- Acute Kidney Injury: Definition, Pathophysiology and Clinical Phenotypes - (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5198510/)
- Acute Kidney Injury - Overview - (https://en.wikipedia.org/wiki/Acute_kidney_injury)
- About Acute Kidney Injury (AKI) - (https://www.kidney.org/atoz/content/AcuteKidneyInjury)
- Acute Kidney Failure - (https://www.healthline.com/health/acute-kidney-failure#symptoms)
- What is Acute Kidney Injury - (https://www.kidneyfund.org/kidney-disease/kidney-problems/acute-kidney-injury.html)
- Renal Function Tests - (https://www.ncbi.nlm.nih.gov/books/NBK507821/)
- Renal Recovery after Acute Kidney Injury - (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5487594/)
What is Acute Renal Failure?
"The kidneys are so beautifully organized; they do their work of regulation with such a positively divine precision, such knowledge and wisdom, that there is no reason why our archetypal man, whoever he is, or any one else, for that matter, should be ashamed to own a pair." ---Aldus Huxley "Antic Hay"
Acute Renal Failure (ARF) is, simply put, a sudden loss of or decline in kidney function. It occurs when the kidneys stop working over a period of hours, days, or in some cases, weeks. The term Acute Kidney Injury (AKI) is preferred and used synonymously with acute renal failure.(1✔ ✔Trusted Source
Acute Kidney Injury: Definition, Pathophysiology and Clinical Phenotypes
Go to source)
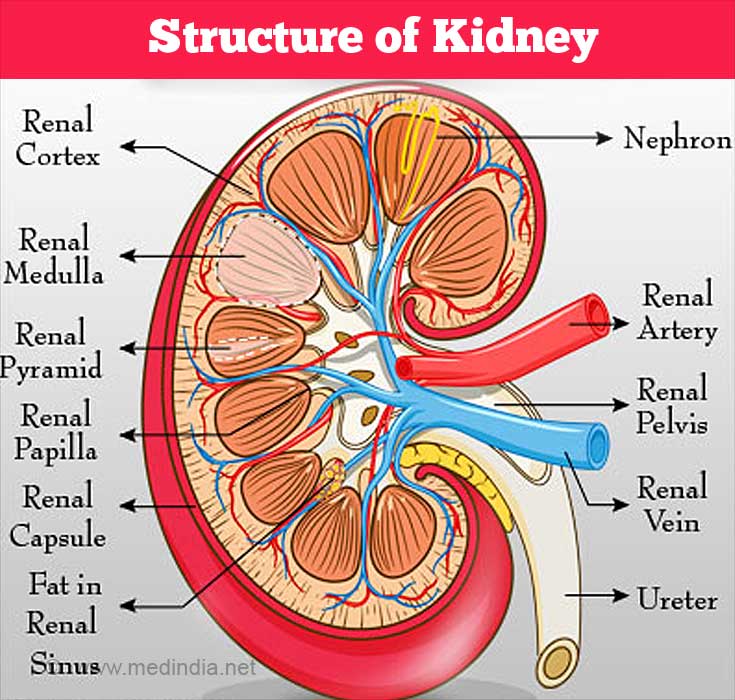
The bean shaped organs, called kidneys need to be 'full of beans' to carry out the crucial task of filtering body waste and maintaining electrolyte levels in the blood. Malfunction of the kidneys could lead to accumulation of waste products, fluids and electrolytes in the body, which could gravely endanger life.
Acute Renal Failure is diagnosed clinically by a sharp increase of the serum creatinine level from baseline (i.e., an increase of at least 0.5 mg/dl) and/or if the urine output is less than 400 ml per day (oliguria), though not strictly applicable for ARF.
Acute Renal Failure complicates about 5-7% of all hospital admissions. The presence of ARF in hospitalized patients also significantly increases the risk of mortality in these patients. The prognosis may be bleak if ARF is accompanied with complicated medical conditions or surgical conditions.
