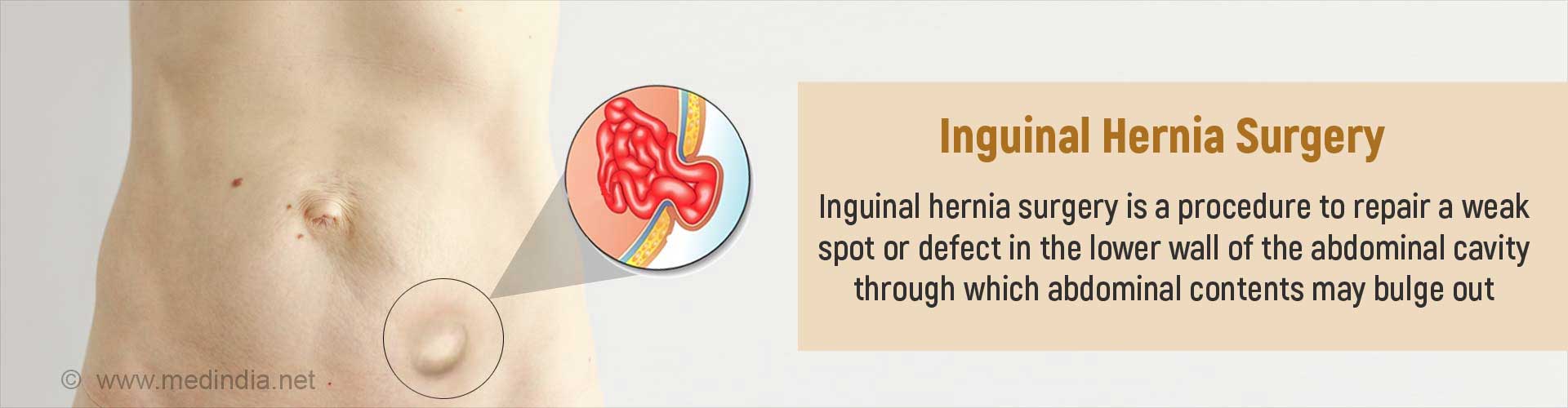
What is Inguinal Hernia Surgery?
Inguinal hernia, also called as groin hernia is the bulging of soft tissue through a weakened spot (defect) in the lower abdominal wall, causing a lump in the inner aspect of the upper thigh. For example, a portion of the small intestine can bulge-out underneath the skin of the groin producing a localized swelling.
This defect can be rectified by performing inguinal hernia surgery, also known as inguinal hernia repair.
The prevalence of abdominal wall hernias is estimated to be 1.7 to 4%. Inguinal hernia is the most common, which accounts for almost 75% of all abdominal wall hernias. The life time risk of inguinal hernia is 27% in men and 3% in women.
Anatomically, the groin or inguinal region is the area between the lower abdomen and the thigh.
The abdominal cavity is a large cavity between the chest and the pelvic region housing several important abdominal organs. The lowermost portion of the abdominal cavity corresponds to the inguinal region. The abdominal cavity is protected and bounded by a wall consisting from below upwards of peritoneum (coverings of the abdominal organs), layers of fascial tissue, abdominal muscles, subcutaneous tissue and the covering skin.
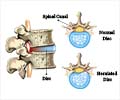
Normally, the abdominal muscles are usually strong enough to keep the internal organs in place. However, if a weakness develops in the wall, the structures within the cavity may protrude through the musculature resulting in a hernia.
- Inguinal hernia surgery is indicated for relieving pain and other symptoms or when the herniated portion of the small intestine cannot be pushed back using a support such as hernia belt.
- The herniated portion of the small intestine may become stuck in the inguinal canal (strangulation), which can result in oxygen cut-off to the affected portion, leading to further complications.
- In case of children, surgical repair is the norm.
- Surgical repair is recommended for femoral hernia in women. Inguinal hernia is usually rare in women.
The following factors should be considered before doing the surgery:
- Age of the patient
- Gender of the patient
- Health status of the patient
- Type of hernia location, side, duration, and recurrence
Only minimal preparation is needed for inguinal hernia surgery. These may include the following to assess the general condition of the patient and heart and lung function to withstand surgery:
- Routine blood tests
- Electrocardiography (ECG)
- Chest X-ray
- Stopping over-the-counter (OTC) medications, including painkillers like aspirin and ibuprofen to reduce risk of hemorrhage during surgery
On the day of the surgery, you will arrive at the hospital after overnight fasting. You will change into a hospital gown and your vital parameters will be checked. The groin area will be shaved and scrubbed to reduce the chances of infection. The area will then be draped before commencement of the surgery.
Types of Anesthesia: Open inguinal hernia surgery can be carried out under general anesthesia (GA), regional (epidural) anesthesia, or local anesthesia, while laparoscopic (closed or keyhole) inguinal hernia surgery is carried out under GA.
