‘Medication is often lifelong, and long-standing treatment can eventually lead to complications such as osteoporosis, pneumonia and gastrointestinal infection.’
Tweet it Now
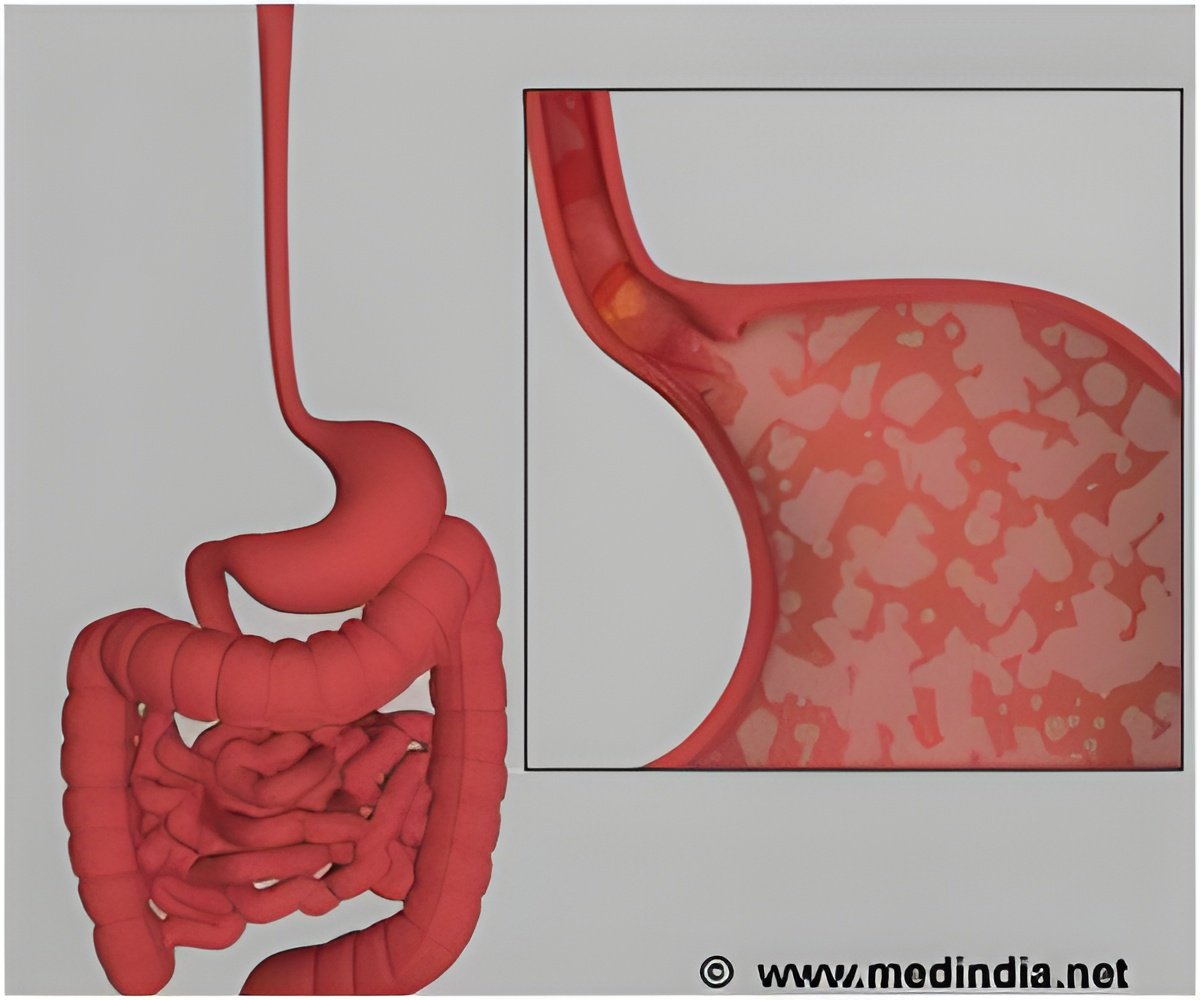
Severe, recurrent heartburn, or reflux, affects between 10 and 20 per cent of the adult population. The most common treatment is medication that reduces the acidity of the stomach, which alleviate the symptoms for most people.Alternatively, sufferers can undergo anti-reflux surgery, whereby the contents of the stomach are prevented from entering the oesophagus by a mechanical valve implanted through keyhole surgery.
However, such operations have declined since the turn of the 2000s due to the greater efficacy of the medications and to the risk of complications and relapse. Older studies of post-operative relapse have been small and provided conflicting results; some, however, have indicated a very high risk of relapse.
To obtain a clearer understanding of the risk of relapse after anti-reflux keyhole surgery, researchers at Karolinska Institute have carried out a large study in which they followed up all adult reflux patients who underwent such an operation in Sweden between 2005 and 2014.
They found that 18 per cent of the 2,655 patients had suffered a relapse, which is lower than in most of the earlier studies. Of these, 84 per cent were put on long-term medication, with the remainder having a second operation.
Advertisement
The risk of reflux relapse was higher in women, elderly people and people with other diseases; the risk was lowest amongst healthy men below the age of 45.
Advertisement
Medication is readily available and effective at alleviating symptoms, but does not treat the underlying disease. Medication is often lifelong, and long-standing treatment can eventually lead to complications such as osteoporosis, pneumonia and gastrointestinal infection.
"The operation requires no lengthy hospitalisation and is a one-off, but it does carry a risk of complications and relapse," says professor Lagergren. "Previous comparisons of medication and surgery have shown that life quality is better after surgery, and surgery is judged likely to be more cost-effective in the long run."
Source-Eurekalert