- Clinical applications of induced hypothermia - (http://ceaccp.oxfordjournals.org/content/6/1/23.full)
- Therapeutic Hypothermia After Cardiac Arrest - (http://circ.ahajournals.org/content/108/1/118.full)
- Sudden Cardiac Death in India : A Growing Concern - (http://www.japi.org/december_2014/006_ra_sudden_cardiac_death.pdf)
- Therapeutic Hypothermia for Neuroprotection - (http://www.ncbi.nlm.nih.gov/pmc/articles/pmc4056415/)
- Therapeutic Hypothermia After Cardiac Arrest: Best Practices 2014 - (https://my.clevelandclinic.org/ccf/media/files/nursing/2014-dicc-handouts/session8_1030_1103_klein.pdf?la=en)
What You Ought to Know About Therapeutic Hypothermia?
Therapeutic hypothermia is a deliberate reduction of the body temperature that may be administered to patients who do not regain consciousness even after circulation is resumed following a cardiac arrest.
Temperature maintained during therapeutic hypothermia: 320C - 350C
Regulation of Body Temperature:
The human body regulates body temperature to ensure optimum functioning of organs and metabolic processes. At lower temperatures, enzyme production is lowered, affecting the metabolic processes.
During hot weather, body temperature is maintained by:
- Perspiration - Sweating aids in heat loss
- Conduction/ Convection of heat is used to maintain body temperature
- Radiation of heat
During cold weather, body temperature is maintained by:
- Shivering, that promotes heat production by the muscles
- Constriction of blood vessels to the skin to reduce the transfer of heat from within the body
What is Hypothermia?
Hypothermia is a condition where the body temperature is lowered to below 350C. This can be a gradual process or could be due to a sudden decrease like an accident that leaves an individual stranded in heavy snow.
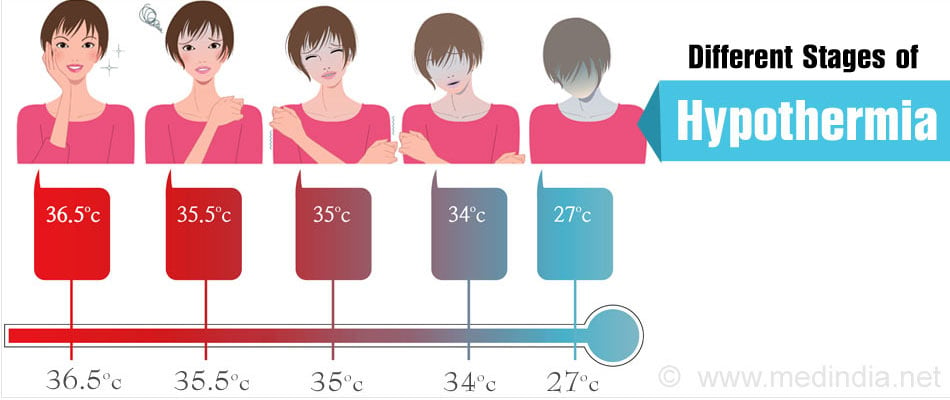
As the temperature decreases, the symptoms of the condition become more severe, requiring immediate medical attention. There are three different stages of hypothermia, depending upon the temperature:
- Mild Hypothermia: ( 32-350C) In mild hypothermia, the patient begins to shiver rapidly, but shivering stops around 330C. The person will seem quiet and withdrawn with slurred speech. The blood pressure of the patient is also lowered.
- Moderate Hypothermia: (28-320C) In moderate hypothermia, blood pressure and pulse of the patient is considerably lowered with no voluntary movements of the body. The person may turn unresponsive below 310C.
- Severe Hypothermia: (<270C) The patient appears to be dead and is unresponsive.
What is Therapeutic Hypothermia?
Therapeutic hypothermia involves the lowering of body temperature to slow down metabolic process, especially those that affect the brain triggered by a cardiac arrest that occurs outside the safety of a hospital.
Why is Cardiac Arrest Out of the Hospital Significant in India?
Statistics show that nearly 300,000 people in America suffer from cardiac arrests outside the hospital, limiting their access to immediate medical care. Only about 40% of these patients receive cardiopulmonary resuscitation which results in lower number of cardiac arrest survivors.
In India, there is a considerable delay in bringing cardiac arrest patients to the hospital.
- In North America, the time taken for a person who suffers a cardiac arrest to reach emergency unit in a hospital is between 110 and 140 minutes
- In India, the time taken for a cardiac patient to reach the emergency unit in a hospital is between 180 and 330 minutes.
