- Botek G, Anderson MA, Taylor R. Charcot neuroarthropathy: An often overlooked complication of diabetes. Cleveland Clinic Journal of Medicine 2010; 77(9):593-99.
- Robert A. Slater DPM, Yoram Ramot MD, Andreas Buchs MD and Micha J. Rapoport MD. The Diabetic Charcot Foot. IMAJ 2004;6:280-283
- Sommer TC, Lee TH. Charcot Foot: The Diagnostic Dilemma. Am Fam Physician 2001;64:1591-8.
- Caputo GM, Jan U, Cavanagh PR, Juliano P. The Charcot Foot in Diabetes: Six Key Points. Am Fam Physician. 1998;57(11):2705-2710.
About
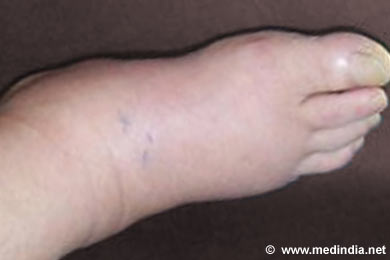
Charcot foot is a condition characterized by progressive deterioration of a weight-bearing joint of the foot. It results in significant destruction of the bony architecture of the foot, resulting in fractures and deformities. It is also known as diabetic neuropathic osteoarthropathy or neuropathic arthropathy. It can progress rapidly without treatment and results in ulcers, deformity and may even require amputation in some cases.
The condition was described by Charcot in 1868 in a patient with syphilis. However, the most common cause of Charcot foot is diabetes. Its incidence is as high as 13% in high-risk diabetes patients. Most of these patients have a poor control of their diabetes.
Charcot foot develops due to loss of sensation in the foot. Diseases affecting the nerves like diabetes make a person insensitive to trauma, i.e., even if the person hits something with his foot, he is unable to feel the pain and tends to ignore the wound. Repeated trauma could thus result in Charcot foot. Another theory suggests that changes in the blood vessels could contribute to the development of Charcot foot.
Other conditions that affect peripheral nerves can also cause neuropathic arthropathy. These include leprosy, syringomyelia (a condition that affects the spinal cord), exposure to toxic substances, polio, multiple sclerosis, injury and advanced syphilis. In the earlier days when syphilis was common, the disease often affected the knee. Syringomyelia was commonly associated with disease of the shoulder.
Conditions that trigger the development of Charcot fool include infection of the subcutaneous tissues, bones or synovium (tissues lining joints), foot surgery and kidney transplant surgery.
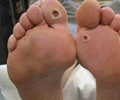
Acute symptoms usually include increase in warmth, swelling and redness of the foot. Pain is usually disproportionately less as compared to the degree of damage. Long-term Charcot foot results in deformities of the foot and repeated ulceration.
Charcot foot is usually diagnosed based on history and clinical examination of the patient. Radiological tests are useful in diagnosing the condition as well as monitoring response to treatment.
Acute symptoms of Charcot foot are treated with immobilization, followed by use of custom-made shoes to prevent repeated ulceration. Deformities are sometimes treated with surgery.