- Postpartum Hemorrhage: Incidence, Risk Factors, and Outcomes in a Low-Resource Setting - (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5098756/)
- Global Causes of Maternal Death: A WHO Systematic Analysis. - (https://www.ncbi.nlm.nih.gov/pubmed/25103301)
- Postpartum Haemorrhage - (https://www.who.int/medicines/areas/priority_medicines/Ch6_16PPH.pdf)
- About Postpartum Hemorrhage - (https://www.chop.edu/conditions-diseases/postpartum-hemorrhage)
- More Information on Postpartum Hemorrhage - (https://www.urmc.rochester.edu/encyclopedia/content.aspx?ContentTypeID=90&ContentID=P02486)
- Prevention and Management of Postpartum Hemorrhage - (https://www.aafp.org/afp/2007/0315/p875.html)
- Post Partum Hemorrhage: Causes and Management - (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3688110/)
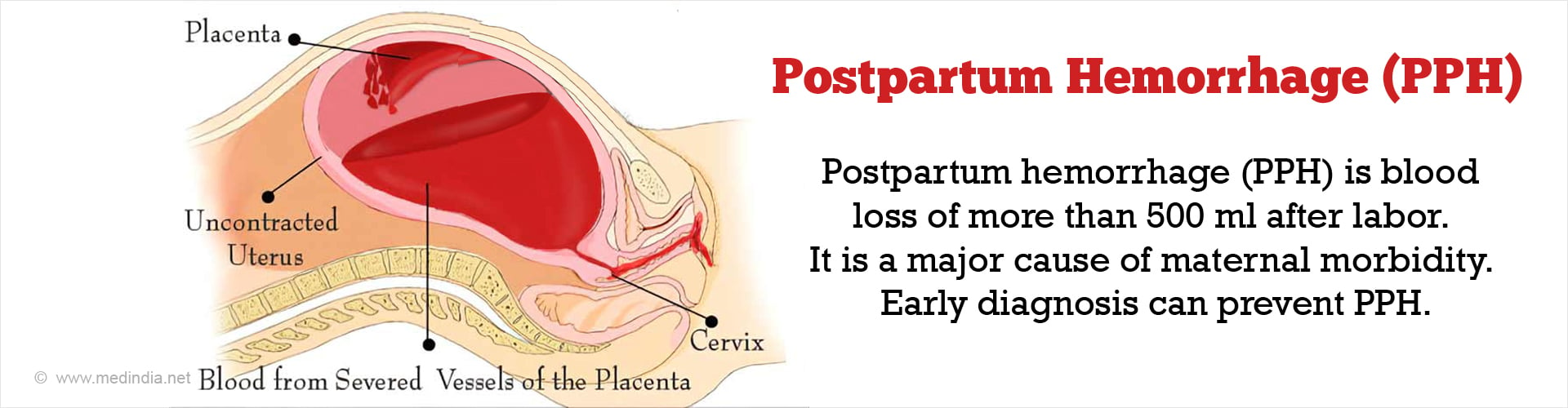
What is Postpartum Hemorrhage?
Postpartum hemorrhage (PPH) is generally considered as an obstetrical emergency and is a major cause of maternal morbidity and mortality in the world. The risk of death of these mothers is low in high-income group countries (1 in 100,000 deliveries) and high in low-income countries (1 in 1000 deliveries).(1✔ ✔Trusted Source
Postpartum Hemorrhage: Incidence, Risk Factors, and Outcomes in a Low-Resource Setting
Go to source) It is estimated that every year 3% to 5% of women who deliver babies will experience postpartum bleeding. Many of these events are preventable but are the cause of 25% of maternal deaths worldwide.(2✔ ✔Trusted Source
Global Causes of Maternal Death: A WHO Systematic Analysis.
Go to source)
If the diagnosis is done on time and corrective measures are taken, PPH can be prevented and maternal mortality avoided.
The WHO definition of postpartum hemorrhage (PPH) is blood loss greater than 500 ml after labor.