The delay in transfer is due to various reasons including:
- Traffic snarls
- Long distances to reach the hospitals
- Only 5.4% of patients in India who suffer from cardiac arrest use an ambulance
- Patients first visit primary/family doctor before reaching the emergency unit of a hospital
The prolonged time increases the risk for brain damage due to lack of oxygen to the brain.
What are the Effects on the Brain after a Cardiac Arrest?
How brain damage occurs after a cardiac arrest?
- A cardiac arrest results in lowered oxygen to the brain due to lowered blood pressure/ activity of the heart.
- The low oxygen level in the brain is called hypoxia and can lead to:
- Absence of synaptic transmissions
- Cerebral edema due to damage to the blood-brain barrier.
Prolonged hypoxia in the brain can lead to increased brain damage that can even lead to brain death. When cardiac resuscitation procedures are initiated shortly after a cardiac arrest, the brain is restored with blood supply.
When blood supply and thereby, oxygen supply is restored to the brain, there is further damage caused to the brain.
- Increase in cerebral edema.
- Inflammatory pathways are initiated leading to increased damage to brain tissue.
- Initiation of chemical cascades that lead to the destruction of brain cells.
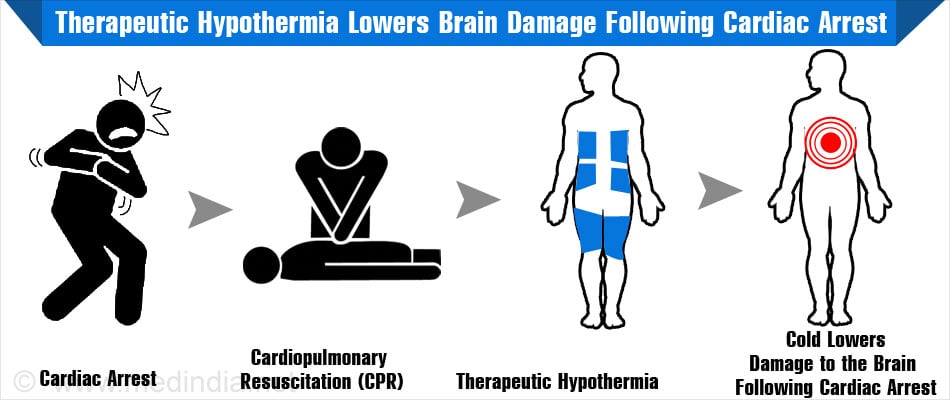
Therapeutic hypothermia is used to lower the body temperature so that
- Chances of survival after a cardiac arrest are improved due to relatively lower damage to the brain.
- Quality of life after a cardiac arrest is improved as the brain suffers less damage on recovery from cardiac arrest.
Brain damage after a cardiac arrest:
| Part of the brain | Function | Effects of hypoxia after cardiac arrest |
| Basal ganglia, caudate | Control of motor function, learning, behaviour and memory | Loss in attention, memory, dystonia and loss of motor functions |
| Hippocampus | Visual, memory, learning abilities | Memory lapses, seizure and amnesia |
| Basal cortex | Learning, language ability, consciousness, cognition and speech. | Coma, a vegetative state of the patient, seizures, impairment of speech and cortical blindness |
| Cerebellum (most importantly, the Purkinje cells) | Co-ordination, gait, cognition, balance | Dysmetria or lack of co-ordinated movement, fine motor impairment |
What is the History of Therapeutic Hypothermia?
- The first documented evidence was by Edwin Smith Papyrus, written more than 5,000 years ago.
- Hippocrates used cold packing consisting of ice and snow to lower hemorrhage in the wounded patients and for patients suffering from tetanus.
- Dr James Currie, in the late 1700 performed experiment of therapeutic hypothermia on patients to study the effect of cooling on the body, respiration and pulse.
- Napolean’s chief surgeon used cold packs to cool limbs before they were amputated, to lower pain.
- Since 1803, Russians use therapeutic hypothermia to resuscitate patients by placing them in snow.
- Sir William Osler, from Johns Hopkins University, studied the effect of therapeutic hypothermia on typhoid patients and noticed a decline in mortality from 24.2% to 7.1%.
- Dr Temple Fay in 1938 reintroduced therapeutic hypothermia to medical care by ‘cooling’ a patient with metastatic cancer and reducing pain symptoms. He was the first to discover ‘cooling blankets’, which are special insulated blankets that aid in lowering body temperature.
- In 1950, Bigelow and colleagues demonstrated the benefit of resorting to therapeutic hypothermia after cardiac arrest in animals.
