- Diabetes insipidus - (http://www.nlm.nih.gov/medlineplus/ency/article/000377.htm)
- About Diabetes insipidus - (http://www.mayoclinic.org/diseases-conditions/diabetes-insipidus/basics/definition/con-20026841)
- DIABETES INSIPIDUS, NEPHROGENIC, AUTOSOMAL - (http://www.omim.org/entry/125800)
- Neurology and Neurosurgery - (http://www.hopkinsmedicine.org/neurology_neurosurgery/centers_clinics/pituitary_center/conditions/diabetes-insipidus.html)
- DIABETES INSIPIDUS, NEUROHYPOPHYSEAL - (http://www.omim.org/entry/125700)
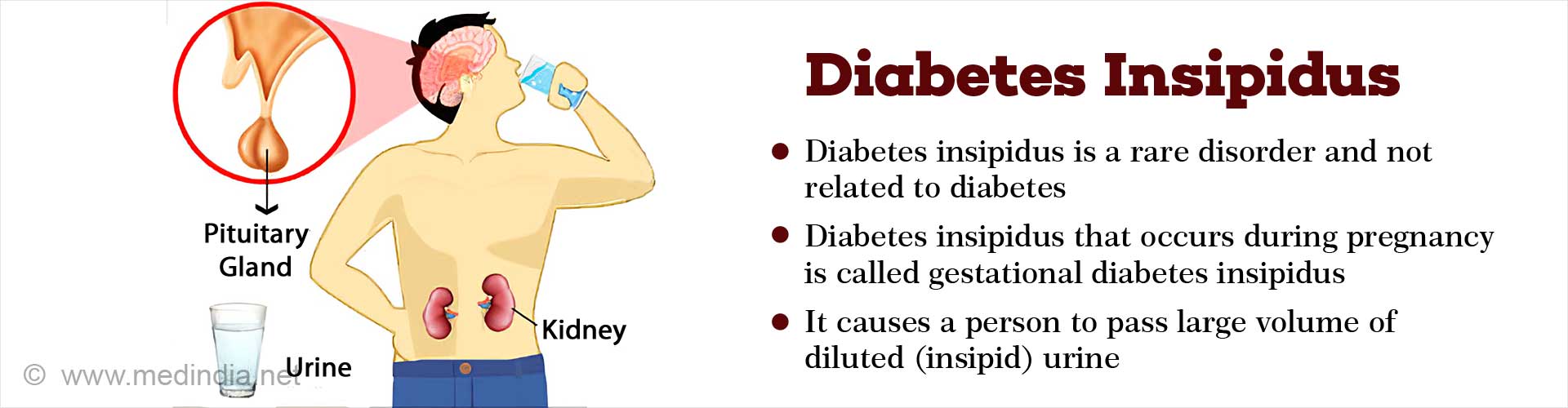
What is Diabetes Insipidus?
Diabetes insipidus (DI) is a rare condition where the kidneys cannot retain the appropriate quantity of water. This occurs due to insufficient production of the antidiuretic hormone (ADH) or arginine vasopressin (AVP/ vasopressin).
The ADH is produced in the hypothalamus and released by the pituitary gland, a small gland at the base of the brain that releases several other hormones as well. The condition affects individuals of all age groups.
Our kidneys play an important function in regulating pour daily fluid and salt balance. Normally, the kidneys first allows excess water to get filtered through it but most of this is reabsorbed back into the system with the regulation of antidiuretic hormone. This hormone enables the body to release urine with the right concentration depending on its fluid requirement. For example if we drink a lot of fluids more dilute urine is produced; whereas if we drink less more concentrated urine is formed. However, in the absence of ADH, the kidneys are unable to reabsorb the waterand a large volume of diluted (insipid) urine is excreted.
What are the Types & Causes of Diabetes Insipidus?
Diabetes insipidus is distinct from diabetes mellitus (simply referred to as diabetes) although certain symptoms like excessive thirst and frequent urination are similar among both the condition. There are 4 forms of diabetes insipidus, each having a different cause:
- Central
- Nephrogenic
- Dipsogenic
- Gestational

Central Diabetes Insipidus
Central diabetes insipidus is a condition that manifests due to damage to the hypothalamus or pituitary gland which then hampers the normal production, storage, and release of adequate quantities of ADH. The condition can also be inherited due to the defect in the vasopressin - producing gene, as seen in familial neurohypophyseal diabetes insipidus.
