New research finds that the cholesterol- lowering drug, simvastatin, can affect the sleeping patterns of some patients.
New research finds that the cholesterol- lowering drug, simvastatin, can affect the sleeping patterns of some patients.
The study, presented at the American Heart Association’s Scientific Sessions 2007, involved 1,016 healthy adult men and women.The volunteers were tested for six months in a randomized, double-blind, placebo-controlled trial using simvastatin, given at 20 milligrams (mg), pravastatin at 40 mg, or a placebo. The research did not include patients with heart disease or diabetes due to concerns about assigning these people to placebos.
The researchers assessed the outcomes with the Leeds sleep scale, a visual analog scale of sleep quality, as well as a rated the scale of sleep problems. Both scales were measured before and during treatment.
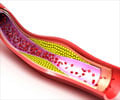
The study compared two types of cholesterol-lowering drugs called statins — simvastatin, which was lipophilic (soluble in fats), and pravastatin, which was hydrophilic (soluble in water).
They found that simvastatin affected patients’ sleep patterns. This the researchers say, is because simvastatin is fat soluble and can thus more readily penetrate cell membranes and cross the blood brain barrier into the brain. The brain controls sleep, and many of the brain’s nerve cells are wrapped in a fatty insulating sheath called myelin.
“The results showed that simvastain use was associated with significantly worse sleep quality. A significantly greater number of individuals taking simvastatin reported sleep problems than those taking either pravastain or the placebo,” said Beatrice Golomb, M.D., lead author of the study and an associate professor of medicine and family and preventive medicine at the University of California at San Diego School of Medicine.
Advertisement
“Several small studies were done early on, including those focused on lipophilic versus hydrophilic statins. “Most (researchers) didn’t see a difference in sleep, but they had short durations of follow-up and enrolled just a handful of people — often fewer than 20, which was not enough to see a difference unless it was very large. “One of these studies did report a significant difference between pravastatin and simvastatin. But without more and bigger studies, an effect was not considered to be established. “Those who reported developing much worse sleep on study medication also showed a significant adverse change in aggression scores compared to others, we should also point out that although the average effect on sleep was detrimental on simvastatin, this does not mean that everyone on simvastatin will experience worse sleep,” said Golomb.
Advertisement
Source-ANI
ANN/C