Obstructive Sleep Apnea - Overview
Obstructive Sleep Apnea was called the 'Pickwickian syndrome' in the past because Joe, the fat boy, described in 'The Pickwick Papers' by Charles Dickens, had typical features such as snoring, obesity, sleepiness and dropsy.
Obstructive Sleep Apnea (OSA) is a sleep- related breathing disorder in which there is repeated obstruction to the upper airway, while the person is sleeping.
'Apnea', which means 'without breath' in Greek, causes its victims to repeatedly stop breathing during their sleep, often for 10 seconds or more and sometimes even for a minute or longer. These episodes of breathing interruptions are dangerous and lead to a drop in the oxygen saturation in the blood. The obstructive episode frequency can be as high as 30 times an hour. Sleep apnea can be caused by either a complete obstruction of the airway (obstructive apnea) or a partial obstruction (Obstructive Hypopnea), both of which can wake a person from sleep to facilitate breathing.
A drop in the oxygen saturation can harm both the heart and the brain and can be dangerous to a person's health. The process of obstruction can lead to poor quality of sleep, waking up in the night and increased sleepiness during the day and at work. This negatively impacts the quality of life. Besides this, snoring can keep the partner awake.
Types of Sleep Apnea
Obstructed Sleep Apnea (OSA):
The airway becomes either completely or partially blocked in this kind of sleep apnea, which is typically caused by the relaxation of the throat muscles. As a result, the body's oxygen levels drop, which might cause the brain to wake the person up to resume breathing.
Central Sleep Apnea (CSA):
This kind of sleep apnea develops when the brain fails to communicate properly with the muscles that coordinate breathing, resulting in breathing pauses.
Complex sleep apnea syndrome (CompSA):
CompSA is also known as treatment-emergent Central Sleep Apnea, this is a combination of OSA and CSA, where the airway is blocked but the brain is not sending the appropriate signals to resume breathing.
Obstructive Sleep Apnea - Incidence
According to population-based studies, symptomatic obstructive sleep apnea appears to affect people over 50 years old. Nearly 2 percent of women and 4 percent of men are known to complain of this condition. Asymptomatic Sleep Apnea is more common than symptomatic obstructive sleep apnea.
Among habitual loud snorers, the incidence of obstructive sleep apnea (OSA) is about 17% in men and 15% in women.
Some researchers have noticed an increased incidence of OSA in people of Asian origin.
Mechanism of Obstructive Sleep Apnea (OSA)
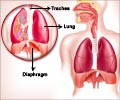
Obstructive Sleep Apnea is caused by repetitive upper airway obstruction during sleep as a result of narrowing of the breathing passages.
When a person is awake the airway muscle tone helps to keep the airways open. Decreased airway muscle tone during sleep, and the pull of gravity in the supine position, result in some prolapse of the airway structures and further decrease their size. This can impede airflow during respiration. Snoring can occur during the initial stages, caused by a partial obstruction in the airway. As tissues collapse further or the patient rolls over on his or her back, the airway may become completely obstructed.
When the nature of the obstruction is partial it is termed hypopnea, whereas, a complete obstruction in the airway is called Apnea. Both hypopnea and apnea cause disruption in victims’ sleep several times during the night, though the disturbance may go unrecognized by patients. Obstructive episodes are often associated with a reduction in blood oxygen levels.
Consequences of Airway Obstruction
The reduction in blood oxygen levels in the blood circulation can be dangerous for both the heart and the brain. Both of these organs require much more oxygen for their normal function than other organs. Obstruction is like strangulating a person repeatedly and depriving them of their constant oxygen supply to the body.
This repeated obstruction in obstructive sleep apnea causes what is called an autonomic stress.
The autonomic nervous system of the body consists of two systems called the sympathetic and the parasympathetic systems. These are systems that we are not normally aware of and these regulate the key functions of the body including the activity of the heart muscle, endocrinal glands, digestion, and the smooth muscle tone (e.g., the muscles of the walls of the blood vessels).
Lack of oxygen plays havoc with the autonomic system and its functioning. The first organs to suffer include the heart and the brain.
Consequence of Obstructive Sleep Apnea on the Heart
Irregularity in the Rhythm of the heart called Cardiac dysrhythmias can be observed in OSA patients
Cyclical variations in blood pressure changes can elevate both pressure in the lung vessels (called pulmonary hypertension) and also increase the normal blood pressure of the rest of the body (called systemic hypertension).
Symptoms and Signs of Obstructive Sleep Apnea
Due to the obstruction of the airways during sleep the patient has snoring and apneic episodes that end as choking and gasping in sleep. Repeated apneic episodes with arousals lead to a disturbed sleep.
