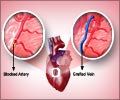
Currently, 40 percent of all patients undergoing CABG suffer from diabetes, and this number is quickly rising. Traditionally these patients have more complications following surgery, including greater risk of heart attacks, more wound infections and reduced long-term survival.
Maintaining serum glucose between 120-180 mg/dl with continuous insulin infusions decreases morbidity in diabetic patients undergoing CABG. Prior studies in surgical patients requiring prolonged ventilation suggest that aggressive glycemic control (less than 120 mg/dl) may improve survival. However, its effect in diabetic CABG patients is unknown.
Eighty-two diabetic patients undergoing CABG were prospectively randomized to receive either aggressive glycemic control or moderate glycemic control using continuous intravenous insulin solutions beginning at anesthesia and continuing for 18 hours after surgery.
According to BMC cardiothoracic surgeon Harold Lazar, MD, who authored the presentation, there was no difference in the incidence of major adverse effects between the two groups. "Aggressive glycemic control did not result in any significant improvement of clinical outcomes than can be achieved with moderate control," said Lazar, who is also a professor of cardiothoracic surgery at Boston University School of Medicine "Although aggressive glycemic control did increase the incidence of hypoglycemic events, it did not result in an increased incidence of neurological events," he added.
Advertisement