- Defibrillators - (https://www.nhlbi.nih.gov/health/health-topics/topics/icd)
- Implantable Cardioverter Defibrillator (ICD) - - (http://www.heart.org/HEARTORG/Conditions/Arrhythmia/PreventionTreatmentofArrhythmia/Implantable-Cardioverter-Defibrillator-ICD_UCM_448478_Article.jsp)
- Recent advances in the entirely subcutaneous ICD System - (http://doi.org/10.12703/P7-46)
- Implantable Cardioverter Defibrillator (ICD) Insertion - (http://www.hopkinsmedicine.org/healthlibrary/test_procedures/cardiovascular/implantable_cardioverter_defibrillator_icd_insertion_92,p08774/)
- Tracy, Cynthia M.; Epstein, Andrew E.; Darbar, Dawood; DiMarco, John P.; Dunbar, Sandra B.; Estes, N.A. Mark; Ferguson, T. Bruce; Hammill, Stephen C.; Karasik, Pamela E.; Link, Mark S.; Marine, Joseph E.; Schoenfeld, Mark H.; Shanker, Amit J.; Silka, Michael J.; Stevenson, Lynne Warner; Stevenson, William G.; Varosy, Paul D. (January 2013). "2012 ACCF/AHA/HRS Focused Update Incorporated Into the ACCF/AHA/HRS 2008 Guidelines for Device-Based Therapy of Cardiac Rhythm Abnormalities". Journal of the American College of Cardiology 61 (3): e6–e75. doi:10.1016/j.jacc.2012.11.007.
- Reiffel, J.A. and J. Dizon, Cardiology patient page. The implantable cardioverter-defibrillator: patient perspective. Circulation, 2002. 105(9): p. 1022-4.
- ICD for Primary Prophylaxis of Sudden Cardiac Death: An Indian Perspective - (http://www.japi.org/april2007/suppliment/Suppliment_47-53.pdf)
What is Implantable Cardioverter Defibrillator (ICD)?
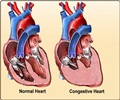
The electrical activity of the heart keeps the heart beating constantly at a regular rhythm. A disturbance in this rhythm is called an arrhythmia.
In patients with arrhythmias arising from the lower heart chambers, the heart cannot pump the blood adequately, which makes the patient pass out or even die if not intervened immediately. In such patients, the procedure used to stun the heart to get it back to a normal rhythm is called defibrillation.
An implantable device which tracks the heart rhythm delivers electrical impulses and shocks the heart when it skips out of the rhythm is called an Implantable Cardioverter Defibrillator.
Defibrillation can also be carried out with an external device, an Automatic External Defibrillator (AED), which helps to deliver the shock in case of Sudden Cardiac Arrest. But in patients with risk of the sudden cardiac death, the implantable defibrillators are required.
The ICD has a pulse generator and wires/leads. The pulse generator which has a battery and a small computer is placed in a small box underneath the skin in the chest. It also has wires called leads that have electrodes at the tips and are passed to the heart through a vein.
What are the Indications of Implantable Cardioverter Defibrillator (ICD)?
Sudden Cardiac Arrest (SCA): The implantation of an ICD is essential in patients with the history or the risk of the Sudden Cardiac Arrest. But in patients with SCA with reversible causes of arrest like electrolyte disturbance or myocardial ischemia (decreased blood to the heart muscle), ICD is not essential if the associated rhythm disturbances are corrected with the treatment for the particular condition.
ICD is also essential in the life-threatening arrhythmias like ventricular tachycardia (the ventricles beat fast) and ventricular fibrillation (the ventricles quiver) associated with the conditions like:
- Coronary Artery Disease (Disease with block in the blood vessels that provide blood to the heart)
- Non-ischemic Dilated Cardiomyopathy (Condition where the muscle layer of the heart is dilated)
- Arrhythmogenic Right Ventricular Cardiomyopathy (A genetic heart disease involving the right ventricle)
- Genetic heart diseases due to ion channel disorders like long QT syndrome, short QT syndrome, Brugada syndrome, and catecholaminergic polymorphic ventricular tachycardia
- Idiopathic Ventricular Fibrillation. (Heart rhythm disorder with quivering of the ventricles due to unknown cause)
- Hypertrophic Cardiomyopathy (Condition where the heart muscle layer is thickened)
Severe Heart Failure: In patients with severe heart failure, Cardiac Resynchronization Therapy (CRT) is essential. CRT involves implanting a biventricular pacemaker which helps to synchronize the function of the two ventricles in these patients. CRT used along with a defibrillator is referred to as CRT-D.
How is Implantable Cardioverter Defibrillator (ICD) Implanted?