These cycles are characterized by repeated wake-up and sleep states, caused due to obstruction and disturbance in breathing. In very acute cases, patients could suffer upper airway obstruction about a hundred times in one hour.
Symptoms of obstructive sleep apnea are:
- Excessive sleepiness - As the person suffering from sleep apnea does not get the required amount of sleep they suffer from 'excessive sleepiness' and this usually is manifested as daytime sleepiness.
- Snoring - Partial obstruction to the airway can cause some resistance to airflow, resulting in snoring.
- Apneic episodes - Episodes of temporary cessation of breathing occurs in the patient, which is initially noticed by the partner.
- Choking or gasping in sleep - At the end of an 'apneic episode' the patient chokes or gasps in an effort to take a breath.
- Tiredness upon awakening - Episodes of apnea can cause repeated arousals from sleep that will lead to sleep fragmentation. This causes fatigue upon awakening.
- Headache - Sleep apnea headaches are different from certain other forms of headaches since they are not associated with nausea or sensitivity to light and sound.
This can cause cognitive difficulties leading to motor vehicle crashes, work-place accidents, impaired performance at work or school, social embarrassment, depression and compromised quality of life.
Diagnosis of Obstructive Sleep Apnea
An Objective testing method is employed to make an initial diagnosis of some patients who complain of snoring and excessive daytime sleepiness.
The
Nocturnal polysomnography is considered the best evaluation tool for diagnosing obstructive sleep apnea. This tool helps in assessing the patient in a sleep laboratory by applying several physiological parameters while the patient is asleep.
Apneic events can then be documented based on chest wall movement with no air flow and low oxygen levels in the blood (measured by oxyhemoglobin desaturations).
A respiratory disturbance index (RDI) is then calculated and expressed as the number of abnormal respiratory events per hour of sleep. The cut-off point adopted by a few sleep laboratories, in the case of continuous positive airway pressure, is a RDI of 20 episodes per hour.
A multiple sleep latency test (MSLT) measures the extent of daytime sleepiness. The time required by an average adult to fall asleep during the day is 10 minutes; therefore it is considered abnormal if the mean sleep latency is below 5 minutes.
Treatment of Obstructive Sleep Apnea
Treatment focuses on rectifying nighttime breathing in order to positively impact the problems of loud snoring and daytime sleepiness. This will also cut the risks of associated medical conditions like high blood pressure, heart attack, and stroke.
Treatment for Obstructive Sleep Apnea also helps patients maintain an appropriate weight. Obese victims of OSA find immense relief with weight loss. Even a modest 10 percent weight loss may eliminate apneic episodes by reducing the fat deposition around the airway and increasing the size of the airway. However, this treatment option is usually not very successful because only a small fraction of people can lose weight and maintain it.
1. Positional therapy
Positional therapy is based on beating the effects of gravity on the airways when lying flat on the bed.
Most people with sleep apnea have bad symptoms if they lie flat on their back during sleep and this is due to gravity enhancing the airway collapse. There are several strategies that can help patients who have mild apnea only when lying on their backs.
Sew or attach socks filled with tennis balls, lengthwise down the back of their pyjama top or nightshirt. This ensures that the victim lies on the back. Additionally, positional pillows can be employed to help the victim sleep on the side rather than the back. Positional therapy has its own limits, and is found to benefit a few patients.
2. Positive Pressure Therapy
Positive airway pressure is very effective in treating obstructive sleep apnea, involving three strategies - continuous positive airway pressure (CPAP), auto titration, and bi-level airway pressure.
CPAP, is by far the most popular therapy to treat sleep apnea. It is administered with the help of a facial or nasal mask that is attached to a tiny air compressor. Administered at bedtime, this apparatus conveys air with a slight pressure through the tube and into the mask. The apparatus ensures that the upper airway does not close, which helps prevent apnea. A polysomnogram is used to determine each patient’s optimum airway pressure.
Conclusion
Obstructive sleep apnea is a health hazard and usually affects middle-aged, overweight adults. It causes not only snoring but also repeated obstructions to breathing while the person is sleeping. This leads to a drop in oxygen saturation within the blood which can damage organs such as the heart and the brain.
The condition can be diagnosed with a visit to the sleep lab, which conducts a simple test called a polysomnogram. Simple advice can treat patients with mild sleep apnea; however a more advanced condition may require the use of equipment like CPAP. Treatment improves a person’s overall health by improving the quality of sleep.
Regular and ongoing follow up is needed with a sleep medicine specialist who will check whether the treatment is working and whether there are any side effects of the treatment.