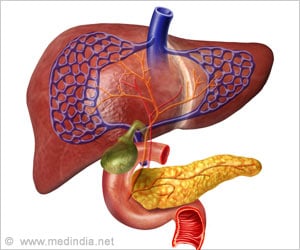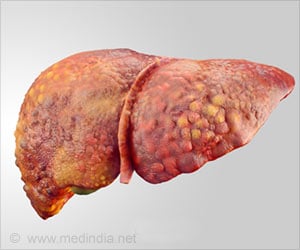
‘Norfloxacin administration for 6 months was associated with a reduced risk of death and infection at 6 months in patients with Child-Pugh class C cirrhosis.’
Tweet it Now
The French study demonstrated that at 12 months, following 6 months after termination of treatment, the cumulative incidence of death was similar between those treated with norfloxacin and those treated with placebo. However, the infection rates remained lower in the norfloxacin group at 12 months. Patients with advanced liver disease who have cirrhosis have differing prognoses. The Child-Pugh classification system, which is used to estimate prognosis in cirrhosis, rates levels of cirrhosis from A to C, with C being the most advanced cases. Child-Pugh class C indicates that the person has decompensation of the liver,1 which is a life threatening condition in which extensive scarring of the organ results in its inability to function properly.2 Decompensated cirrhosis is a leading reason for liver transplantation. Over 8,500 people in Europe3 and over 16,000 people in the United States are waiting for a liver transplant, with this number expected to increase.
"This study shows that long-term oral antibiotic therapy may improve the prognosis of patients with life-threatening liver disease. However, overuse of broad spectrum antibiotics is a subject that has been thoroughly debated over the years," said Dr Richard Moreau, Beaujon, Hospital, Clichy, France, and lead author of the study. "The results from this study provide evidence that 6 months of norfloxacin therapy reduces the risk of infections and death in the short-term, but not in the longer-term."
This randomised, placebo-controlled, phase 3 trial assigned 291 patients with Child-Pugh class C cirrhosis to receive either a 400mg norfloxacin tablet or placebo once a day for 6 months. Patients were followed up for an additional 6 months for infections, death and other liver-related complications.
After 6 months of treatment, fewer patients had died in the norfloxacin group than the placebo group (22 [15.3%] versus 36 [24.5%]). Seventeen (11.8%) patients had received a liver transplant in the norfloxacin group compared with 15 (10.2%) in the placebo group. At 6 months follow-up, the cumulative incidence of death was lower in the norfloxacin than placebo group (15.5% versus 24.8%), although at 12 months the cumulative incidence of death was similar in the two groups. At 6 months follow-up, fewer patients receiving norfloxacin had developed an infection compared with the placebo group (30 [20.8%] versus 46 [31.3%]). The cumulative incidence of infection at 6 months was lower in the norfloxacin group, and at 12 months remained lower compared with the placebo group. The cumulative incidence of any other liver-related complication was similar in the two groups at both 6 and 12 months.
Advertisement
Source-Eurekalert