- Heart Inflammation - (https://www.nhlbi.nih.gov/health-topics/heart-inflammation)
- Pericarditis - Better Health Channel - (https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/pericarditis)
- Pericarditis - (https://www.ncbi.nlm.nih.gov/books/NBK431080/)
- Pericardial Disease: Diagnosis and Management - (https://www.ncbi.nlm.nih.gov/pmc/articles/pmc2878263/)
- About Pericarditis - (https://www.nhs.uk/conditions/pericarditis/)
- What is Pericarditis? - (https://www.heart.org/en/health-topics/pericarditis/what-is-pericarditis)
- Pericarditis - Department of Surgery - (https://surgery.ucsf.edu/conditions--procedures/pericarditis.aspx)
About
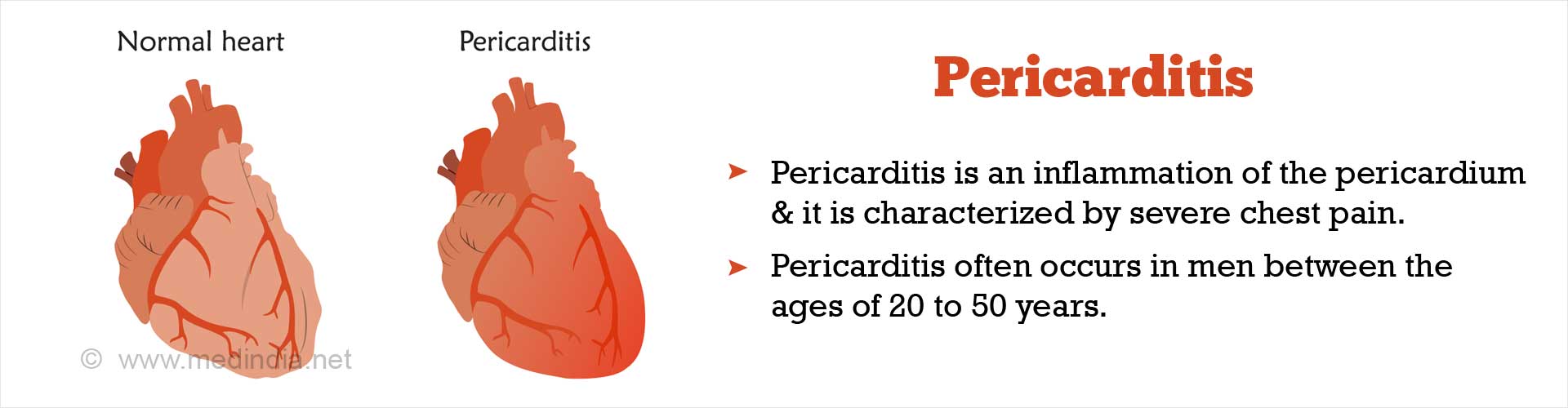
Pericarditis occurs when the pericardium gets inflamed. It is characterized by severe chest pain.
What is pericarditis?
Pericarditis, as the name suggests, is an inflammation of the pericardium, the protective sac around the heart. The pericardium consists of 2 layers separated by a thin layer of fluid that prevents the layers from generating friction with each other. When there is inflammation in the pericardium, the 2 layers rub against each other and the heart, creating intense chest pain that resembles a heart attack. The pain is aggravated when the individual inhales.(1✔ ✔Trusted Source
Heart Inflammation
Go to source)
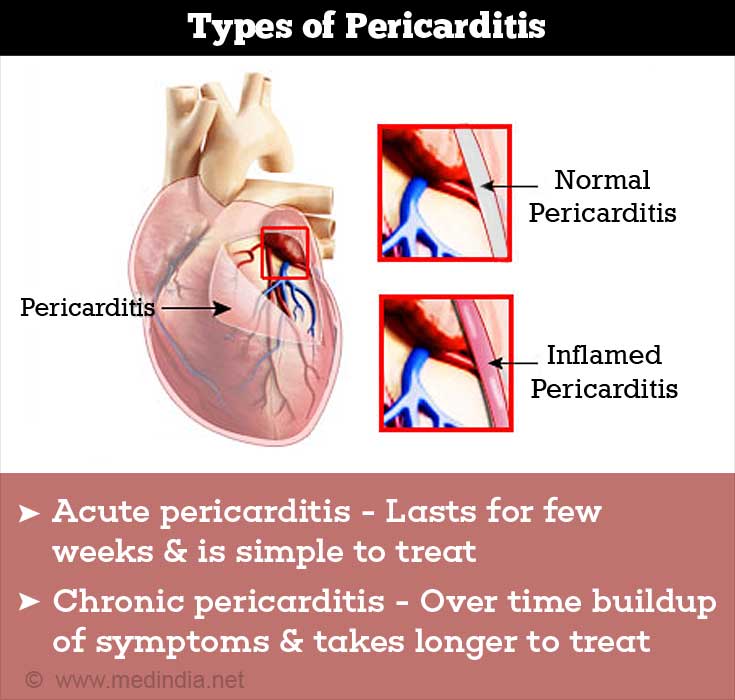
There are 2 main forms of pericarditis:
- Acute pericarditis occurs for a short while (lasting for a few weeks) and is simple to treat.
