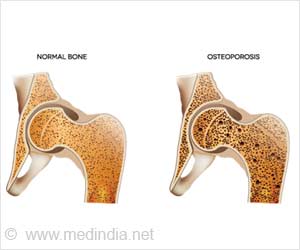
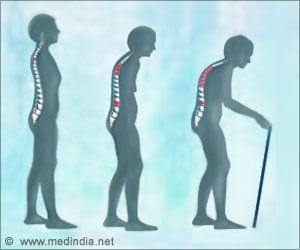
Use of bisphosphonates and denosumab on a long-term basis can be more effective in treating osteoporosis among postmenopausal women.
‘Postmenopausal women with osteoporosis need to be on a long-term treatment plan to treat osteoporosis.’





The presentation at The North American Menopause Society (NAMS) Annual Meeting in Philadelphia presented the new evidence about the long-term effectiveness and safety of treatment with bisphosphonates and denosumab.Bisphosphonates and denosumab are the most commonly prescribed treatments for osteoporosis. Protection from fractures occurs within the first few months of treatment and persists as long as treatment is continued. Upon stopping bisphosphonate therapy, protection from fractures is gradually lost over three to five years.
Treatment for more than three years has been associated with an increasing risk of unusual or "atypical" fractures of the femur (thigh bone). After five years of treatment, the risk of these atypical fractures is about 20 per 100,000 patients and increases to about 1/1,000 patients after eight to ten years of treatment.
The combination of increased risk of atypical fracture along with a relatively slow offset of the protection from fractures due to osteoporosis led to the confusing concept of a "bisphosphonate holiday."
The American Society for Bone and Mineral Research has recently provided clear recommendations about "bisphosphonate holidays." After three to five years of bisphosphonate treatment, a patient's risk of fracture should be reevaluated.
Advertisement
For patients whose risk of fracture is lower, stopping treatment for two to three years (the "holiday") can be considered but is not mandatory.
Advertisement
"Because protection from fractures disappears quickly if denosumab treatment is stopped, and since there are no currently known safety issues that limit the duration of denosumab therapy, there is no justification for a drug holiday with this treatment," says Dr. Michael McClung of the Oregon Osteoporosis Center in Portland, Oregon, who will be presenting his recommendations on long-term osteoporosis therapy at the NAMS Annual Meeting.
"Just as we do not recommend stopping treatment for high blood pressure or diabetes, it is necessary to have a long-term treatment plan for postmenopausal women with osteoporosis if the benefits of our therapies are to be realized."
"Prevention of osteoporosis should be a goal for those treating menopausal women, as up to 20 percent of bone loss occurs within the first five years of menopause. Once diagnosed with osteoporosis, the goal becomes lowering the risk of fractures as fractures can be life changing or life limiting. This presentation will offer valuable insights about the need for long-term treatment and will change the way health care providers approach long-term osteoporosis management," says Dr. JoAnn Pinkerton, NAMS executive director.
Drs. McClung and Pinkerton are available for interviews before the presentation at the Annual Meeting.
Source-Eurekalert