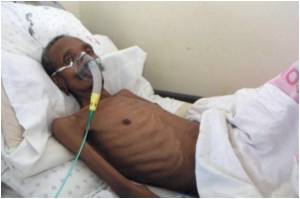
Social and economic determinants at individual, household and community levels affect a person's vulnerability to TB. Special situations such as massive population movements - the displacement of people and refugee flows - and living or working in particular conditions also increase the risk of a person contracting TB.
In developed countries, ethnic minorities and other marginalized communities are at a greater risk of contracting the disease. In Canada for instance, indigenous communities have a 20 to 30 times higher TB burden than majority ethnic groups, Dr Kim Barker and Dr Anne Fanning from Stop TB Canada had said to CNS during the 38th Union World Conference on Lung Health in 2007.
Factors such as social isolation, reduced access to health services, a lack of trust in the health system and lack of organized community voices exacerbate the risk of TB spreading. But by identifying these vulnerabilities to TB, control strategies can become more focussed on reaching the people most in need.
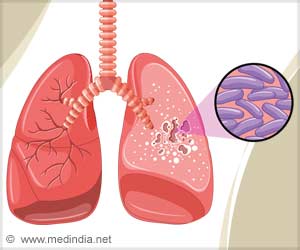
TB is transmitted more readily in conditions such as overcrowding, where there are inadequate ventilation and malnutrition. Improvements in socio-economic conditions will therefore lead to reductions in TB incidence. This should also lead to improvements in access to care, its rational use and quality of care.
About one billion people live in urban slums and over the next 30 years that number is expected to double. In the poorest countries, about 80% of the urban population lives in slums. The poor socio-economic and environmental conditions that characterize the slums facilitate the transmission of many communicable diseases including TB. The burden of TB is often far greater in these urban settings than in rural areas.
Advertisement
Poor TB patients in developing countries are mainly dependent on daily wages or income from petty trading and have no security of income or employment. In many studies people with TB have been found to have borrowed money, used transfer payments or sold assets because of their illness.
Advertisement
At this TB and poverty consultative workshop, listening to the experiences from those fighting TB on the frontlines in high burden settings like in Nepal, Thailand and India, and from five states in India, it was evident that even where Directly Observed Treatment Shortcourse (DOTS) programmes are well established, patients with TB face substantial costs prior to diagnosis. While aggregate costs for poor people tend to be lower than for those from a higher socio-economic position, the costs as a proportion of income is much higher for the poor.
Experiences from other programmes like HIV show that it was usually health-care volunteers or members from affected communities that reached the most marginalized communities, providing them with TB and HIV care and treatment services. Home-based care (HBC) experiences for people living with HIV in most hard-hit communities provide learning lessons.
Poverty has played a leading role in accelerating the spread of TB. The poor are at the greatest risk for tuberculosis because of poor housing, poor diet, poor education and risky behaviour.
Let's combat TB by addressing the barriers faced due to poverty such as infrastructural, housing, employment, educational and nutritional deficiencies.
Source-Medindia