- Tice A D. Osteomyelitis.In Longo DL,Fauci AS, Kasper DL, Hauser SL, Jameson JL, Loscalzo J editors. Harrison s Principles of Inernal Medicine Volume 1, 18thedition The Mc Graw Hill Company 2011:1071
- Berendt A,McNally M A.Diseases of Bones and Joints. In Russell R.C.G, Williams N S, BulstrodeC.J.K editors.Bailey and Love s Short Practice of Surgery 24th edition Arnold 2004:419
- Rosenberg A E. Bones, Joints and Soft Tissue Tumors.In Kumar V, Abbas A K, Fausto N, Aster JC editors.Robbins and Cotran Pathologic Basis of Disease 8th edition Elsevier 2011: 1221.
About
What is Osteomyelitis?
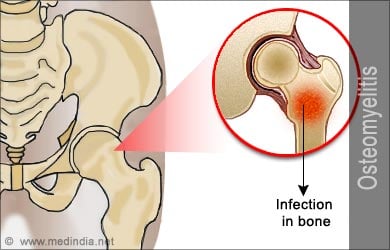
Osteomyelitis results from inflammation of the bone and marrow cavity which almost always means infection. Osteomyelitis may arise as a complication of systemic infection or as a solitary focus of disease.
Penetrating wounds, surgical procedures, dental extractions can all be precipitating factors for osteomyelitis. Diabetes in the host predisposes to osteomyelitis due to loss of sensation and impaired immunity in the host.
History tells us that osteomyelitis has been part of vertebrate biology since the time of the dinosaurs with fossil evidence of healed bone infection from the Pleistocene era to early humans. Thus the relationship between pathogenic bacteria and vertebrates is really long standing.
A wide variety of bacteria, fungi, viruses and parasites can cause osteomyelitis. Bacteria cause pyogenic osteomyelitis and mycobacteria cause tuberculous osteomyelitis. The disease can be extensive or localised to a single bone. The patient presents with fever, swelling, pain and this can be accompanied by a discharge at the site. Even in innocuous looking painless ulcers, especially in diabetics, the index of suspicion should be high and treatment should be started early after the necessary investigations to prevent the infection from becoming chronic.
The outcomes vary depending on the treatment provided, the follow up by the patient, the site of involvement and the presence of underlying disease.
Complications of osteomyelitis can be many and may even lead to loss of function of the bone and surrounding tissue. Awareness about the sites of infection and maintaining strict infection control practices especially prior to surgery can go a long way in prevention of osteomyelitis.







