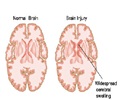
Dystonia causes muscles to contract, with the affected body part twisting involuntarily and symptoms ranging from mild to severe. The Food and Drug Administration approved deep brain stimulation as a therapy for certain treatment-resistant dystonias in 2003 after approving it for essential tremor in 1997 and Parkinson's disease in 2002. The procedure recently was approved on a limited basis for obsessive-compulsive disorder.
"We knew from earlier work that younger patients with shorter disease duration had better clinical outcomes in the short term. Now we know they fare best in the long term, as well. Our study uniquely showed that age and disease duration play complementary roles in predicting long-term clinical outcomes. The good news for older patients is that while they may not see the rapid gains of younger patients, their symptoms may gradually improve over several years," said Tagliati, who is considered one of the world's top experts on the therapy.
The study involved 44 patients with generalized dystonia ranging in age from 10 to 59 years, with a midpoint of 31 years. Disease duration ranged from two to 42 years, with a midpoint of 15 years. There were three key clusters of patients whose medical records were analyzed:
- Those younger than 27 and who had suffered from dystonia fewer than 17 years (17 patients)
- Those older than 27 but who had suffered fewer than 17 years (eight patients)
- Those older than 27 and who had suffered more than 17 years (19 patients)
Advertisement
- Every patient experienced overall improvement in motor function – their ability to control muscles and movements -- after surgery and device activation. All ratings of individual body regions or functions such as speech (sub-scores) improved significantly at one year. Further gains were seen at three years.
- Three patients' overall outcomes declined, with mild worsening of some symptoms between years one and three.
- Five more patients had some worse sub-scores at year three but continued to show overall improvement and did not return to their pre-treatment impairment levels.
- Patients older than 27 at the time of surgery showed an additional 10 percent average improvement between years one and three of therapy.
- Thirty-two patients were taking prescription drugs before surgery but this number declined by 52 percent at year one and 80 percent at year three.
Advertisement
Source-Eurekalert