- In 1958, the first published use of therapeutic hypothermia for patients in coma after a cardiac arrest was reported. The temperature of hypothermia was maintained at 330C and 6 out of the 12 patients survived.
- In 1964 Dr Peter Safar advocated the use of therapeutic hypothermia if patients did not show any central nervous system activity even after 30 minutes of resumption of blood circulation.
The use of therapeutic hypothermia was not popularly used during this period, even though studies showed their benefit, because of the side effects produced. Earlier moderate hypothermia, which is maintenance of body temperature between 33-280C was advocated, but it resulted in:
- Coagulopathy
- Arrhythmias
- Infections
In the 1980s, there was a resurgence of therapeutic hypothermia, when mild hypothermia was also found to have far reaching benefits for patients after brain injury following traumatic accidents or after cardiac resuscitation.
Bernard et al in a study on comatose patients after cardiac arrest showed that patients who were treated with therapeutic hypothermia had a 49% chance of survival while non-treated patients had 26%.
Peberdy and colleagues studied the effect of therapeutic hypothermia on out of hospital cardiac arrest patients and found that:
- Better neurological symptoms were exhibited by therapeutic hyperthermia treated patients (55%) than control patients (39%).
- 6 months mortality rate among the treated patients (41%) was lower than in the control patients (55%).
Mechanism of Action - How Therapeutic Hypothermia Protects the Brain?
Acute Phase:
This phase of therapeutic hypothermia extends from minutes to hours and it has the following benefits on brain activity:
- For every 10C drop in temperature, cerebral metabolic rate is lowered by 6 to 7%.
- Reduction in the demand for oxygen.
- Preservation of phosphates and energy.
- Prevention of acidosis.
- Improves the utilization of glucose in the brain.
- Lowers the release of excitatory amino acids (which lead to neural injury).
- Prevents synthesis of nitrous oxide mediated by glutamate.
Subacute Phase:
This phase of therapeutic hypothermia extends from hours to days. The brain may have undergone secondary injury mechanism that results in the formation of reactive oxygen species, inflammation and programmed cell death. Hypothermia will result in:
- Oxidative stress markers are reduced.
- 50% reduction in hydrogen peroxide concentrations.
- The neurons then retain viability.
- Inflammatory responses after brain injury are the leading cause of damage to brain cells, post injury. Hypothermia lowers the expression of:
- Inflammatory cytokines
- Neutrophils
- Endothelial molecules
- Monocyte infiltration
- Neural injury results in the death of cells, but hypothermia aids in release of factors that prevent death and the secretion of factors (p53) that promote repair.
- Preserves the blood brain barrier.
Chronic Phase:
This phase of therapeutic hypothermia extends from weeks to months.
- Hypothermia for 4 to 24 hours aids in post-ischemic neurogenesis and provides benefits that are not observed when conducted for 45 minutes or less.
- Lowers reactive oxygen species production.
- Restricts apoptosis (programmed cell death) and inflammation.
- Aids in neuronal cell regeneration and neuronal circuit repair.
How is Therapeutic Hypothermia Carried Out?
There are three phases involved in therapeutic hypothermia: induction or the cooling phase, maintenance and the re-warming phase.
Induction Phase:
The induction phase involves lowering of the core body temperature to the required temperature. This may be done through internal cooling or surface cooling method.
Internal cooling - In this method of cooling the body, a catheter is inserted into the femoral vein which is in the groin of the patient. This catheter is inserted till it is just below the heart in the inferior vena cava. As soon as the catheter is in position, cool fluid (40C) is injected through it to cool the blood that flows near it. The circulation of this cooled blood aids in lowering the core body temperature.
External or surface cooling method - Thigh pads and chest pads are fastened onto the patient and water tubes are attached to these pads. Cold fluid is circulated through these pads to lower temperature.
It normally takes 30 minutes to cool the body temperature by 2 to 2.50C. Sometimes, a combination of both the methods of cooling is adopted. Once the temperature is achieved, cooling blankets are placed over the patient.
Maintenance:
The temperature of the patient should be maintained between the induction phase and the re-warming phase by attaching cooling blankets placed over the patient to cooling machine.
The patient’s vitals like blood pressure, urine creatinine and electrolyte levels are monitored. Anesthesia is provided to an extent that allows neurological tests to be monitored. Shivering is controlled by providing neuromuscular blocking agents.
Rewarming:
The re-warming procedure is a gradual process and should take place over a period of 12 hours. The temperature of the cooling machine is increased slowly till the temperature is increased.
In the event of severe bleeding, active re-warming procedures are carried out which allows return to normal temperature within 8 hours.
