Pneumonia
Pneumonia is an infection of the lung tissue. It is usually associated with cough, sputum, fever and shortness of breath. There are various kinds of pneumonias.
In adults, most pneumonias are due to bacterial infections (the most common infectious cause of pneumonia is the bacterial Streptococcus Pneumoniae). Other bacteria, such as Mycoplasma and Legionella, as well as certain viruses, may also cause pneumonia. Fungi, and protozoa, however, may also be causes. These microorganisms have become very common as causes of pneumonia in immuno-suppressed persons, such as those with HIV infection. In children, pneumonia is most commonly caused by viruses.
The infections may not cause all of the classic pneumonia symptoms, so they are often called atypical pneumonias. Atypical pneumonias most commonly occur in individuals under 40 years of age. Also, in some instances a patient may have all of the symptoms and chest X-ray changes associated with pneumonia, but these findings may be due to a non-infectious cause such as a tumor or an allergic reaction to a drug.
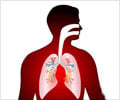
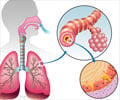
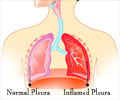
In the lungs, the microbes that cause pneumonia can lodge in the air sacs, where the oxygen is normally exchanged for carbon dioxide in the blood. There, the microbes can multiply rapidly and the air sacs may fill with fluid and with white blood cells produced by the body to fight the infection. When a lobe (major section) of a lung is affected, the infection is called lobar pneumonia. The infection is called bronchial pneumonia if it primarily affects the bronchioles (tiny air passages of a lung). Interstitial pneumonia chiefly affects the interstitium, the small spaces between the air sacs and the blood vessels.
The symptoms of pneumonias vary with the type of microbe involved and the patient's general health before the onset of the disease. In general, the symptoms of bacterial pneumonia are more severe and begin more suddenly than those of viral pneumonia. Most cases of bacterial pneumonia start with a sudden attack of chills, high fever, and chest pain. The patient also may develop a painful cough, which is dry at first but later produces rust-colored sputum. Most cases of viral pneumonia are mild.
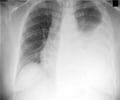
Using a stethoscope, the doctor can hear characteristic sounds from the lungs that indicate the presence of pneumonia. X rays and laboratory tests confirm the diagnosis. To determine the type of microbe involved, the doctor examines the patient's sputum.
The physician also looks for signs of confusion, which may indicate that there is inadequate oxygen flowing to the brain, or that pneumonia-causing germs have moved from the lung into the bloodstream. Confusion is more common in older patients with pneumonia than it is in younger patients. In addition to confusion, the doctor looks for other signs of low blood oxygen, such as a purplish hue to the lips, fingernails or hands.
Bacterial pneumonias may begin to respond to treatment within two to three days, and a hospitalized patient may be discharged within five to seven days if the pneumonia affected only a modest portion of the lung. Atypical pneumonias, which usually have less severe symptoms, are often treated successfully on an outpatient basis, while more extensive bacterial pneumonias, especially in debilitated persons, may result in prolonged hospitalization or respiratory failure.
A vaccine has been developed against some of the common forms of Streptococcus Pneumonia. Although this vaccine appears to be moderately effective when given to otherwise healthy persons, there is some question whether it works as well in patients who are suffering from debilitating diseases.
In addition to antibiotics, other treatments for pneumonia include: close observation, rest, adequate fluids, and use of supplemental oxygen to arise blood oxygen level. Cough should be only partially suppressed, because it is an important defense mechanism that aids in cleaning infected material from the lungs. In some cases, a progressive pneumonia may need to be treated with medicine that elevates the blood pressure, or with artificial ventilation using a mechanical ventilator.