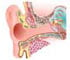
- Hearing loss - infants - (http://www.nlm.nih.gov/medlineplus/ency/article/007322.htm)
- High Risk Factors for Hearing Loss - (www.infanthearing.org/statematerials/description/vt_high%20risk%20factors%20for%20hearing%20loss.pdf)
- How Early Intervention Helps Your Child - (https://www.babyhearing.org/language-learning/how-early-intervention-helps)
About
Worldwide statistics estimate that one in every 1000 infants is born with severe to profound hearing impairment and 6 in every 1000 are born with some degree of hearing loss. Children may also acquire hearing loss in course of their growth due to illnesses like measles and mumps.
Causes of hearing loss in children that can be corrected include build up of ear wax in the ear canal, build up of fluid behind the eardrum and injury or rupture to the eardrum. Certain conditions like ototoxicity (damage to receptor cells of hearing due to drugs), infections that can damage brain after birth, problems with the development in the structure of ear and tumors can result in permanent damage to hearing.
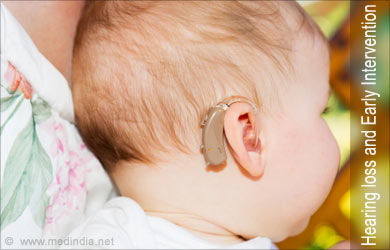
Early Intervention for Hearing Impairment
Early intervention is a term used for the process of identifying conditions in children that may cause delays in development of physical skills, cognitive skills, communication, adaptive skills and social and emotional development. The main focus of early identification and early intervention for a child with hearing loss is on developing communication skills, both verbal and sign language, to the maximum possible extent. Further, if hearing impairment is associated with other disorders like mental retardation, blindness, cerebral palsy, etc., the intervention program addresses those needs also.
Hearing impairment is detrimental to the normal speech and language development in such children. While speech and language are innate skills of human beings, these skills develop only by hearing, listening and incorporating the use of words, intonations, voice variations, and the patterns in which words are strung together to form expressions.

Why Early Intervention?
The American Academy of Pediatrics recommends a hearing screening to be done for every baby a few weeks after birth, and also follow-up visits up to two years of age. With modern technology of manual and automatic hearing testing routines, congenital hearing loss is being identified in children before they are 3 months of age. Identification of hearing impairment is possible by looking into the risk factors, responses of the baby to sounds around and seeking professional help when the risks and signs indicate a hearing problem.
Risk Factors for Hearing Loss
Some of the important risk factors associated with hearing loss can be listed and an informal screening can help in determining whether to look out for signs of hearing impairment. The risk factors include:
- Family history of hearing impairment
- Prenatal infections in the mother like rubella, herpes simplex and toxoplasmosis
- Abnormal development of the structures in head and neck region like cleft palate, atresia (absence of pinna), etc
- Premature birth
- Hyperbilirubinemia
- Medications given in neonatal period
- Syndrome associated with hearing loss like Waardenburg, neurofibromatosis, etc
- Recurrent infections in the ear, nose and throat
- Infections like meningitis, measles, mumps, etc
- Head trauma

Certain symptoms may be noticed by the mother or primary caregiver of the baby that can call for a detailed hearing assessment to be done.
- Absence of startling response to a sudden loud noise
- Absence of response to familiar voices in older infants, when spoken out of the infant’s view
- If a child is not using voice or speech to ask, seek attention or call out
Assessment Techniques for Hearing Loss
Hearing tests for infants are carried out objectively. Auditory Brain Stem response test uses electrodes placed on the infant’s head with a sound-generator inserted into the external ear, to record the responses of the auditory nerve to a sound. Otoacoustic emissions test records the echo of the sound given out via the speakers into the ear, wherein the absence of the echo confirms hearing loss.
Initial Steps towards Intervention
The first step towards the intervention program is to provide the suitable amplification for the child diagnosed with hearing loss using a hearing aid or cochlear implant. The goal of the intervention program should be to help the child to learn to communicate, maximize the use of residual hearing and interact with the society. Everyone in the family and immediate surroundings of the child becomes a contributor in the intervention program.
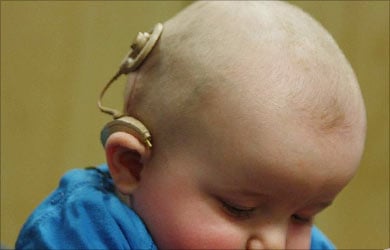
The team of professionals in the intervention program includes Otolaryngologist, Audiologist, Speech and Language therapist, primary care physician and psychologist if required. They can help in deciding whether the child can be helped to develop verbal language skills, use of sign language or any other means of communication. This decision is based on the overall cognitive skills, physical ability and intelligence of the hearing impaired child.
Auditory Training after Amplification
Children or adults with severe or profound hearing loss may still be able to hear some low frequency sounds and this hearing ability in them is called residual hearing. It is very important to preserve and use this residual hearing in the intervention program. Amplification with hearing aid or cochlear implant will help the child hear the sounds while the Auditory training sessions will help the child differentiate, discriminate and identify the sounds he or she hears. The auditory training can be extended to speech sound discrimination and identification, ultimately helping the child to improve on verbal communication skills.
Critical Period of Language Learning
A child with normal hearing learns to use verbal communication and spoken language during the critical period for language development, before two years of age. During this development, almost 80 percent of first language is learnt by the child, building up the vocabulary thereafter. Studies have shown that if this period is missed for language learning, the language development may not be as natural. Early identification of hearing impairment makes it possible to use this critical period to the maximum extent.

Professionals in the Intervention Program
Otolaryngologist: The ENT specialist determines the requirement of cochlear implant based on the residual hearing of the child. If the child is a suitable candidate, the implant is surgically placed.
Audiologist: An audiologist is typically responsible for fitting the right hearing aid, dispensing and management of a hearing aid. He or she can also advice the best use of residual hearing using this newly acquired amplification, to improve communication skills.
Speech and Language Therapist: A Speech and Language therapist focuses on developing the use and control of voice, vocabulary, comprehensive skills, expressive language skills, pronunciation of words and sounds, use of language in conversation and more. Developing reading comprehension and written language is also included. A number of non-verbal means of communication like sign language, lip reading and use of appropriate gestures is also taught to the child.
Teachers: The teachers at school for the hearing impaired can follow the schedule of the speech and language development program under the guidance of a speech and language therapist. This will help the child to use the skills learnt during the therapy sessions. If the child is attending a regular school, the teachers can make special arrangements to accommodate the hearing impaired child, to facilitate comprehension through lip reading and other non-verbal signs.
Primary caregivers: Parents or primary caregivers are the most important people in the intervention program for a child with hearing impairment. The sessions with the therapist and audiologist need to be followed on a regular basis and incorporated into the daily routine of the child. The siblings and friends of the hearing impaired child also contribute in their own way.

Integrating the hearing impaired child into the world full of sounds and verbal and written language is the ultimate goal of the intervention program. Earlier the start of the program, the better is the result. Hearing impairment is often a silent and hidden impediment. Early intervention and effective treatment can restore the child’s confidence and self esteem by enhancing social, cognitive and behavioral skills.