”Acute Renal Failure (ARF) and Chronic Kidney Disease (CKD) – Are They Different?”
The answer is ‘yes’. The most important way in which ARF is different from Chronic Kidney Disease is that ARF is reversible if early diagnosis and treatment take place whereas in CKD there is a permanent loss of kidney function.
Acute Renal Failure is often the consequence of any untoward experience the body is subjected to; for instance – blood loss due to surgery, or medicine overdose or any injury to the body.
Chronic kidney disease (CKD) is often the consequence of long-term illness like high blood pressure or diabetes which gradually takes a toll on the kidneys, causing them to malfunction.
Who are Affected by Acute Renal Failure?
Acute Renal Failure (ARF) occurs most often in people who are already hospitalized for other medical conditions.
ARF develops from 5% to 7% of all patients in the hospital. Of those hospitalized in intensive or critical care units, up to 30% develop ARF. Factors that increase a person's risk of Acute Renal Failure include advanced age, chronic renal insufficiency, liver disease, diabetes, high blood pressure, heart failure, and obesity.
People undergoing heart surgery and abdominal surgery also have an increased risk. ARF can also occur in normal healthy people who indiscriminately use pain-killers, specifically, NSAIDs and some other prescription medicines and alternative therapies.
Types of Acute Renal Failure
Acute renal failure can be divided into three categories:
- Acute renal failure characterized by diminished renal blood flow; Pre-renal (60 to 70 percent of cases)
- Acute renal failure, due to damage to the renal tissue; Renal (25 to 40 percent of cases)
- Acute renal failure because of urinary tract obstruction; Post-renal (5 to 10 percent of cases)
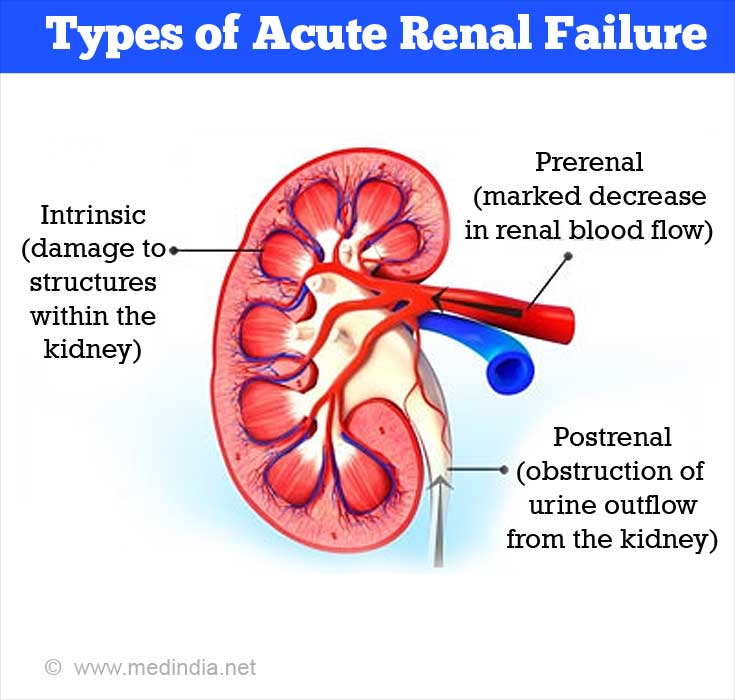
Pre-Renal Causes (not related to kidney per se):
- Systemic conditions like heart failure, blood or fluid loss
- Local causes renal artery narrowing, diseases of arteries
Renal Causes:
- Acute tubular necrosis - 85% /toxic/septic renal failure
- Glomerular disease - 5% (primary in systemic diseases)
- Other diseases of Kidney – (Drug induced) 10%
Post-renal Causes (due to blocked flow of urine from kidney)
Urinary tract obstruction like in tumors, stones, inflammation within the urinary tract like both ureters or bladder or an enlarged prostate gland.(2✔ ✔Trusted Source
Acute Kidney Injury - Overview
Go to source)
What are the Causes of Acute Renal Failure?
