- American Academy of Pediatrics. (2009) Prevention of Neonatal Ophthalmia. In: Pickering LK, Baker CJ, Kimberlin DW, Long SS eds. Red Book 2009 Report of the Committee on Infectious Diseases. 28th ed. Elk Grove Village, Ill: American Academy of Pediatrics; 827-9.
- Margaret R. (2011) Chlamydial and Gonococcal Infections in Infants and Children. Clin Infect Dis.; 53(3):S99-S102.
- Olitsky SE, Hug D, Plummer LS, Stass-Isern M. Disorders of the conjunctiva. In: Kliegman RM, Behrman RE, Jenson HB, Stanton BF, eds. Nelson Textbook of Pediatrics.
- Rubenstein JB, Tannan A. Conjunctivitis: infectious and noninfectious. In: Yanoff M, Duker JS, eds. Ophthalmology.
What is Neonatal Conjunctivitis?
Conjunctivitis in infants within first 28 days of life is referred as Neonatal Conjunctivitis or Ophthalmia Neonatorum. Conjunctivitis is defined as inflammation of conjunctiva, which is the thin tissue that covers the white part of the eye and inside portion of eyelids.
Neonatal conjunctivitis affects around 1-12% of newly born in the western world. The rates are higher in developing countries, where it affects almost 23% of infants.

What Causes Neonatal Conjunctivitis?
Neonatal conjunctivitis is usually caused by bacteria like Chlamydia trachomatis, Neisseria gonorrhoeae, Staphylococcus aureus, and Streptococcus pneumoniae. Gonococcal or chlamydial infections present in the genital tract of the mother are transmitted to the child during vaginal delivery and infects the eyes. The incidence of gonococcal bacteria as a cause of ophthalmia neonatorum has decreased, and other bacteria like Staphylococcus, Streptococcus and Haemophilus species have emerged as common causes of bacterial neonatal conjunctivitis. Lack of hygiene in hospital, lack of awareness among mothers and guardians, and childbirth in household settings under non-aseptic conditions are some of the reasons for such infections.
In rare cases, neonatal conjunctivitis can be caused due to viral infection by herpes simplex virus. Chemical irritants can also cause conjunctivitis. Chemical conjunctivitis is usually caused by silver nitrate drops instilled in the newborn to prevent neonatal conjunctivitis. These are not used nowadays.
What are the Symptoms of Neonatal Conjunctivitis?
Infants affected with neonatal conjunctivitis present with discharge from the eye, redness of the eye and swelling of the eyelid. Fever may also be present in some babies.
Chemical conjunctivitis develops a day or two after silver nitrate drop instillation. The baby has red eyes with watery discharge.
Bacterial conjunctivitis in a child usually appears as redness of eye, swelling of the eyelid and pus discharge. Redness and discharge are more severe in cases of gonococcal infection. The cornea may also be damaged. Chlamydial eye infection causes an initial watery discharge, which changes into pus-containing discharge. The skin of the eyelids and around the eyes may also be inflamed.
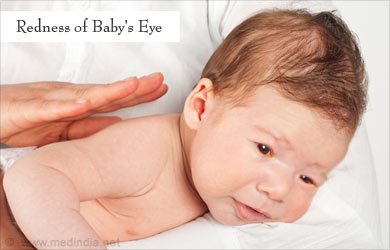
Viral conjunctivitis usually presents as watery discharge along with traces of blood. Along with conjunctivitis, inflammation of various parts of the eyes like cornea, iris, retina and optic nerve may be present. Viral conjunctivitis may also cause cataract or small eruptions on the skin.
How is Neonatal Conjunctivitis Diagnosed?
Investigations for neonatal conjunctivitis are performed in a step-wise manner. History taking is usually the first step where mothers are asked about previous or present sexually transmitted disease like gonorrhea or chlamydia infection. If medical reports of the mother are readily available, they can be gone through to identify any sexually transmitted disease or viral infection. A cervical swab can also be cultured to identify any infection in the mother, which may have been transferred to the child.
Physical examination of eyes for symptoms also allows the physicians to identify a particular type of infection. Examination of culture obtained from the conjunctiva provides confirmed diagnosis for infection type. If the doctor suspects gonococcal infection, urgent testing is requested by Gram staining method.

Blocked nasolacrimal duct, a small duct that connects the inner angle of the eye and the nose, is a common condition, which produces similar symptoms as ophthalmia neonatorum and therefore often interferes with appropriate diagnosis. While this condition also causes moderate-to-severe sticky and crusty discharge from the eye in newborn babies, it does not cause redness and swelling of eyes. Furthermore, the discharge usually stops after simple cleaning of the eye, specifically the duct.
How is Neonatal Conjunctivitis Treated?
Chemical conjunctivitis usually subsides on its own without specific treatment.
Treatment for bacterial neonatal conjunctivitis should be started before waiting for the culture results since the results can take a few days. Also in many cases, the results are inconclusive. Therefore, standard guidelines suggest that as soon as infective conjunctivitis is suspected in neonates, a broad-spectrum antibiotic like ofloxacin 0.3% (4 times a day) must be initiated for a week or until conclusive culture reports are obtained. Drugs like ofloxacin or norfloxacin eye drops can handle infections due to non-sexually transmitted diseases.
If recurrence of the infection is observed after antibiotic therapy, infection with chlamydia should be suspected. Chlamydial infection usually responds to oral erythromycin syrup.
Gonococcal ophthalmia neonatorum should be treated more urgently because of the associated complications. Local medications like bacitracin ointment and injections of ceftriaxone or cefotaxime may be administered. Atropine eye drops are administered if corneal injury is observed.
Viral infection is treated with local and injectable forms of the antiviral drug, acyclovir.
What is the Prognosis or Outcome of Neonatal Conjunctivitis?
Most cases of neonatal conjunctivitis respond to broad spectrum antibiotic eye drops. Full recovery occurs for chemical conjunctivitis even without treatment. Gonococcal conjunctivitis can be associated with severe complications if not treated early. Similarly, viral conjunctivitis can result in permanent vision loss. The viral infection can be fatal to the baby if it spreads to other parts of the body.
How can Neonatal Conjunctivitis be Prevented?
Preventive measures for neonatal conjunctivitis must be taken at three stages viz. prenatal, natal and post-natal. Pregnant mothers with chlamydial or gonococcal infections must be treated to reduce the chances of disease transmission during vaginal delivery. Considering natal care, it is vital to perform vaginal delivery in a highly aseptic environment to prevent infections during childbirth. If vaginal infections are present in the mother, closed eyelids of the newborn must be cleaned properly and then dried.
Since the silver nitrate (1% solution) administration has been found to cause chemical conjunctivitis, other preventive drugs are preferred now. In case of suspected neonatal conjunctivitis, following preventive treatments are used:
- 1% tetracycline ointment or 0.5% erythromycin ointment
- One time administration of ceftriaxone in dosage 50mg/kg given via IV or IM route
Health tips
- Get yourself treated before or during pregnancy if you are suffering from an infection of the genital tract. If possible, avoid pregnancy, if you or your partner has an uncured sexually transmitted disease.
- Maintain a hygienic environment around the baby to prevent bacterial conjunctivitis.
- Never forget to administer eye drops or medications to the child as prescribed by the doctor.