What are the Effects of Therapeutic Hypothermia on the Organ Systems and What are the Risks?
Therapeutic hypothermia produces both positive and increases the risk for negative effects on the various organ systems.
Cardiovascular System:
- Hypothermia aids in improving left ventricular filling.
- Increases the risk for arrhythmias, which is more pronounced below 300C.
- Increases risk for cardiomyopathy.
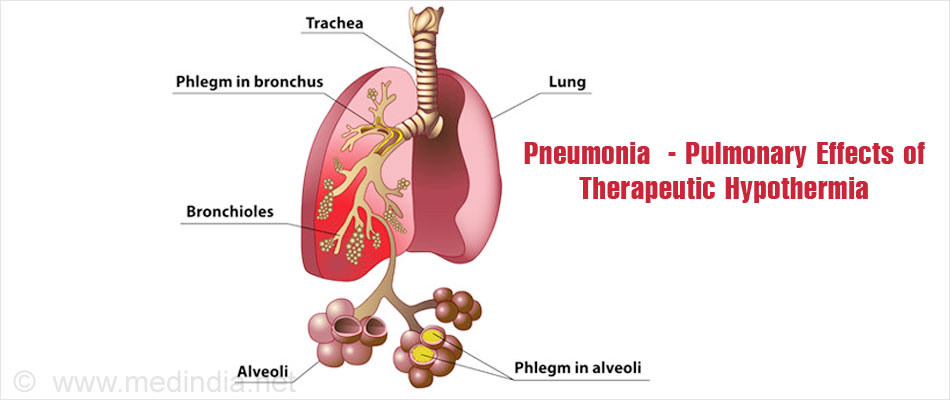
Pulmonary Effects:
- Increases risk for acute respiratory distress syndrome (ARDS).
- Decreases oxygen consumption and carbon -di-oxide production.
- Lowered inflammatory response due to hypothermia; leads to infections like pneumonia.
- Patients with decontaminated digestive tract showed lower rate of infection.
Coagulation of Blood:
- Platelet count is lowered.
- Hemoglobin levels remain the same.
- There is a low risk of bleeding in patients without a history of bleeding disorder. Patients with bleeding disorder should not be cooled lower than 350C.
Gastro-intestinal, Renal and Endocrine Effects:
- Electrolyte disorders are common.
- Potassium levels are lowered.
- Lowers insulin sensitivity.
- Delayed ileus and gastric emptying.
In patients receiving therapeutic hypothermia, there are marked changes in drug metabolism as there is a delay in drug clearance in the body. This could increase the potency of the drug as it is retained for longer periods in the body.
What are the Various Clinical Applications of Therapeutic Hypothermia?
- To prevent neural damage after cardiac arrest.
- Traumatic Brain Injury: Damages to the brain after a traumatic injury can be treated in certain cases using therapeutic hypothermia especially intra-cranial pressure elevation caused during the injury.
- Stroke: It is difficult to treat stroke patients with therapeutic hypothermia as they are awake, but there have been reported cases of benefits.
- Spinal Cord Injury: People with spinal cord injury suffer from severe neurological damages. These damages may be limited using therapeutic hypothermia.
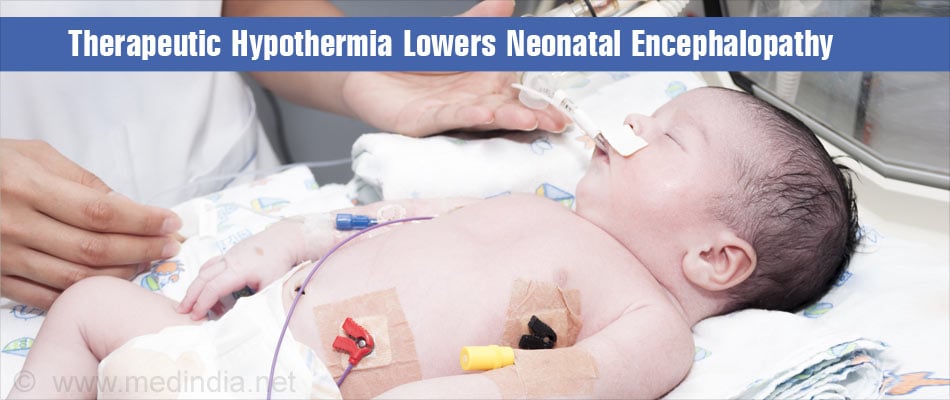
- Neonatal Encephalopathy: Neonatal encephalopathy could lead to developmental disabilities which are lowered considerably by the use of therapeutic hypothermia.