- When ARF occurs, waste products, such as nitrogen or salt, and excess fluids are not removed by the kidneys and builds up in the body, upsetting the body's normal chemical balance.
- Chemicals and electrolytes, such as sodium, potassium, and calcium, which are needed for normal body functioning, become harmful or sometimes poisonous (toxic) to the body when they reach abnormally high or low levels.(3✔ ✔Trusted Source
About Acute Kidney Injury (AKI)
Go to source)
What are the Symptoms of Acute Renal Failure?
Symptoms of Acute Renal Failure depend on the cause of the problem. Acute Renal Failure cannot be diagnosed exclusively based on the following symptoms. Symptoms may include:
- Swelling of the hands, face, or feet
- Decreased urinary output (oliguria)
- Shortness of breath (dyspnea)
- Rapid, irregular heart rate
- Enlarged or distended neck veins
- Nausea, vomiting, and loss of appetite. Profound weakness or fatigue. Confusion, agitation, or combative behavior(4✔ ✔Trusted Source
Acute Kidney Failure
Go to source, 5✔ ✔Trusted Source
What is Acute Kidney Injury
Go to source)

What are the Complications of Acute Renal Failure?
- The complications of Acute Renal Failure (ARF) can affect the entire body, including the digestive system, heart, lungs, and nervous system.
- Infection is one of the most common complications of ARF, because the body's immune system may stop working properly.
- Uremic syndrome (uremia) is a serious complication of severe or prolonged Acute Renal Failure. It can cause severe nausea, confusion, psychosis, irregular heartbeats, and pulmonary edema pulmonary edema (fluid in lungs).
- Increased potassium in the blood - due to inability to filter and excrete the electrolytes properly.
How is Acute Renal Failure Diagnosed?
Acute Renal Failure is usually diagnosed using blood and urine tests to monitor kidney function. Tests may include:
- Blood urea nitrogen (BUN),
- Serum creatinine,
- Complete blood count (CBC),
- And an Urinalysis.

A chemistry screen may be used to look for abnormalities in electrolytes, such as sodium, potassium, bicarbonate and calcium. Sometimes a kidney biopsy may be required to diagnose the cause of renal failure.(6✔ ✔Trusted Source
Renal Function Tests
Go to source)
How do you Treat Acute Renal Failure?
- The treatment of Acute Renal Failure depends on the cause and may include:
- Correcting the underlying cause of kidney failure, such as dehydration or medication toxicity.
- Providing supportive care for the kidneys through dialysis.

- Preventing other complications, such as infection or fluid or electrolyte imbalances.
What is the Prognosis of Acute Renal Failure?
Acute Renal Failure (ARF) can usually be reversed, but it can also cause permanent loss of kidney function leading to Chronic Kidney Disease (CKD). Older adults and people who have other serious medical conditions are less likely to recover from ARF and its complications. Patients who have been treated for ARF and recovered need to be followed up to prevent onset of chronic kidney disease.
In some cases, the Acute Renal Failure (ARF) causes severe damage to the kidney wherein a transplant may be required. This condition is termed as End Stage Renal Disease (ESRD).
What is Recovery from Acute Renal Failure Like?
Kidney function may quickly return to normal if the cause of Acute Renal Failure (ARF) is diagnosed and corrected. ARF may be corrected within a few days, or it may last for more than a month. Chances of recovery from ARF depend on many factors, including what caused the ARF, how severe and prolonged it was, how quickly the problem was recognized and treated, and what other medical conditions the person has.
Acute Renal Failure caused by dehydration, blood loss, or obstruction in the urinary system is rapidly reversed. About 50% of people who develop ARF recover completely. Some may have only partial recovery and others may require long term dialysis.(7✔ ✔Trusted Source
Renal Recovery after Acute Kidney Injury
Go to source)