Types of Surgery: The common surgical methods for repairing an inguinal hernia include the following:
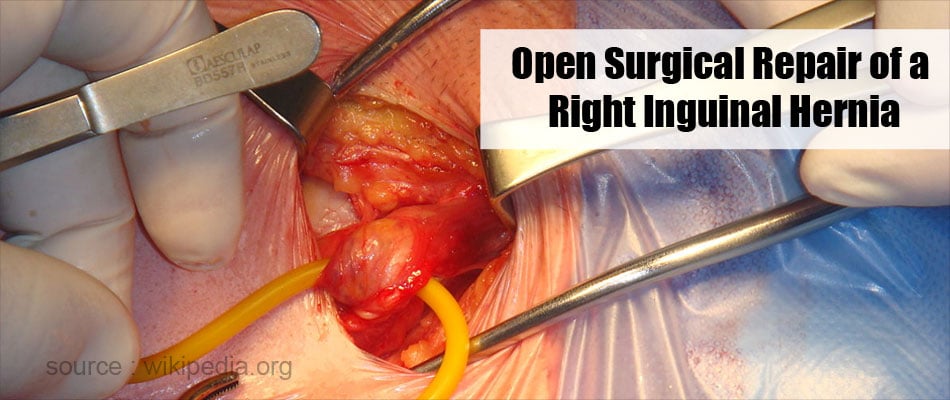
- Open Inguinal Hernia Surgery: These are again sub-divided into three types, which include herniotomy, herniorrhaphy, and hernioplasty. This type of surgery is usually performed in case of large hernias, where the surgeon makes a large incision in the abdomen to gain access to the herniated area.
![Open Inguinal Hernia Surgery Open Inguinal Hernia Surgery]()
- Herniotomy involves the excision of the band of tissue that constricts the protruding structures and pushing them back into place (reduction of hernia)
- Herniorrhaphy involves a standard herniotomy procedure described above followed by suturing the defect in the abdominal wall. The Bassini, Shouldice, and Darning repairs are examples of herniorrhaphy.
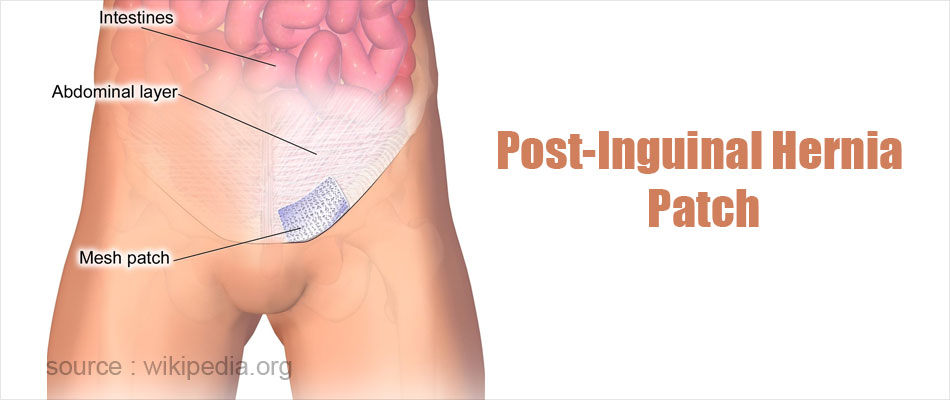
- Hernioplasty involves giving additional reinforcement to the abdominal wall defect after repair using autogenous tissue i.e. the patients own tissue or with a heterogeneous material such as a Prolene® mesh made of polypropylene. The Lichtenstein tension-free mesh repair is an example of hernioplasty and is currently one of the most popular techniques among surgeons for inguinal hernia repair.
Post-operative pain, soreness, and scarring can be present after open inguinal hernia surgery. Moreover, the recovery time may be prolonged.
- Laparoscopic (Closed or Keyhole) Inguinal Hernia Surgery: This is a minimally invasive surgical method that is recommended for small hernias. In this procedure, the surgeon makes several small incisions in the abdomen, through which some special instruments are inserted. One of these is a thin tube that has a miniature camera fitted at its tip. This is called a laparoscope, through which the surgeon is able to visualize the surgical field and carry out the operation. The operation is carried out using the other instruments like electrocautery knives and miniature scissors. Sometimes, a Prolene® mesh is inserted to increase the strength of the weakened abdominal wall through which the herniation occurred. Following the operation, the external incisions are closed with sutures.
Since laparoscopy is minimally invasive, there is much less scarring, lesser post-surgical pain and a quicker recovery.
Inguinal hernia surgery is generally very safe. However, as with any surgery, there is always a risk of complications. Some of these include the following:
- Infection: This is a common complication of surgery in general. This will become evident if the wound area is abnormally swollen, warm and red. Proper preventive measures before, during and after surgery can reduce the chances of infections appreciably.
- Pain: This is very common after surgery. As the wound heals, the pain usually subsides, with the area remaining sore till complete healing occurs. Pain is generally more in case of the open type surgery and much lesser in case of laparoscopic surgery.
- Thrombosis: There is a chance of formation of blood clots, especially in the lower extremities due to being immobilized for a long time under the influence of anesthesia.
- Nerve Damage: Since the groin is innervated by several fine nerves, there is a chance of nerve injury during the surgery or afterwards when the staples / sutures are inserted. Neuropathy is characterized by sharp, piercing or tingling pain.
- Recurrence: There is a chance of recurrence of the hernia, especially if the muscles of the abdominal wall where the herniation occurred are too weak to support the internal stitches. The chances of recurrence can be reduced appreciably by using a mesh for reinforcement.
- Miscellaneous Surgical Complications
Following any surgery, especially to the abdomen, the following post-operative complications may occur:
- Fever
- Pain, swelling, redness, bleeding at the incision site
- Nausea and vomiting
- Urination problems
- Difficulty in bowel movements