- Chronic pericarditis results from a buildup (over time) of the symptoms of pericarditis and takes longer to treat. There are 2 forms of chronic pericarditis.(2✔ ✔Trusted Source
Pericarditis
Go to source)
- The first is incessant pericarditis, where the condition recurs within 6 weeks, when the treatment is progressively stopped.
- The second is intermittent pericarditis, where the condition recurs after 6 weeks of treatment.
In addition, pericarditis can also be classified as autoimmune pericarditis, post-myocardial infarction syndrome, and infectious pericarditis. Pericarditis often occurs in men between the ages of 20 and 50 years.
Causes of pericarditis
There is no clearly defined cause of pericarditis. In general, pericarditis tends to occur following a heart attack. The heart muscles that are damaged cause the 2 layers of the pericardium to get affected leading to pericarditis. Dressler’s syndrome is a similar situation that occurs after a prolonged gap following a heart attack. This is considered a case of an autoimmune response where the pericardium becomes a target of inflammation due to the damage to the heart muscles. In addition, health conditions such as AIDS, cancer, kidney damage, and tuberculosis may lead to pericarditis. Inflammatory conditions, eg, rheumatoid arthritis or lupus erythematosus may also cause pericarditis.

Other causes of pericarditis include any injury to the chest or the heart (as a result of an accident), certain medications such as chemotherapy drugs or penicillin, and infection with viruses, fungi, and bacteria. Some viruses that cause pericarditis are adenoviruses, the cytomegalovirus, HIV, the influenza virus, the herpes simplex virus, the hepatitis C virus, and the common cold virus. Fungi such as Actinomyces, Candida, Histoplasma and Aspergillus, can also cause pericarditis.(3✔ ✔Trusted Source
Pericarditis - Better Health Channel
Go to source)
Recurring pericarditis is observed, in general, after a case of acute pericarditis. The exact cause of the condition is unknown. It has been observed that patients who are treated with corticosteroids for acute pericarditis are most likely to develop recurring pericarditis. There are 2 potential explanations for recurring pericarditis. In the first case, the virus that causes acute pericarditis is not completely removed from the body and lies dormant in the pericardium. When the virus is reactivated, it triggers an episode of recurring pericarditis. In the second case, autoimmune antibodies are generated during acute pericarditis. Following a few months or years, these antibodies sometimes attack the pericardium, resulting in inflammation. This results in a recurring episode of pericarditis.
Symptoms of Pericarditis
Acute pericarditis can usually cause intense chest pain. The middle, or left side of the chest is normally affected by pain. The pain may also be in the back, the abdomen, the neck, or the shoulders. Other symptoms include palpitations, difficulty in breathing, fever, cough, muscle pain, and lack of strength.

Symptoms vary based on the type of pericarditis. In acute pericarditis, the individual experiences intense spasms of pain in the chest on the left side or behind the breastbone. The pain may then spread to the neck and the shoulder on the left side. The individual suffers from chest pain while lying down, breathing deeply or coughing. When the individual sits up, there is a reduction in pain.
Individuals with chronic pericarditis exhibit similar symptoms. Chest pain is the major symptom. They may also suffer from cough, shortness of breath, and exhaustion. Individuals who suffer from a severe case of chronic pericarditis also show hypotension or low blood pressure as well as swelling in the legs and the abdomen.(4✔ ✔Trusted Source
What is Pericarditis?
Go to source)
Diagnosis of Pericarditis
Pericarditis can be diagnosed in an individual through a physical examination. The medical history of the patient provides information on the symptoms related to the condition. The doctor may verify if the patient has had a heart attack, flu, or suffered any injury to the chest, or if the patient has been afflicted with any other medical condition that gives rise to pericarditis. Since the main symptom for pericarditis is chest pain, the doctor will verify the location of the pain in order to confirm the diagnosis of pericarditis.
1. Physical examination: The doctor checks for the presence of fluid in the chest region, either in the pericardial sac or lungs, using a stethoscope. Pericardial rub is the sound of the pericardium rubbing against the heart, when it is inflamed. The sound that is produced is a grating sound.
