About one in 3,000 live births in the United States result in the baby having neonatal HSV; it is very rare, but it can be devastating, Kimberlin says.
Previously, the Collaborative Antiviral Study Group (CASG), a National Institute of Allergy and Infectious Diseases-sponsored organization housed at UAB and led by UAB researcher and professor Richard J. Whitley, M.D., discovered that babies treated intravenously with the antiviral drug acyclovir had improved mortality. But the CASG suspected that HSV could still be causing problems for these infants, and that additional doses of acyclovir might provide additional benefit.
Our thought was there might be ongoing damage, a sub-clinical replication of the virus within the brain, and that damage might result in worse outcomes over time, says Kimberlin, who is a co-principal investigator for the CASG and lead author of the new study.
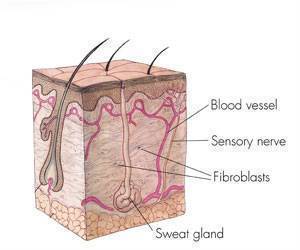
In two parallel, identical, placebo-controlled trials, 19 academic medical centers involved in the CASG, including UAB, enrolled 74 infants with HSV disease. The groups were separated into those with central nervous system (CNS) involvement and those with skin, eye and mouth disease. Babies with CNS involvement can suffer brain damage; babies with skin, eye and mouth, while neurologically unharmed, are affected by skin lesions.
The babies completed the typical course of parenteral acyclovir immediately after symptoms of HSV infection were identified. They were then given an oral dose of acyclovir for six months. In both trials, the babies were assessed through 12 months of age. The researchers used the Bayley Scales of Infant Development to assess the neurological outcomes.
Advertisement
The relative rarity of HSV transmission to infants, Kimberlin notes, made it difficult to find enough babies to enroll in the trial; in fact, the results have been more than a decade in the making. Twelve years later, we found that when you give oral acyclovir to babies for six months, they have better neurologic outcomes compared to the babies randomized to placebo, Kimberlin says.
Advertisement
The researchers say the likelihood of having a better outcome was higher if the oral acyclovir treatment was started immediately following the intravenous therapy. But if HSV had already created significant damage, the oral medication could not reverse it.
“Even taking the therapy for six months cannot undo any injury to the brain that has already occurred,” Kimberlin says.
Kimberlin adds that not all women who have had a history of genital herpes will pass the virus to their baby. The women most at risk of doing so are those who acquire the virus for the first time near the end of their pregnancy. In women who have active genital herpes, a cesarean delivery usually is performed, according to the Centers for Disease Control and Prevention.
Source-Newswise