Based on the amount of blood loss, it can be -
Minor – or less than one - liter blood loss
Major – More than one - liter blood loss
Severe – Over two liters blood loss
PPH can be of two types:
- Primary: occurs within 24 hours of delivery
- Secondary: occurs beyond 24 hours (also called late postpartum hemorrhage)(3✔ ✔Trusted Source
Postpartum Haemorrhage
Go to source)
What are the Causes of Postpartum Hemorrhage?
The causes of Post-Partum Hemorrhage include:
- Uterus without muscle tone or Uterine atonia: This is the most common cause of a true postpartum hemorrhage.
- Post-delivery, the uterus contracts and retracts to normal size slowly, however, if there are imperfect contractions and retractions of uterine musculature, it will cause continuous bleeding. There are various reasons for this loss of tone and include:
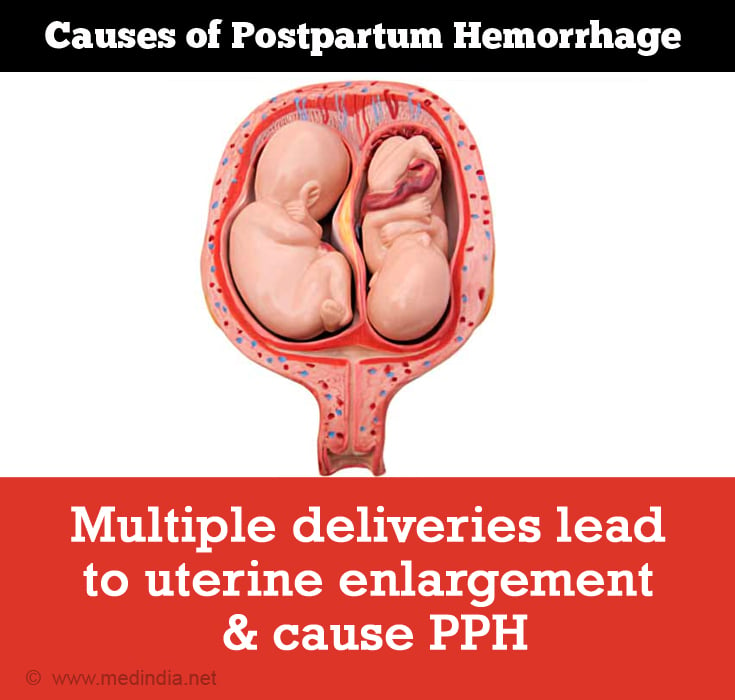
- Elderly age group mother who had multiple deliveries in the past (grand multipara)
- Over distended uterus due to twin or triplets or big baby
- Anemia and malnutrition
- Prolonged labor
- Trauma: Trauma to the genital tract such as the cervix, vagina, perineum and rarely uterine rupture causes bleeding.
- Retained tissues: Bits of placenta or blood clots
- Drugs: Drugs like Ritodrine, MgSO4, Nifedipine. induces Postpartum Hemorrhage. Individuals taking these drugs must use them with caution.
- Coagulation disorders: Conditions, where such disorders may occur are, a premature separation of the placenta from the uterus (Abruptio placentae ) or jaundice in pregnancy.(4✔ ✔Trusted Source
About Postpartum Hemorrhage
Go to source)
What are the Symptoms and Signs of Postpartum Hemorrhage?
The foremost sign of PPH postpartum hemorrhage is hemorrhage from vagina after delivery.
Usually, the bleeding is slow trickle from the vagina.
Rarely, it is concealed as vulvovaginal or broad ligament hematoma (i.e. collection of blood outside blood vessels).
There is associated anemia in severe cases along with symptoms of shock due to decreased blood volume called hypovolemic shock. Low blood pressure and high pulse rate are seen in severe cases.(5✔ ✔Trusted Source
More Information on Postpartum Hemorrhage
Go to source)
How to Diagnose Postpartum Hemorrhage?
History of bleeding along with physical examination where the uterus can be easily felt in the lower abdomen is enough to come to a diagnosis. If in shock, the blood pressure will be low and pulse rate would be high. A further blood test will reveal a low hemoglobin.