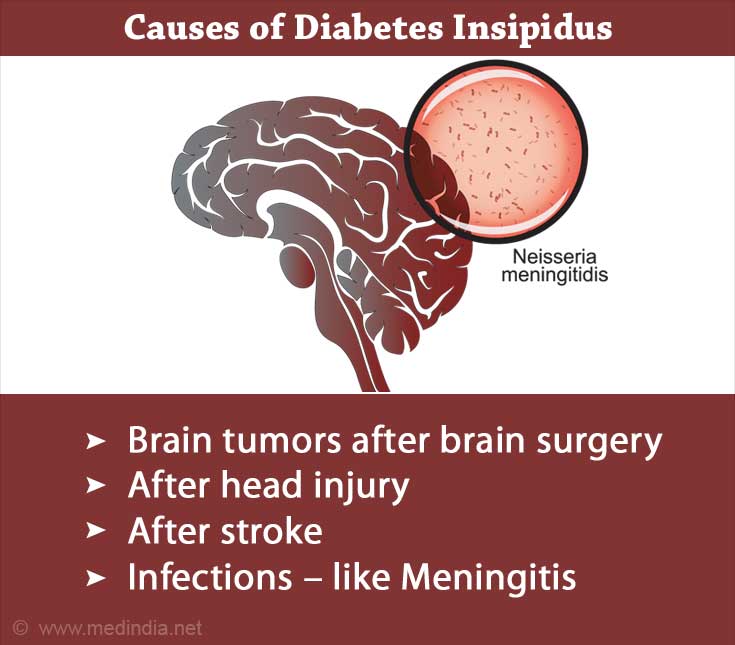
Other causes of central diabetes insipidus are:
- Brain tumors
- Brain surgery
- Head injury
- Infections (e.g., meningitis, encephalitis)
- Stroke affecting the blood supply to the hypothalamus or the pituitary gland
- Inflammatory conditions affecting the brain like meningitis and others like sarcoidosis, systemic lupus erythematosus, and so on
Nephrogenic Diabetes Insipidus
Nephrogenic diabetes insipidus is when the kidneys are incapable of reabsorbing water despite the presence of the Vasopressin hormone.
It occurs due to inherited defects in a gene, or mutations that allow the kidneys to become unresponsive to vasopressin. This, in turn, enables the excessive removal of fluid from a person's bloodstream. Other acquired causes of nephrogenic diabetes insipidus include:
- Kidney disorders like chronic kidney disease & polycystic kidney disease
- Formation of inflammatory granulomas in the kidney e.g. sarcoidosis
- Imbalances in blood electrolytes level like excess quantities of calcium (hypercalcemia) or low levels of potassium (hypokalemia)
- Blockage of the urinary tract
- Certain medications like lithium, ofloxacin, demeclocyline, aminoglycosides and a few others
Dipsogenic Diabetes Insipidus
Similar to central diabetes insipidus, the cause of dipsogenic diabetes insipidus is located in the higher centers of the thirst mechanism, in the hypothalamus. Any damage to the thirst mechanism adds to the reduced vasopressin secretion and increased urine output.
Some of the mental health problems and medications might also predispose a person to dipsogenic diabetes insipidus.
Gestational Diabetes Insipidus
Diabetes insipidus that occurs during pregnancy is called gestational diabetes insipidus. During pregnancy, the placenta (a temporary connecting organ between the mother and baby) produces an enzyme that breaks down the mother's vasopressin and contributes to the condition.
Other causes like increased prostaglandin in pregnancy, a hormone-like chemical that reduces kidney sensitivity to vasopressin contribute to gestational diabetes insipidus. The condition gradually disappears after the pregnancy.
What are the Symptoms of Diabetes Insipidus?
The main symptoms of diabetes insipidus are as follows:
- Increased thirst and craving for iced water (polydipsia) – An individual can drink between 2 to 20 L of water a day
- Increased frequency of urination (polyuria), with the production of large volumes of urine
- Dehydration symptoms due to loss of electrolytes like dry mouth, low blood pressure, fatigue, and muscle pains
- Changes in mental state, lethargy, and seizures observed in infants and the elderly

How do you Diagnosis Diabetes Insipidus?
