stringent".
The researchers conclude that "Neither B vitamin supplementation nor omega-3 PUFA supplementation has a significant effect on the occurrence of cancer in men. However, women receiving omega-3 fatty acids tended to present a higher risk of cancer compared with the placebo group (adjusted HR =3.02; CI of 95 % = [1.33; 6.89]). Although the underlying mechanisms are not clear, a potential mediating effect on the metabolism of oestrogens is suggested," they add.
To confirm or contradict these results, it is necessary to await new studies: randomised trials, cohort studies and mechanistic studies.
Source-Eurekalert