VIB researchers of Ghent University, in collaborated with research centers in Beijing and Shanghai in China, and have developed a test to detect liver cancer in an early stage. This innovative test made possible accurate detection of liver cancer in over 50% of the cases for which earlier diagnostic tests could not detect it accurately. This new test is quite simple as it requires only a small blood sample.
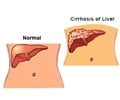
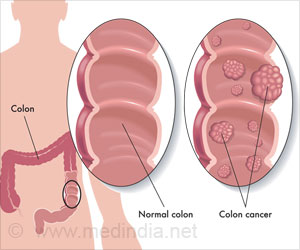
Detection of liver cancer is not very easy. It has become a major cause of death in Asia and Africa with growing incidence in the western countries.Liver cancer Hepatocellular carcinoma (HCC) is the most prevalent primary liver cancer. The disease most often appears following a chronic inflammation of the liver as a consequence of a hepatitis B or C virus infection or cirrhosis of the liver. Cirrhosis of the liver comprises a group of liver diseases in which the normal liver cells become damaged and are replaced by scar tissue.
This reduces the amount of healthy liver tissue, and the accumulation of scar tissue disrupts the development and functioning of this complex organ. Cirrhosis of the liver has various causes, including: excessive use of alcohol, chronic viral hepatitis B, C and D infections, diseases of the bile ducts, and parasitic infections.
Half a million patients die every year in China because of cirrhosis of the liver or liver cancer. 60% to 80% of the patients with liver cancer have a previous history of cirrhosis of the liver. In Belgium as well, 350 new cases of liver cancer occur each year.
Transplantation often offers the only possible remedy. Detection methods that would detect HCC in an early stage would save many lives.
Current detection methods Methods of detecting malignant growths are often based on the concentration of particular substances – called 'markers' – present in the blood. For the detection of HCC, only one marker (AFP) is generally used. However, this marker has a low specificity and is frequently inadequate because of false-positive results.
Advertisement
By examining blood concentrations in Chinese patients with cirrhosis of the liver due to a hepatitis B virus infection, they found that the quantities of two particular sugar groups that appear on the blood proteins varied according to the stage of the disease.
Advertisement
Promising results When the AFP test is used in combination with the new test, the accuracy of HCC diagnosis rises dramatically. The new test succeeds in detecting liver cancer in more than half of the patients with cirrhosis of the liver for which the AFP test provides no answer.
This test would allow frequent and non-invasive analyses to be carried out on cirrhosis patients, which would enable scientists to detect liver cancer in an earlier stage and to closely monitor the development of the disease.
At the moment, the researchers are working on implementing this test for the diagnosis of liver disease in compliance with clinical practice. The new results concerning HCC diagnosis provide an extra incentive for pursuing this development as intensively as possible.
Source-Eurekalert
BIN/J