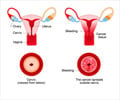
Cervical screening in women aged 20-24 has little or no impact on rates of invasive cervical cancer up to age 30, concludes a study published on bmj.com today.
A second study shows that the risk of developing pre-cancerous lesions on the surface of the cervix (known as cervical intraepithelial neoplasia or CIN) is much higher in women with persistent human papillomavirus (HPV) infection, especially the high-risk HPV types 16 and 18.Together, these findings highlight the challenges faced by policy makers in balancing the benefits and harms of screening women at different ages and at different levels of risk.
In 2003, cervical screening in England was moved to start at age 25 as it was felt it did more harm than good in younger women. But recent public controversy has led the government to review whether women aged 20-24 should be offered smear tests, as they are in Scotland, Wales and Northern Ireland.
So researchers at Queen Mary, University of London set out to study the impact of screening on risk of cervical cancer at different ages. They identified 4,012 women aged 20-69 diagnosed with cervical cancer between 1990 and 2008 and a matched group of 7,889 healthy controls of the same age and living in the same area.
They found no evidence that screening women aged 22-24 reduced the incidence of cervical cancer over the next five years (at ages 25-29).
Screening was associated with a 60% reduction of cancers in women aged 40, increasing to 80% at age 64. Screening was particularly effective in preventing advanced stage cancers. However, in younger women, the effect of screening was substantially and significantly less.
Advertisement
In fact, a careful review of the screening histories of women aged 20-24 with a diagnosis of cancer suggests that few, if any, of the cancers occurred through a lack of screening, say the authors. Indeed, only five of 73 women had not been screened in the previous six years.
Advertisement
Policy decisions should be based on balancing the benefits and harms of screening and the need to take into account the underlying risk of cervical cancer at different ages, write the authors. “We have provided more accurate estimates of the benefits of cervical screening in different age groups, which should aid policy makers in making their decisions,” they conclude.
In an accompanying editorial, three cancer specialists suggest that in many developed countries the low incidence of invasive cervical cancer and the lack of effectiveness of screening in young women indicate that screening should not start before the age of 25. At younger ages, the main challenge is to find the progressive lesions and to avoid treating the remaining lesions, given that treatment may be harmful to future reproductive health, they conclude.
Source-BMJ
LIN