- Pelvic Inflammatory Disease (PID) - CDC Fact Sheet - (http://www.cdc.gov/std/pid/stdfact-pid.htm)
- Pelvic Inflammatory Disease: Guidelines for Prevention and Management - (http://www.cdc.gov/mmwr/preview/mmwrhtml/00031002.htm)
- Pelvic inflammatory disease - (http://www.nhs.uk/conditions/pelvic-inflammatory-disease/pages/treatment.aspx)
- Pelvic inflammatory disease (PID) - (http://www.mayoclinic.org/diseases-conditions/pelvic-inflammatory-disease/basics/prevention/con-20022341)
What is Pelvic Inflammatory Disorder?
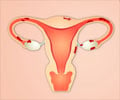
Pelvic inflammatory disease or disorder (PID) is a reproductive disorder that affects women. It is a complication that often develops because of sexually transmitted diseases, but can also be caused by other circumstances. The condition can cause damage to the uterus, ovaries, fallopian tubes and the rest of the reproductive system as infection spreads. The damage is unfortunately irreversible and this is a major cause for infertility in women. Incidentally, PID is also preventable and if treated appropriately and early enough, damage can be minimized and the condition may not affect reproductive function.
The main reason why the condition is so problematic is because it often does not cause any visible symptoms and goes undiagnosed until it is too late. Therefore quite often, the condition only gets picked up when a woman has trouble conceiving or when chronic pelvic pain sets in.
What are the Causes of Pelvic Inflammatory Disorder?
Pelvic inflammatory disorder is almost always caused by bacterial infection. Bacteria that are present in the vagina or cervix sometimes travel up the reproductive tract and cause PID. The most common types of bacteria that are responsible are those that cause sexually transmitted infections like chlamydia or gonorrhea. PID could at times, be caused by other bacteria as well that are not responsible for sexually transmitted infections.
Certain conditions or circumstances can increase your risk of developing pelvic inflammatory disorder. These include:
- If you have neglected a sexually transmitted disease and failed to treat it
- If you have a promiscuous lifestyle with multiple sex partners
- If your sexual partner is promiscuous and has multiple sex partners
- If you are under the age of 25 and are sexually active
- If you douche regularly. Douching removes the protective organisms in the vagina and changes the pH, thus favoring the growth of disease-causing bacteria.
- If you have suffered from PID before
- If you use an intrauterine device (IUD). The risk is higher towards the first few months after beginning usage, but this risk is reduced with the new generation of IUDs
What are the Symptoms and Signs of Pelvic Inflammatory Disorder?
Pelvic inflammatory disorder doesn’t always produce symptoms and very often the symptoms only appear as the condition progresses. Symptoms of PID can include:
- Nausea, fever, chills and vomiting
- Abnormally lengthy duration of periods
- Increased pain during menstruation and unusual discharge
- Spotting that may be noticed between periods and may be accompanied by pain
- Pain that radiates to the lower abdomen and back
- Painful vaginal intercourse
If you notice any of these symptoms, make it a point to consult your health care provider immediately. PID is not easy to diagnose because the symptoms overlap with many less threatening conditions like urinary tract infections and ovarian cysts. If PID is not diagnosed or treated promptly, it can result in serious complications such as an ectopic pregnancy, infertility and chronic pain. The risk of such complications increases with any recurrence of PID. This is why regular checkups are so important, especially if you are sexually active.
How to Diagnose Pelvic Inflammatory Disorder?
Pelvic inflammatory disease is hard to diagnose on the basis of symptoms alone and you will probably need to undergo a pelvic exam. Samples of vaginal discharge and cervical cultures will be taken during the pelvic exam and analyzed to identify the bacteria responsible for the infection. Tests that are commonly used to confirm the diagnosis and to establish the effects of the infection include:
- Blood tests to check for any signs of infection.
- An ultrasound to check for any damage or abnormalities in the reproductive organs.
- An endometrial biopsy (procedure to obtain tissue sample from the inner lining of the uterus) is not usually necessary but may be performed if required.
- Laparoscopy, which is another diagnostic tool that is rarely used for PID, but may be necessary in some situations to enable direct examination of the reproductive organs.
How do you Treat Pelvic Inflammatory Disorder?
When dealing with pelvic inflammatory disorder, the key to successful treatment is early diagnosis. This is extremely important because it is difficult to repair damage to the reproductive organs, once it is done. Avoid delaying treatment as this greatly increases the risk of complications.
Treatment for pelvic inflammatory disease includes:
- Antibiotics: Treatment with oral antibiotics usually begins before all the test results are even in. Treatment is fairly standard because the infection is generally caused by a combination of bacteria and the antibiotics are accordingly administered. In more advanced cases of infection, treatment is administered both orally and intravenously. In very serious cases, the patient may even need to be hospitalized and treatment has to be provided intravenously. You may also be given painkillers along with antibiotics if the pain is severe. Make sure to keep all your appointments as the follow-ups are extremely important. Tests are conducted to monitor progress and responsiveness to treatment. The treatment plan will then be continued or modified as necessary.
- Surgery: Surgical treatment is not the standard approach to pelvic inflammatory disease treatment but it may be necessary under certain circumstances, such as when the infection causes the formation of an abscess and antibiotics are ineffective. In these cases surgery may be the safest option as it becomes necessary to remove the abscess and at times possibly the affected organ itself, so as to contain the risk of infection to the entire pelvis and abdomen if the abscess were to rupture.
Prevention of Pelvic Inflammatory Disorder
The only foolproof way to prevent pelvic inflammatory disorders would be avoid picking up an STD, by avoiding all kinds of sexual activity. This off course, is contrary to human behavior or the behavior of any species that must reproduce to survive, so instead it would be prudent to take certain precautions. If you are sexually active, you can lower your risk of infection by:
- Maintaining a monogamous relationship with a partner who is free of STDs
- By using barrier contraceptives. When used as per the directions, both mechanical and chemical barriers can be extremely effective in lowering the risk of STDs, PID and tubal infertility.
It should be pointed out that barrier methods include mechanical barriers like condoms and diaphragms, and chemical barriers like vaginal spermicides. It is also notable that latex condoms when used correctly are extremely effective at preventing various infections and they provide greater protection as compared to natural membrane condoms. The use of vaginal spermicides can also help to lower your risk of infection as studies have shown that this reduces the risk of cervical infection with bacteria like C. trachomatis and gonorrhoeae. The best strategy would be to use a combination of barrier methods like a condom with spermicide or a diaphragm with spermicide.