The uterus is well contracted in cases of trauma as the cause of bleeding whereas, the uterus is flabby and becomes hard on massaging in cases the cause is decreased uterine muscle tone.
How do you Treat Postpartum Hemorrhage?
There are various steps in the management of postpartum hemorrhage.
In case of placental site bleeding:
- Palpate the fundus of uterus and massage to make it hard
- Start a crystalloid solution (Normal Saline) with Oxytocin
- Catheterize the bladder
- Give antibiotics (Ampicillin and Metronidazole)
- Uterine massage and bimanual compression
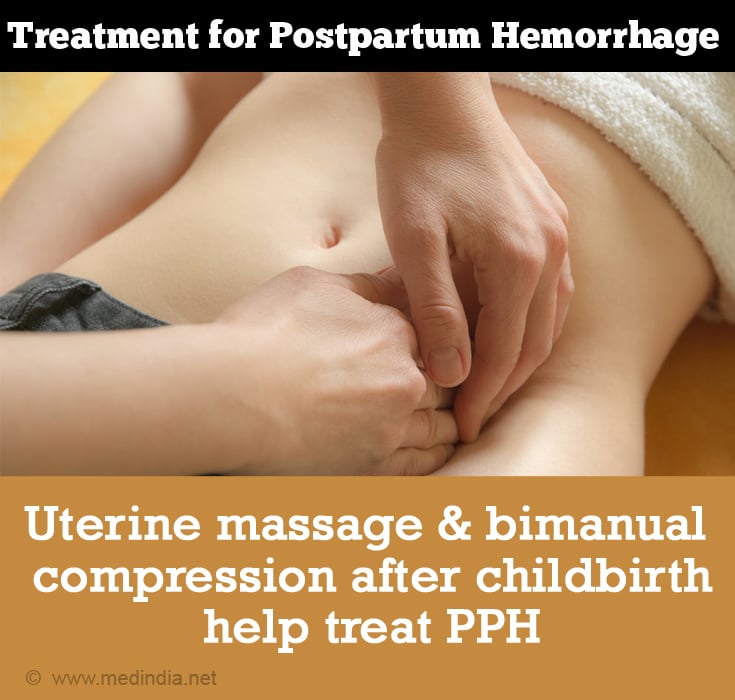
In the case of traumatic bleeding, the site of trauma is sutured under general anesthesia after the placenta has been expelled.
Blood transfusion may be necessary depending on the hemoglobin and the state of the patient.
Ensure that the cause of PPH is taken care and addressed.
In cases where the bleeding is persistent and refractory, the use of tranexamic acid is advised.(6✔ ✔Trusted Source
Prevention and Management of Postpartum Hemorrhage
Go to source)
Prevention of Postpartum Hemorrhage
Postpartum hemorrhage can be prevented by various methods: the first being reducing the risk factors for developing anemia, i.e., by ensuring that hemoglobin levels of the mother are greater than 10 g/dL so that she can withstand blood loss.
Blood grouping must be done before delivery to ensure swift transfusion if and when required.
Placental localization must be done using ultrasonography and in complicated cases using MRI scans.
High-risk cases must be delivered in a well-equipped hospital.
Postpartum hemorrhage is a major contributing factor to maternal mortality. It must be controlled by taking various precautionary measures during delivery.
- Active management of the third stage of labor must be a routine for all women.
- In the case of induced or augmented labor, oxytocin drip must be continued for an hour after delivery.
- For women delivered by C-section, oxytocin must be given to reduce loss of blood.
- After delivery, the doctors should not rush to deliver the placenta. If the placenta is separated early, the blood vessels (or the intervillous spaces) do not get enough time to contract and help control the flow of blood.
- Exploration of the uterovaginal canal for bits remaining.
- Observation for 2 hours after delivery.
- Examination of placenta to detect missing parts.(7✔ ✔Trusted Source
Post Partum Hemorrhage: Causes and Management
Go to source)