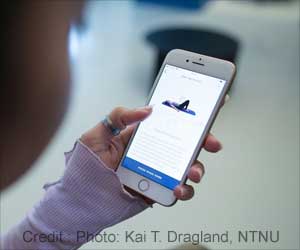
With a view to reduce the overdoses, deaths and health care costs associated with abuse of opioids and other prescription drugs, the medical insurers use prescription monitoring data

The report, available online, describes the proceedings of a December 2012 meeting of more than 75 medical insurers, federal agency heads and state PDMP administrators, who explored the value and feasibility of PDMPs sharing its prescription data with third party payers.
"This report documents the emerging consensus among leaders in the insurance and workers' compensation industry that knowing the full prescription history of an insured patient will help to provide safe and effective care and keep costs under control," said John Eadie, PDMP Center of Excellence director.
The meeting was convened by the Center of Excellence as called for by the Office of National Drug Control Policy in its 2011 Prescription Drug Abuse Prevention Plan. It was funded by a grant from the U.S. Department of Justice, Bureau of Justice Assistance Harold Rogers Prescription Drug Monitoring Program, which develops and encourages the adoption of PDMP best practices.
"With the support and expertise of the PDMP Center of Excellence and the PDMP Training and Technical Assistance Center at Brandeis University, almost every state in the country has a prescription drug monitoring program," said Congressman Hal Rogers of Kentucky. "These important tools serve the dual function of promoting good medicine and effective law enforcement, and as co-chairman of the Congressional Caucus on Prescription Drug Abuse, I am heartened by efforts to expand access to PDMPs so that we can prevent the abuse and misuse of powerful medications."
As detailed in the report, meeting participants agreed that data sharing between PDMPs and third party payers would significantly enhance insurers' capability to monitor prescribing of opioids and other commonly abused prescription drugs, permitting better detection of inappropriate prescribing and dispensing. Workgroups at the meeting formulated data sharing policies and procedures for consideration by regulatory agencies.
By enabling insurers to see their enrollees' activity beyond their respective health plans, PDMP data also would provide payers with efficient—and most importantly with respect to patient safety—early identification of unscrupulous or otherwise dangerous controlled substance prescribing and dispensing.
"Prescription drug diversion is a serious problem across the U.S. that puts lives in jeopardy and costs consumers and insurers billions of dollars each year," added Dennis Jay, executive director of the Coalition Against Insurance Fraud.
"Sharing prescription monitoring data will help public and private insurers better detect abuse and fraud involving prescription drugs, and ultimately save money and lives."
The report will be discussed at the National Rx Drug Abuse Summit in Atlanta, Tuesday, April 22, 1:45-3 p.m., during the panel presentation on "PDMP Coordination with Third-Party Administrators."
Source-Eurekalert
 MEDINDIA
MEDINDIA


 Email
Email