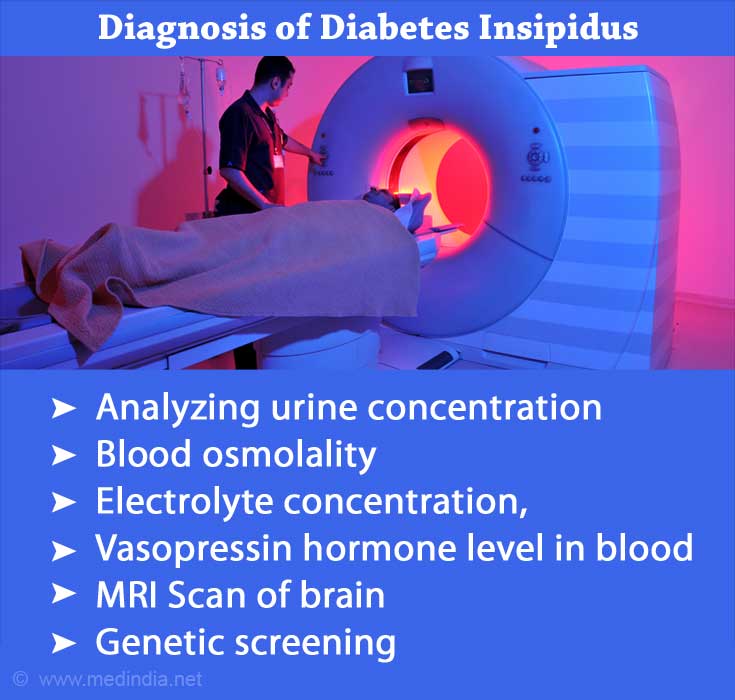
Diabetes insipidus may be diagnosed in the following ways:
- Urine- Analyzing the concentration of the urine, urine output via urinalysis
- Blood-
- Testing the blood for osmolality of the plasma,
- Electrolyte concentration,
- Levels of blood glucose,
- Levels of plasma ADH or AVP hormone
- Fluid deprivation test- restricting the intake of water to indicate the cause of excess urination
- Brain imaging- techniques like MRI and fMRI
- Functional Magnetic Resonance Imaging (fMRI) is a non-invasive technique used to obtain brain activity by detecting changes in the blood flow of the pituitary gland and brain. This aids in the diagnosis of Diabetes insipidus.
- Genetic screening
It is difficult to diagnose diabetes insipidus in children. The neurophysiological changes in children are monitored regularly with MRI. In children with nephrogenic diabetes insipidus, the electrolyte concentrations are measured.
How can you Treat Diabetes Insipidus?
- Treatment for diabetes insipidus differs based on the severity of the condition. Consuming adequate quantities of water may treat mild diabetes insipidus and prevent dehydration.
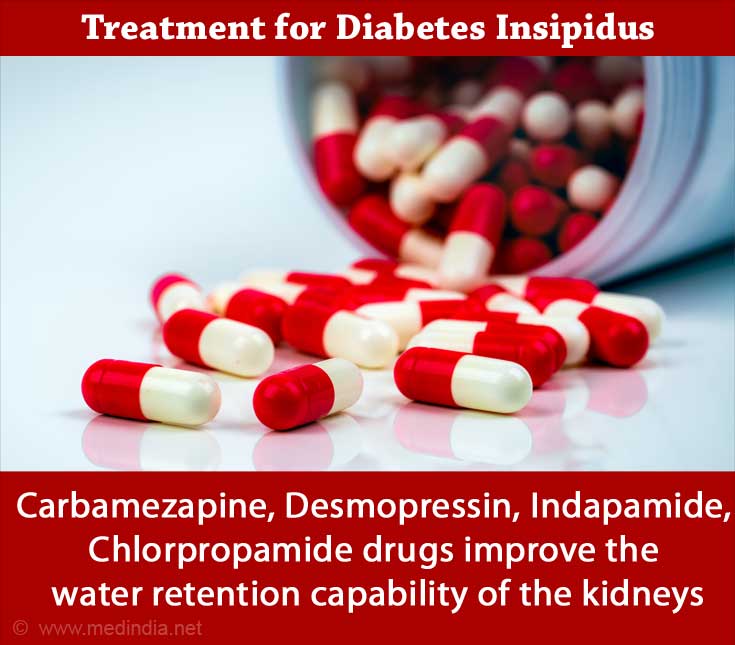
- The drugs used to treat central diabetes insipidus, include desmopressin, indapamide, carbamazepine, chlorpropamide, among others. These drugs improve the water retention capability of the kidneys.
- Children are favorably treated with vasopressin or desmopressin (the synthetic analog of vasopressin).
- Maintaining the sodium levels in the body, and thus, the water content in the body, are ways to treat nephrogenic diabetes.
- Nonsteroidal anti-inflammatory drugs are also used for the treatment. Indomethacin and chlorothiazide areused to treat children with nephrogenic diabetes insipidus.
- Other therapeutic strategies to treat patients with nephrogenic diabetes insipidus arebeing investigated. These include the use of phosphodiesterase (PDE) inhibitors, statins, heat shock proteins (HSP90), and prostaglandins.
- Regular monitoring of the patient during treatment should be carried out by which one can identify water intoxication and electrolyte imbalance.
What are the Complication of Diabetes Insipidus?
Dehydration is the main complication of diabetes insipidus that occurs due to an imbalance between fluid loss and intake.
It is thereby important to look for warning symptoms of dehydration like sluggishness, dizziness, confusion, seizures, that may later result in permanent brain damage and even death.