2. The jugular venous pressure or JVP is raised on examinationHow to examine jugular venous pressure or JVP in a patient -
- JVP is indicative of the central venous pressure of the heart
- The neck vein on right side is examined (right internal jugular vein)
- The neck is turned slightly to the left with patient in semi-reclined position at a 45° angle on the bed
- The vein travels from the inner side of the collar bone or clavicle towards the right ear lobe
- Once located look for two waves or double waveform pulsation
- Measure the height of the prominent vein appearance from the clavicle. It should normally be less than 3 cms
3. Other tests for diagnosis:
Some of the tests for diagnosing pericarditis include chest X-ray, ECG (electrocardiogram), echocardiography, cardiac CT, cardiac MRI and blood tests.
The first few diagnostic tests that are conducted are blood tests, draining and analyzing the fluid from the inflamed pericardial sac as well as performing an electrocardiogram. If the results from these tests are negative, and other symptoms persist that resemble pericarditis, the remaining diagnostic tests are recommended to confirm the condition.
Blood tests: Infections or the presence of a heart attack can be detected with blood tests.
Electrocardiogram (ECG): The electrical activity of the heart can be monitored with an ECG. Pericarditis causes a change in the electrical activity of the heart.
Cardiac Magnetic Resonance Imaging (MRI): Radio waves and magnets are used to provide a detailed image of the heart and the pericardium. Changes to the pericardium can be visualized through this technique.
Echocardiogram: Sound waves are used to create an image of the heart and the pericardium. Inflammation of the pericardium can be detected with an echocardiogram. The functioning of the heart can also be detected with an echocardiogram.
Cardiac Computed Tomography (CT): A detailed X-ray picture gives an indication of the source of chest pain and confirms the diagnosis of pericarditis.
Chest X-ray: A chest x-ray aids in visualizing the heart and to observe if it is swollen due to an inflammation in the pericardium.(5✔ ✔Trusted Source
Pericardial Disease: Diagnosis and Management
Go to source)
Treatment of Pericarditis
Rest is the primary recommendation for pericarditis in order to reduce the fever. Medications are generally used to treat pericarditis. Surgery is rarely used as a treatment option.
Pain-relief medications such as ibuprofen and aspirin are used to counter the inflammation in the pericardium. Pericarditis caused by infections can be treated with antibiotics. Medications such as prednisone or colchicine are recommended for persistent pain.(6✔ ✔Trusted Source
About Pericarditis
Go to source)

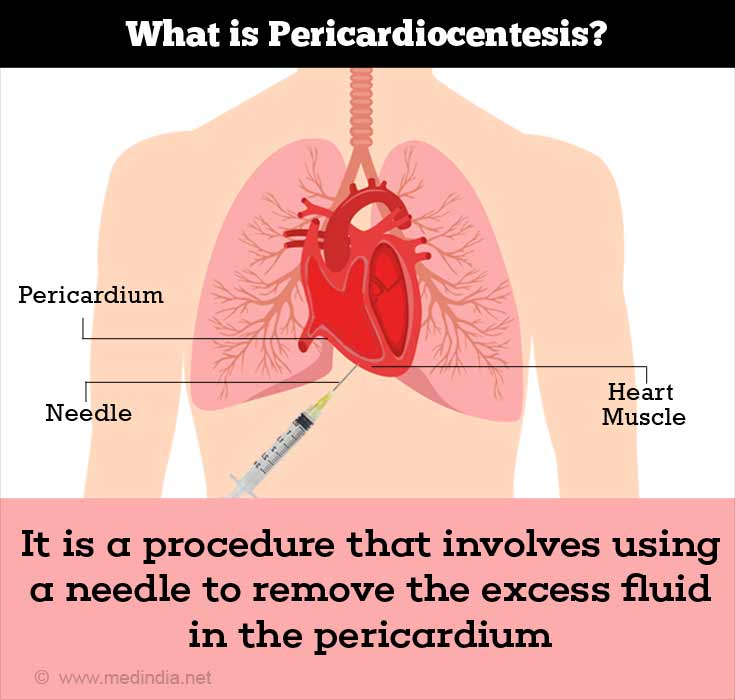
Pericardiectomy:This is a surgical procedure to treat a severe condition known as chronic constrictive pericarditis. The pericardium is removed in this procedure.
Pericardiocentesis: This procedure involves using a needle to remove the excess fluid in the pericardium. The removal of the fluid reduces the pressure of the pericardial sac on the heart.(7✔ ✔Trusted Source
Pericarditis - Department of Surgery
Go to source)