Before the Procedure:
- The diagnostic tests which are required to diagnose the arrhythmias and to confirm the need for the implantation are:
- Electrocardiogram: Electrocardiogram is an investigation by which the electrical heart rate and rhythm of the heart are recorded.. It records only for a short duration, which is sometimes not sufficient to detect the life-threatening arrhythmias which are intermittent, and appear only sometimes during the day.
- Event Monitor: An event monitor is used to record the abnormal events in the heart’s electrical activity. It is used for months or until the problem is identified.
- Echocardiogram: An echocardiogram is used to view the structure and function of the heart on a screen. It helps to see the chambers of the heart, valves and the movement of the heart.
- Electrophysiology Study: An electrophysiological study done in an Electrophysiology lab, helps to find the origin of the abnormal electrical impulses.
- Holter Monitor: Holter monitor is used to record the heart electrical activity continuously. The patient has to wear the recording device for a day or two.
- Inform your doctor regarding the health ailments like diabetes, bleeding disorders, kidney problems and the medications that you take before you undergo the procedure.
- It is required to fast before the procedure; you will be notified about it.
- Some investigations like blood work will be ordered by your doctor. You will be informed regarding the medications to be taken on the day of the procedure.
During the Procedure:
The procedure is usually performed under sedation and aseptic precautions. The nurse puts the intravenous line prior to the procedure. An electrocardiogram is connected and also the large electrode pads are placed on the chest and the upper back. The area on the chest below the collar bone is cleaned and draped. Local anesthesia is given in this area and then an incision is made. A tube called the sheath is inserted into a blood vessel. One or more leads are inserted through the sheath into the blood vessel and advanced till the heart. The leads are checked to make sure they are properly inserted. The sheath is then removed. Then ICD generator is placed in a pocket under the skin and attached to the leads. Your doctor will run few tests to ensure that the ICD is functioning properly. Then the skin is sutured and dressed.
After the Procedure:
- The nurse monitors parameters like the heart rate and blood pressure. After a few hours, you will be allowed out of the bed. Discharge can be on the same day or the next day. You will be prescribed the necessary medications before the discharge.
- Once you are at home you can get back to routine activity in a few days. It is suggested not to lift the heavy weights for a few weeks.
- If you receive a shock through the ICD, approach your doctor. Inform your doctor if you have chest pain, swelling in the chest, dizziness, breathlessness or palpitations.
Precautions:
Certain devices interfere with the ICD and can impair its function. Microwaves at home, electric generators, welding machines, metal detector in airports, electrocautery (used to stop bleeding during surgery), shock wave lithotripsy (used for crushing kidney stones) and Magnetic Resonance Imaging test may interfere with the ICD function. So you may have to avoid them or maintain a particular disturbance. Inform the concerned people about the ICD and show them a Medical ID card which states about your ICD to prevent exposure. Cell phones are safe but avoid carrying them in the shirt pocket. Tell your doctor about the ICD before any test, procedure or when you are in doubt.
How Does Implantable Cardioverter Defibrillator (ICD) Work?
ICD has four main functions:
- Anti-tachycardia pacing (ATP): The device delivers the rapid and regular impulses to maintain the normal heart rhythm by overtaking the irregular heart impulses.
- Cardioversion: It delivers the low energy shock to correct arrhythmias.
- Defibrillation: The high energy shock is delivered in the case of an episode of a life-threatening arrhythmias. The patient feels like a kick in the chest. This property is absent in a pacemaker, which only delivers low energy shock.
- Backup pacing: After the shock, the heart rate may drop to very low rate then the device stimulates heart until it reaches the normal rate.
Implantable Cardioverter Defibrillator Advantages
- It is a safe and an effective method to prevent sudden cardiac death in patients with life-threatening arrhythmias.
- It can be used for an indefinite period once in place unless there is any damage like a lead fracture or an infection.
- It just needs a small procedure for the generator change when the battery exhausts.
Implantable Cardioverter Defibrillator Risks
- Pocket Infection: Infection in the area below the skin where ICD generator is placed.
- Bleeding and infection of the incision site
- Injury to the blood vessel at the insertion site
- Lung Collapse: Injury to the lung during the surgery can cause the air entrapment between the lung and the chest wall and later can lead to lung collapse.
- Lead misplacement
- Inappropriate Shocks: Sometimes the shocks are delivered when not required.
- Injury to the heart
Conclusion
Implantable Cardioverter Defibrillator is the effective way to prevent sudden cardiac death in the risk group. It is the safe procedure with minimal complications. Patients with ICD should be conscious about electronic devices which interfere with the ICD function. The patients should notify their health care provider regarding the presence of an ICD before any procedure or test.