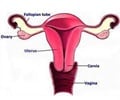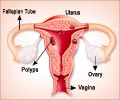
For two years, Ghamande and his team followed a small group of high-risk patients with early-stage endometrioid adenocarcinoma, a common subtype of endometrial cancer, and those with atypical endometrial hyperplasia, or thickening of the uterine lining, which can lead to cancer. Patients were treated with an intrauterine device that releases the progestin levonorgestrel, successfully used for the past decade as a contraceptive.
The endometrial stripe, or thickness of the endometrium, was measured with transvaginal ultrasound before the study and at the three- and six-month marks. The stripe's progressive thinning at each stage demonstrated the effectiveness of the treatment. Subsequent endometrial biopsy found reversal of abnormal cell growth, known as neoplastic changes, in all patients.
Ghamande's group also analyzed 13 published studies and found a complete pathological response in 91.3 percent of cases, with no progression of disease, confirming their findings. The study also validated use of transvaginal ultrasound, commonly used to diagnose endometrial cancer, as a useful follow-up tool in assessing endometrial cancer treatment.
"Thirty to 35 percent of women with hyperplasia will go on to develop endometrial cancer, and in 30 percent of these cases, women will present with a co-existing cancer," said Ghamande. "Traditional treatments can result in postoperative complications and morbidity, not only in patients at high risk. But we may succeed in establishing a lower-risk and more cost-effective way of managing this cancer in all women."
"Identifying better treatments for cancer is the most important goal of our cancer research center," said Dr. Samir N. Khleif, Director of the GHSU Cancer Center. "Studies such as Dr. Ghamande's are changing the landscape of cancer care today, both here in Georgia and around the world."
Advertisement
Advertisement