Researchers at the Oxford University claim to have developed a new IVF screening technique that could double the success rates for some women.
Defects in the number of chromosomes in an embryo is believed to be a major cause of miscarriage, with older women being more at risk.Healthy embryos should have 23 pairs of chromosomes, but some have more or less than this number.
The new technique called comparative genomic hybridisation (CGH) is the most advanced way yet of counting chromosomes.
The available techniques mean that only half of the embryo's DNA can be checked for problems before being implanted in the womb.
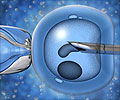
However, the new method can check 23 pairs of chromosomes, meaning many more defects can be found and those embryos discarded so only the perfect ones with the best chance of creating a baby are then implanted in the womb.
The latest study has been presented today at the American Society of Reproductive Medicine conference in San Francisco.
Advertisement
The embryos were allowed to mature in the lab for slightly longer than normal and then screened. Of the 23 patients, 21 had a positive pregnancy test and 18 have so far carried the baby past the first trimester, which is when most miscarriages occur.
Advertisement
The chances of the embryo implanting in the womb with this technique is 62 per cent double the normal chances for this age group.
The researcher who has developed the new technique is planning to offer it in the UK for about 2,000 pounds, on top of the fee for IVF, and around the same as standard screening techniques.
"The pregnancy rates we've got so far are absolutely phenomenal," Guardian.co.uk quoted Dr Dagan Wells at Oxford University and Reprogenetics UK, who led the study, as saying.
Source-ANI
SK