Diagnosis
For a diagnosis of Multiple sclerosis, one must have the following: a typical history, evidence of lesions or ‘sclerosis’ in at least two areas of the brain or spine or optic nerve by MRI which have occurred at least a month apart, and a raised protein level in the spinal fluid.
- The characteristic history of relapse followed by remission is suggestive
- Neurological examination to locate the affected area
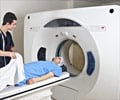
- MRI scan is very helpful in picking up the areas scarred and showing ‘sclerosis’. An MRI with a gadolinium contrast can pick up lesions which are active or less than 2 months old.
- Lumbar puncture The proteins in the cerebro-spinal fluid will be raised and be seen as an oligoclonal band.
- A visual evoked potential will reveal slowing of transmission of impulses caused by damage to the optic nerve
The disease can be confused with some other conditions that affect the brain and spinal cord, including Vitamin B12 deficiency, some inflammatory conditions like syphilis, Lyme disease, sarcoidosis and systemic lupus erythematosus or SLE. Tumor of the brain or spinal cord and cervical spondylosis can also mimic some of the features of MS.
Hughes Syndrome (also known as Sticky Blood Syndrome) was first discovered by Dr. Graham Hughes in 1983. In this condition the blood clots easily and causes Thrombosis or Strokes. The symptoms of Hughes Syndrome can be similar to MS. Depending on the area affected a patient can have
- Foot drop
- Difficulty with walking
- Double-vision
- Slurred speech
- And loss of balance.
The condition can be easily treated using Aspirin, Heparin or Warfarin. Sometimes the condition if not recognized can be fatal. It is estimated that almost 33% of the patients diagnosed with MS may actually have Hughes Syndrome.